Type:
Educational Exhibit
Keywords:
Inflammation, Connective tissue disorders, Arthritides, Education, Diagnostic procedure, Comparative studies, Ultrasound-Colour Doppler, Ultrasound, Conventional radiography, Musculoskeletal soft tissue, Musculoskeletal joint, Extremities
Authors:
H. Elfattach1, F. Houari1, O. Addou1, M. Maaroufi2, S. Tizniti2; 1Fez/MA, 2Fès/MA
DOI:
10.1594/ecr2013/C-2237
Imaging findings OR Procedure details
Imaging techniques
1. Musculoskeletal Ultrasound (US) :
- US is a relatively cheap,
non ionsing,
dynamic form of imaging that can provide both structural,
functional and vascular information.
- The us is characterized by the flexible,
repeatable and real-time imaging for clinical diagnosis,
monitoring and intervention of rheumatologic practice.
- US allows the operator to make a clinical assessment of the patient at the time of imaging along with easily allowing examination of the contralateral side or additional joints.
- the potential difficulties with US assessment of the joints are the inability to compare temporal changes directly at the time of scanning,
nonvisualization of internal bone structure,
inability to assess bone edema,
and inherent operator dependence of the technique.
2. Conventional radiography (CR) :
- CR has been widely used in both clinical and research settings to assess rheumatoid arthritis joint damage due to its feasibility,
but it has limitations in early disease detection.
- CR has traditionally been the mainstay for imaging patients with rheumatoid arthritis; findings such as soft-tissue swelling,
periarticular osteopenia,
joint space loss,
joint subluxation,
and marginal erosions are all features that may be seen.
However,
information regarding the synovium is much more difficult to assess on radiographs.
3. MRI :
- The Magnetic resonance imaging is the golden standard in the field of rheumatism.
It has the advantage of providing a more global view of the joint,
including the articular surfaces and internal bone structure.
- The disadvantages of using MRI include motion artifact,
the increased time necessary for the examination,
feasibility and potentially invasive administration of a contrast agent.
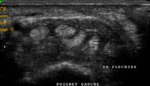
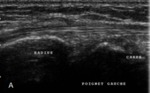
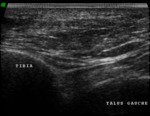
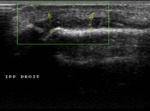
Normal Sonographic Anatomy (figures 1,2,3,4,5,6)
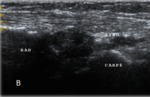
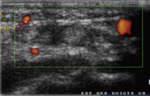
- Sonographically,
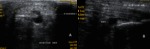
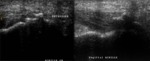
tendons are echogenic fibrillar structures that consist of multiple parallel lines in longitudinal planes and multiple dotlike echoes in transverse planes .
- The synovial sheath is depicted as a thin echogenic fluid-containing structure that surrounds the echogenic tendon fibers.
The synovial fluid is usually but not always anechoic.
Clinical presentation
- Patients most frequently present with pain and stiffness in one or multiple joints.
- The wrists,
metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints are the most commonly affected joints,
but any synovial joint can be affected.
- Usually bilateral and symmetric.
- Women are more commonly affected than men.
- In addition to joint-based pathology,
patients may present with extraarticular manifestations of the disease,
such as enthesopathy,
bursitis,
tenosynovitis,
and tendon rupture.
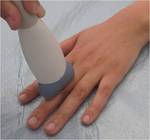
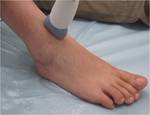
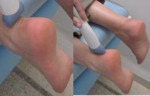
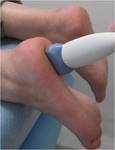
Sonographic Technique
- The ultrasound examination was performed with a high frequency transducer 15 MHz to visualise the earlier abnormalities,
including synovitis,
tenosynovitis,
bone erosions,
enthesitis,
and bursitis.
- All images were acquired by using a commercially available sonographic system with a 15MHz linear-array transducer.
- Gaining comparable pictures of the same anatomical area during different time
- A large standoff mound of gel was used to allow optimal visualization of the most superficial structures.
- The probe placed in an appropriate position for imaging of the specific areas of interest :
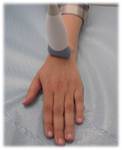
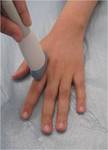
Sonographic Technique of the wrist(Figures 7,8,9,10)
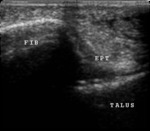
Sonographic Technique of the ankle(Figures 11,12,13,14)
Musculoskeletal Ultrasound findings
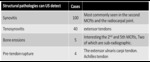
- The musculoskeletal US showed: 100 cases of synovitis,
40 of tenosynovitis,
5 bone erosions and 50 positive Doppler signals (Table 2).
SEMIOLOGY PATTERNS
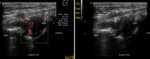
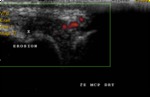
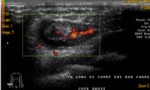
1. Synovitis : (figures 15,16,17,18,19,20)
- The synovial fluid is an abnormal hypoechoic or anechoic intraarticular material that can be displaced and compressed,
but without Doppler signal.
- The synovial hypertrophy that is represented by a hypoechoeic material that is non-displaceable,
poorly compressible and may exhibit Doppler signal.
- The nondisplaceable nature of synovitis on ultrasound is important because this characteristic distinguishes joint fluid from synovial thickening; however,
these two entities frequently coexist within one joint.
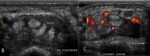
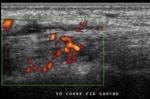
- The use of power Doppler has made it possible for US to determine the degree of synovial vascularity.
This can be assessed semi-quantitatively by scoring the amount of PD signals within the joint capsule on a 0–3 scale.
- Power Doppler ultrasound (PDUS) is shown to correlate well with histologically detected synovitis in inflamed joints and is reliable in qualitative grading of the synovium vascularity.
- Ultrasound has the advantage of clinical correlation and dynamic assessment of the joints at the time of scanning and is increasingly being performed by rheumatology clinicians in the outpatient setting.
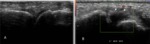
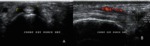
2. Bone erosions : (figures 21,22)
- The OMERACT definition of an erosion seen on ultrasound imaging is an intraarticular discontinuity of the bone surface that is visible in two perpendicular planes.
- US detects more RA joint erosions than CR especially in the context of early disease.
- Its limitations arise in areas where there is a poor
- acoustic window,
such as in the mid-carpus,
and the misinterpretation of normal anatomic variants as erosions.
- When compared with gold standard CT,
US has a moderate sensitivity but a high specificity and accuracy in detecting MCPJ erosions in RA.
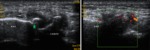
3. Tenosynovitis : (figures 23,24,25,26,27)
- The tenosynovitis on US is defined an hypoechoic or anechoic thickened tissue seen in two perpendicular planes with or without tendon sheath fluid and Doppler signal.
- Tenosynovitis is seen on ultrasound as an inflammation of the synovial sheath appearing on ultrasound as a concentric anechoic or hypoechoic swelling around the tendon.
4. Bursitis : (figure 28)
- Bursitis is characterised by an increase in the synovial fluid that usually appears as a sharply defined anechoic area.
- Its the fluid collections more or less limited,
more or less compressible,
often heterogeneous echogenicity.
Its walls are generally highly vascularized in power Doppler.
5. Enthesopathy : (figures 29,30)
- the enthesis has appeared hypoechoic or heterogeneous with possible thickening of it.
- Cortical erosions;
- Enthesophytes;
- Ossification;
- Doppler +
- Bursitis may be associated.