Definition:
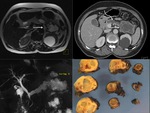
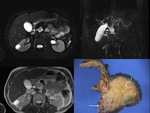
MD-IPMN is characterized by segmental or diffuse dilation of the main pancreatic duct (MPD) of>5mm without other causes of obstruction [3]. Fig. 1
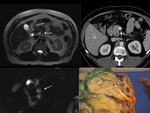
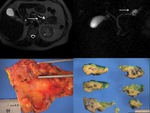
Pancreatic cysts of >5mm in diameter that communicate with the MPD should be considered as BD-IPMN (pseudocyst is another consideration). Fig. 2, Fig. 4.
IPMNs usually present in older patients,
with a greater male predominance.
Imaging:
Ultrasonographic Findings: Ultrasound can show a septate cystic lesion and dilated MPD.
Not sufficient for diagnosis.
CT Findings:
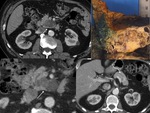
BPD type: Lobulated multicystic wih thin,
irregular,
peripheral ring-enhancing walls.
Fig. 4,
Fig. 5
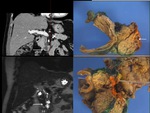
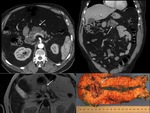
MPD type: Markedly dilated tortuous main duct.
Fig. 1 May see nodular lesions lining the duct.
Fig. 6 Calcification may also be seen.
Combined type: Multicystic lesion in the uncinate process communicating with a grossly dilated main duct.
Atrophy of the gland may be seen upstream from tumour.
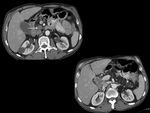
MR Findings:
Lobulated,
clustered cysts and dilated main ducts.
Can identify communication between cystic lesions & ducts.
May detect nodular filling defects. Can also assess for biliary obstruction.
EUS:
Endoscopic ultrasonography allows superior visualization; can guide biopsy & aspiration.
Elevated CEA is a marker that distinguishes mucinous from non-mucinous cysts,
but not benign from malignant cysts.
Histological subtypes:
There are 4 subtypes of cell origin of the papillary component of IPMNs; Gastric,
intestinal,
hepatobillary and oncocytic.
Gastric is the most common and oncocytic is the least common.
These are histopathological diagnoses and they cannot be distinguished on radiology.
It is felt that gastric and intestinal sub-types have less malignant potential and that carcinomas from intestinal types are less aggressive [4].
Differential Diagnosis:
Serous cystic neoplasms are the most common of the cystic neoplasms.
They have a four to one female to male predominance.
They are characteristically microcystic,
although they may be macrocystic.
Since they are only very rarely malignant,
symptomatic and enlarging lesions only should be surgically resected.
Mucinous cystic neoplasms mostly affect women between the 4th and 6th decades of life; they are mostly localized in the tail of the pancreas.
They do not communicate with the duct and contain an ovarian-type stromal component.
Surgery is indicated in any case in a diagnosis of MCN as these tumors have the potential for malignancy.
Solid papillary neoplasms are benign in more than 90% of cases and affect mainly young women.
Since they are not easily distinguishable from pancreatic cancer in terms of the differential diagnosis,
surgery is indicated.
Management: [3]
The management of IPMN is dictated by its subtype.
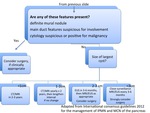
BD-IPMN Table 1,
Table 2
The incidence of malignancy in BD-IPMN is lower than MD-IPMN,
but remains significant,
up to 25%.
They occur mostly in elderly patients and surgical resection is not always possible.
"High risk stigmata" have been validated,
such as jaundice,
enhancing mural nodularity and main duct >10 mm,
and their presence should prompt surgical resection.
If these are not present,
a set of "worrisome features" contained in table 1 should also prompt consideration for surgery.
If these are not identified,
further evaluation with EUS+FNA is advised,
and if cytology is negative and no more "worrisome features" are identified,
follow-up surveillance can be performed dictated by lesion size.
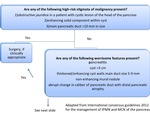
MD-IPMN
According to published literature,
MD-IPMNs have >50% presence of malignancy.
Due to the high incidence of malignancy,
surgical resection should be strongly considered in all surgically fit patients.
MD dilatation of 5-9 mm should be considered a "worrisome feature" as in BD types and should warrant evaluation (EUS+FNA).
In MD-IPMN,
unlike BD,
no consistent features of malignancy have been established (such as duct size,
presence of mural nodules or symptoms).
Fig. 6
Mixed type IPMNs are treated as MD types.
Multiple BD-IPMNs are considered a "field change",
but do not have an increased rate of malignancy when compared with solitary BD-IPMNs and should be treated according to the largest cyst as per single BD types.