MATERIALS,
METHODS AND RESULTS:
We retrospectively reviewed cases of intraspinal tumours treated at our institution from January 2008 to December 2011 (n = 67; 36 women,
31 men,
median age at diagnosis 53 years [range 18-83]).
In this period,
344 craniospinal tumours were treated in our centre,
thus representing a prevalence of 19% of intraspinal tumours (similar to published data).
We evaluated clinical data,
location,
histological type,
radiological features,
type of treatment,
and outcome.
Clinical symptoms were variable and determined by location and tumour size.
Pain was the most frequent clinical presentation (n=29),
associated in some cases with a motor deficit (n=12).
In 17 cases,
isolated motor deficit was the first clinical presentation and in 14 cases the tumour was an incidental finding with no valuable clinical data.
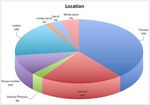
Location:
We classified intraspinal tumours by the area of the spine in which they occur: cervical (n=14; 20.9%),
cervico-thoracic (n=2; 3%),
thoracic (n=26; 38.8%),
thoraco-lumbar (n=7; 10.4%), lumbar (n=12; 17.9%),
lumbo-sacral (n=1; 1.5%),
sacral (n=2; 3%),
and whole-spine (n=3; 4.5%).
(Fig. 2)
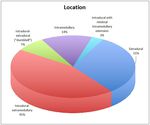
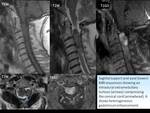
Additionally,
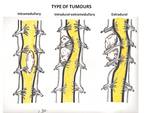
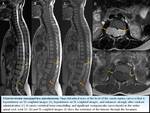
we classified them by their anatomic relations with vertebrae,
dural sac,
and spinal cord: (Fig. 3)
1,
2: Extradural (n= 21; 31%)
3: Intradural extramedullary (n=30; 45%)
4: Intradural-extradural (dumbbell) (n=5; 7%)
5: Intramedullary (n=9; 14%)
6: Intradural extramedullary with minimal intramedullary extension (n=2; 3%)
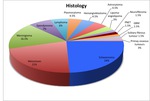
The most frequent histological type was schwannoma (n=16; 24%),
followed by metastases (n=14; 21%) and meningioma (n=11; 16.5%). Other,
less frequent tumours were: ependymoma (n=5; 7%),
lymphoma (n=4; 6 %),
plasmocytoma (n=3; 4.5%),
hemangioblastoma (n=3; 4.5%),
astrocytoma (n=3; 4.5%),
lipoma-angiolipoma (n=2; 3%),
primary osseous tumours [chordoma (n=1;1.5%), hemangioma (n=1;1.5%)],
neurofibroma (n=1; 1.5%),
primitive neuroectodermal tumour-PNET (n=1; 1.5%),
glioblastoma multiforme (n=1; 1.5%),
and solitary fibrous tumour (n=1; 1.5%).
(Fig. 4)
Radiological findings:
In 19 patients,
MRI was not available for evaluation; therefore,
these cases were excluded from the analysis.
The 48 remaining cases were analysed:
- On T1-weighted TSE sequences,
23 lesions were isointense (48%),
22 were hypointense (45.8%),
2 were hyperintense (4.2%),
and 1 had a heterogeneous mixed signal (2%).
- On T2-weighted TSE sequences,
most lesions were hyperintense (n=34,
70.8%),
7 were isointense (14.6%),
5 were hypointense (10.4%),
and 2 had a heterogeneous mixed signal (4.2%).
- STIR sequences were done in 38 patients: Most lesions were hyperintense (n=31,
81.6%),
4 were hypointense (10.5%),
one was isointense (2.6%),
and 2 had a heterogeneous mixed signal (5.2%).
- Gadolinium-enhanced sequences were obtained in 35 patients: 33 lesions showed contrast enhancement (enhancement was homogeneous in 20,
heterogeneous in 8,
and peripheral in 5) and two lesions did not enhance.
- Evidence of cord compression was present in 69% of cases,
and associated intramedullary lesions (oedema or syringomyelia) were present in 45%.
Treatment and outcome:
58 cases were treated with surgery (total or partial resection) and in 8 cases radiotherapy or chemotherapy was done.
One case was clinically observed without treatment.
48 patients showed clinical improvement after treatment; 10 achieved clinical stabilization,
and 9 worsened despite treatment (5 of these died).
CLINICAL CASES WITH RADIO-PATHOLOGIC CORRELATION:
EXTRADURAL LESIONS:
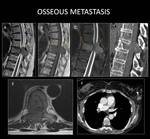
CASE 1: OSSEOUS METASTASES (Fig. 5)
67-year-old woman with recent chest pain associated with progressive loss of sensation and muscle weakness in the legs.
MRI and CT detected an isolated lytic lesion in a thoracic vertebra (T9) with an associated extradural soft-tissue mass in an anterior and posterior location that compressed the spinal cord.
Tumour extension studies detected a breast neoplasm.
She underwent T9 vertebrectomy with vertebral prosthesis and spinal fixation system.
Teaching points:
-Metastases are the most frequent extradural tumours.
-Solitary vertebral lesions are less frequent than tumours with multiple locations.
-Metastases are most frequent in the thoracic spine followed by the lumbar spine.
-The most common primary tumours giving rise to metastatic spinal tumours are lung,
breast,
and prostate tumours.
-Most lesions are osteolytic; osteoblastic metastases occur frequently with metastases from prostate and breast cancer.
-In elderly patients,
the differential diagnosis with plasmocytoma/myeloma must be done.
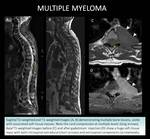
CASE 2: MULTIPLE MYELOMA (Fig. 6)
66-year-old man with a three-week history of low back muscular pain with lower limb paresthesias,
with pain increasing in the last 2 to 3 days despite treatment.
He was diagnosed with IgG-kappa multiple myeloma with multiple lesions in the spine,
ribs,
pelvis,
cranial vault,
and sternum.
Teaching points:
-Myeloma is the most frequent primary malignant tumour of the spine.
-The peak incidence is in the sixth to seventh decade.
-The spine and especially the vertebral bodies are the most common sites; epidural extension is common.
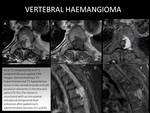
CASE 3: VERTEBRAL HAEMANGIOMA (Fig. 7; Fig. 8)
77-year-old man with chest pain. MRI detected an osseous vertebral lesion at T5-T6 with an epidural component that extends to the vertebral canal and foramina,
compressing the spinal cord and nerve roots.
Teaching points:
-Vertebral hemangioma is the most common benign spinal tumour.
-Most occur in the vertebral body and about 10% extend into the posterior elements.
-The thoracic region is the most frequent.
-There are two different types: 1- asymptomatic; 2-aggressive,
symptomatic types with intraspinal tumour extension and cord compression.
-Lesions with high T1 signal are considered benign.
Low signal on both T1- and T2-weighted sequences represents degenerative change/involution of the lesion.
Low T1 signal together with high T2 signal may represent an atypical hemangioma.
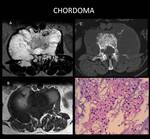
CASE 4: CHORDOMA (Fig. 9)
53-year-old man with a history of chronic low back pain radiating to the lower limbs,
associated with dysesthesia over the last 2 months.
MRI detected an osseous tumour at L2 that was diagnosed as a chordoma at histologic study.
He showed good clinical recovery after partial posterior vertebrectomy and postsurgical radiotherapy.
Teaching points:
-Chordomas are malignant tumours that arise from remnants of the notochord,
show local invasion,
and can produce distant metastases.
-Chordomas are destructive,
lytic (or mixed lytic/sclerotic) lesions with an associated mass.
-Amorphous calcification may be seen (50%-70% cases).
-On MRI,
most are isointense or hypointense on T1-weighted images and hyperintense on T2-weighted images compared to muscle.
The internal fibrous septa that divide the gelatinous components of the tumour have low signal intensity on T2-weighted images and are a characteristic feature.
-Half of these tumours are found in the sacrum,
35% in the clivus,
and the rest in the vertebrae.
-They are usually located along the midline.
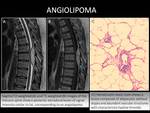
CASE 5: ANGIOLIPOMA (Fig. 10)
52-year-old woman with lower limb paraparesis.
A posterior intraspinal extradural mass,
corresponding to an angiolipoma,
was detected at T6-T7.
MRI showed signs of compressive myelopathy.
She showed good recovery after complete resection of the lesion.
Teaching points:
-Angiolipomas are common benign lesions that are almost always located subcutaneously.
However,
spinal angiolipoma is a specific but uncommon clinico-pathological entity that should be considered in the differential diagnosis of long-standing,
slowly progressive paraparesis.
-They are composed of varying proportions of mature fat cells and abnormal vascular elements.
The variability of the vascular and adipose elements of the tumor results in significant heterogeneity in imaging studies.
-Most are located in the thoracic region.
Almost all noninfiltrating epidural angiolipomas are posterior or posterolateral in location.
INTRADURAL-EXTRAMEDULLARY LESIONS
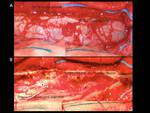
CASES 6 and 7: MENINGIOMA
Case 6: 51-year-old man presented with Brown-Séquard syndrome.
CT and MRI showed a well-delimited oval lesion with intense contrast enhancement in the intradural extramedullary space at the level of C1 causing compressive myelopathy (Fig. 11).
Outcome after complete resection of the lesion (see video- Fig. 12) was very good.
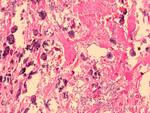
Histologic study diagnosed meningothelial meningioma (Fig. 13).
Case 7: 40-year-old man with a four-year history of progressive left back pain radiating to the waist and progressive gait disturbances (lower limb paraparesis without associated sensory deficit).
MRI detected an intradural extramedullary lesion compressing the thoracic spinal cord and causing secondary myelopathy (Fig. 14).
The lesion was excised (Fig. 15),
and histology diagnosed psammomatous meningioma (Fig. 16).
He developed paraplegia as a postsurgical complication.
Teaching points:
-Spinal meningiomas are the second most frequent intradural extramedullary tumor after nerve sheath tumours.
-They are slow-growing,
usually benign tumours.
-They are most frequent in thoracic region (80%),
followed by the cervical region (15%).
-They are usually located posterolateral in the thoracic region and anteriorly in the cervical region.
-Broad dural based.
A dural tail may be seen.
-They may be calcified.
-They enhance avidly and homogenously with contrast.
-Female predominance. They usually present after the fourth decade.
-Keep in mind that multiple meningiomas may be present in NF-2.
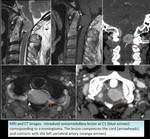
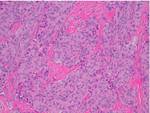
CASE 8: SOLITARY FIBROUS TUMOR
71-year-old man presenting with Brown-Sequard syndrome.
An intradural extramedullary lesion compressing the cervical cord was detected (Fig. 17).
Preoperative MRI suggested meningioma.
After laminectomy with tumor resection,
pathologic examination revealed a solitary fibrous tumour (Fig. 18).
The patient died of a postsurgical respiratory complication.
Teaching files:
-Solitary fibrous tumours are uncommon mesenchymal tumours that involve the pleural cavity and numerous extrathoracic sites,
including the prostate,
kidney,
thyroid,
and rarely the intraspinal compartment.
-This rare entity should be included in the differential diagnosis of intradural extramedullary spinal neoplasms.
CASES 9 and 10: FILUM TERMINALE EPENDYMOMA
Case 9: 21-year-old woman with low back pain,
impaired ambulation,
lower limb paresis,
and sphincter incontinence.
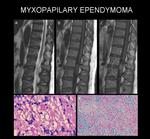
MRI detected a huge intradural lesion at the filum terminale and cauda equina (T12-L5),
producing bone remodeling and syringomyelia (Fig. 19).
Subtotal resection resulted in good outcome.
Pathologic examination ruled out a grade I myxopapillary ependymoma (Fig. 20).
Case 10: 54-year-old man with long-standing symptoms of sphincter incontinency,
hypoesthesia in the left L5-S1 territory,
and minimal lower limb motor deficit.
MRI detected an intradural extramedullary tumour at L1-L2 ( Fig. 21).
The lesion was excised (see intraoperative video- Fig. 22).
Pathologic examination of the specimen revealed a grade I myxopapillary ependymoma of the filum terminale
Teaching points:
-Myxopapillary ependymomas are relatively common in the conus medullaris and the filum terminale; they are by far the most common tumours in those locations.
-They are slow-growing tumours that arise from ependymal glia of the filum terminale or conus medullaris or rarely from ependymal remnants in sacral regions.
-They are usually well circumscribed and do not infiltrate adjacent cord tissue.
-They have a tendency to bleed (myxopapillary ependymomas are the subtype of ependymomas that are most prone to haemorrhage),
which may lead to subarachnoid haemorrhage.
-They may calcify or undergo cystic degeneration.
-They tend to have an earlier clinical presentation than other spinal ependymomas,
with a mean age of presentation of 35 years.
-If they become large,
myxopapillary ependymomas may expand the spinal canal,
cause scalloping of the vertebral bodies,
and they may protrude through the neural exit foramina.
CASES 11 and 12: SCHWANNOMA
Case 11: 45–year-old man,
asymptomatic.
Routine follow-up MRI for discectomy detected an intradural extramedullary tumour at T12-L1 compressing the conus medullaris and nerve roots of the cauda equina.
Benign schwannoma was diagnosed at pathologic examination after surgical excision (Fig. 23).
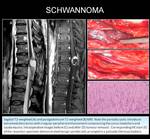
CASE 12: 66-year-old man with a several-month history of predominantly distal left upper limb paresis and predominantly proximal lower limb paresis affecting his gait.
He slowly developed quadriparesis.
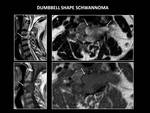
MRI detected a left-sided spinal lesion at C3-C4 with an intraspinal part (that has both intradural extramedullary component and extradural component and causes compressive myelopathy) and an extraspinal part (extending to the left foramen and paravertebral soft tissues).
A dumbbell-shaped Schwannoma was diagnosed ( Fig. 24, Fig. 25).
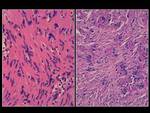
Teaching points:
-Schwannomas are considered benign tumors (>90% cases); they are the most common intradural extramedullary spinal lesions,
followed by meningiomas.
-Schwannomas are the most frequent type of nerve sheath tumors,
followed by neurofibromas.
-70% are intradural extramedullary,
25% extradural,
and <1%intramedullary.
- They often show cystic degeneration and haemorrhage.
-They usually present as solitary tumors. If multiple spinal root tumours are present,
think of NF1 (neurofibromas) or NF2 (schwannomas). Neurofibromatosis is present in 35%-45% of all patients with spinal nerve sheath tumours.
-Both neurofibromas and schwannomas may have an extradural component,
and extension through the foramina may be seen,
which potentially results in widening of the foramina (see Fig.24).
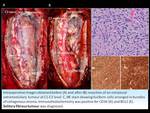
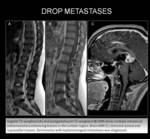
CASE 13: LEPTOMENINGEAL METASTASES
18-year-old man with diplopia and radicular pain.
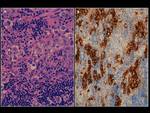
Brain MRI ruled out pineal and hypothalamic lesions and multiple intradural extramedullary lumbo-sacral lesions (Fig. 26).
One leptomeningeal lumbar lesion was surgically biopsied and histologic study diagnosed germinoma with leptomeningeal spread at the cauda equina (Fig. 27).
Teaching points:
-Intradural extramedullary metastases result from CSF spread from primary neoplasms.
-Primary tumors include:
*Central nervous system (Drop Metastases): Cerebral glioblastoma,
anaplastic astrocytoma,
ependymoma,
medulloblastoma,
PNET,
pineal tumors (germinoma,
pineoblastoma),
choroid plexus neoplasms).
*Non-CNS: lung cancer,
breast cancer,
melanoma,
lymphoma,
leukaemia.
-The lumbo-sacral region is the most common location.
INTRAMEDULLARY LESIONS
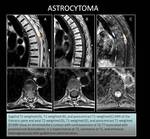
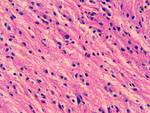
CASE 14: ASTROCYTOMA
51-year-old woman with lower limb paresthesias and mild motor deficit.
MRI detected an intramedullary lesion (Fig. 28).
Pathology diagnosed a grade II astrocytoma after surgical biopsy (Fig. 29),
and posterior subtotal tumour resection was done.
At follow-up,
the rest of the tumour was upgraded to a grade IV glioblastoma.
Teaching points:
-Astrocytoma is the most common intramedullary tumour in children and the second most common in adults.
-Most (75%) are low grade.
-They most frequently occur in the cervical and thoracic region.
-Astrocytomas diffusely invade the spinal cord and are difficult to delineate; they are more infiltrative than ependymomas and therefore complete resection of astrocytomas is rare.
-Eccentric location within the posterior spinal cord is typical.
-Several spine segments are involved at the time of diagnosis.
-Fusiform expansion of the cord is common.
-Cystic components are present in 30%.
-Despite the low grade,
nearly all enhance after contrast administration.
-The incidence of spinal astrocytomas is higher in patients with NF-1.
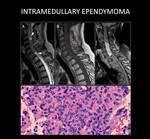
CASES 15 and 16: EPENDYMOMA
Case 15: 46-year-old man with cervical and thoracic back pain,
hypoesthesia in hands and feet,
motor deficit in hands,
and mild instability.
MRI detected a relatively well-defined intramedullary mass extending from C3 to C6,
with a widened cervical and thoracic cord and syringomyelia.
Grade II ependymoma was diagnosed after excision ( Fig. 30).
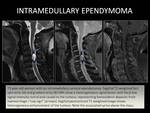
Case 16: 73-year-old woman with a several-month history of neck pain,
upper limb sensory loss,
and motor deficit in her hands.
Typical MRI findings enabled the diagnosis of an intramedullary cervical ependymoma.
( Fig. 31).
Teaching points:
-Ependymomas are the most common intramedullary tumors in adults.
-Cellular ependymomas most frequently occur in the cervical spine (unlike myxopapillary types,
which occur in the filum terminale and cauda equina).
-These slow-growing tumors are usually well circumscribed.
-They tend to be centrally located in the cord,
unlike astrocytomas,
which tend to be eccentric and more infiltrative.
-Cyst formation and haemorrhage are common,
especially at the tumour margins (hemosiderin deposits-“dark caps” are sometimes seen rostral and caudal to the tumour) (see Fig 29-different patient with a grade II cervical ependymoma).
-Intense,
homogeneous or heterogeneous enhancement after contrast is the rule.
-Syringohydromyelia may be associated,
especially with cervical ependymomas.
-They often can be surgically resected.
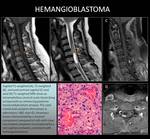
CASE 16: HEMANGIOBLASTOMA (Fig. 32)
31-year-old woman with cervical pain and Von Hipple-Lindau disease.
She recently had a cerebellar hemangioblastoma removed.
An intramedullary lesion consistent with hemangioblastoma was detected at C6.
Outcome was very good after excision of the cervical lesion.
Teaching points:
- Hemangioblastoma is the third most frequent intramedullary tumour.
-These tumors occur more commonly as sporadic isolated lesions (70%-80% of cases) rather than as multiple lesions,
as part of the dominantly inherited familial cancer syndrome,
von Hippel-Lindau disease (16%-25% of cases).
-Most (75%) spinal hemangioblastomas are intramedullary,
mainly located in the dorsal surface of the cord.
-MRI typically shows a large intramedullary cyst with a mural nodule.
-Symptomatic hemangioblastomas usually have relatively large associated syringes,
whereas asymptomatic lesions often do not.