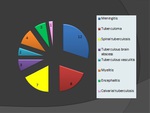
The results that were obtained: Fig.
2
- Meningitis (n=12),
- encephalitis (n=3),
- tuberculoma(n=8),
- tuberculous brain abscess (n=3),
- tuberculous vasculitis (n=2),
- myelitis (n=4),
- spinal tuberculosis (n=7),
- calvarial tuberculosis(n=1).
MENINGEAL TUBERCULOSIS
Tuberculous meningitis (TBM) is the most common presentation of neurotuberculosis and occurs predominantly in young children and adolescents.
Clinical features
TBM most often presents with fever,
headache,
decreased level of consciousness,
and meningeal signs such as neck stiffness,
photophobia,
and vomiting.
In addition,
symptoms related to cranial nerve involvement and focal ischemic syndromes may occur.
Radiological patterns
The common triad of neuroradiological findings in TBM are:
1.
Basal meningeal enhancement.
2.
Hydrocephalus.
3.
Infarctions in the supratentorial brain parenchyma and brainstem.
1.
Basal meningeal enhancement
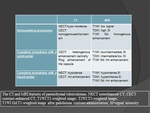
CT Findings
NECT
- May be normal early .
- Isodense to hyperdense exudate effaces CSF spaces,
fills basal cisterns,
sulci.
CECT
- Intense basilar meningeal enhancement that is linear or nodular.
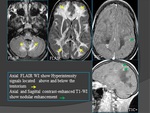
MR Findings: Fig.
3
T1WI
- Exudate isointense or hyperintense to CSF.
T2WI
- Exudate is isointense or hyperintense to CSF.
FLAIR
- Increased intensity in basal cisterns,
sulci related to proteinaceous exudate.
T1 GADO: idem CECT
2.
Hydrocephalus: Fig.
3
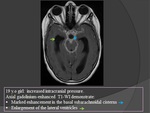
- Hydrocephalus is the most frequent complication of TBM and is usually more prominent in children.
- Hydrocephalus is generally of the communicating type and is secondary to blockage of CSF resorption by inflammatory exudates in the basal subarachnoidal cisterns.
- In addition to the dilatation of lateral ventricles,
an increased periventricular signal may be seen onT2-WI as a sign of interstitial oedema due to increased intraventricular pressure with transependymal migration of CSF.
3.
Infarctions in the supratentorial brain parenchyma and brainstem: Fig.
4,
5
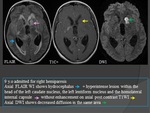
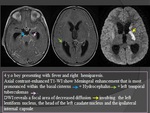
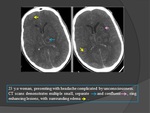
- Cerebral infarction is another common complication of basal meningitis which adds to morbidity and mortality.
- The majority of the infarcts are seen in the basal ganglia and internal capsule related to the encasement of the basal perforating arteries,
particularly the origin of the lenticulostriate arteries,
by the extensive basal meningeal exudates that characterize TBM.
The large vascular distribution territories of the anterior and middle cerebral arteries are less commonly involved.
- A high proportion of these infarctions are hemorrhagic and this may lead to cavitation.
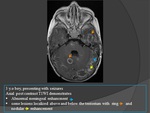
CT
- CT shows ill-defined hypodense areas with mass effect and variable peripheral,
sometimes diffuse,
IV contrast,
enhancement.
- These lesions progress to circumscribed hypodensities.
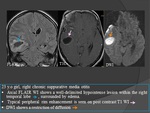
MRI
- A hyperintense lesion on T2-WI with mass effect and variable enhancement pattern after contrast of a recent infarct will progress to a cavitated infarct which is typically hypointense on T1-WI andhyperintense on T2-WI.
- FLAIR imaging may even be more useful to define the exact extent of the lesion and to differentiate old cerebral infarctions with cystic appearance from the surrounding tuberculous border zone encephalitis.
- MR angiography has also been reported to be a useful and non-invasive technique for assessment of vascular involvement in TBM.
Differential diagnosis
Infectious diseases:
- Nontuberculous bacterial,
viral or parasitic meningitis,
as well as fungi such as coccidioidomycosis and cryptococcosis.
Non-infectious inflammatory disease affecting the leptomeninges:
- rheumatoid disease,
sarcoidosis,
idiopathic pachymeningitis.
Meningeal carcinomatosis:
- meningeal spread of a medulloblastoma in children or breast carcinoma in adults.
TUBERCULOMA
- The most common parenchymal form of CNS TB is tuberculous granuloma (tuberculoma).
Other presentations of parenchymal diseases are tuberculous abscesses,
focal cerebritis and tuberculous encephalopathy.
- Tuberculomas can involve the brain,
spinal cord,
subarachnoid,
subdural or epidural space,
and may be solitary or multiple.
- In children,
tuberculomas predominate infratentorially,
whereas in adults lesions are predominantly found in the supratentorial compartment.
- The frontal and parietal lobes are the most commonly affected regions.
- Occasionally,
tuberculomas have been described in the intrasellar region,
brain stem,
thalami,
basal ganglia,
cerebellopontine angle,
optic pathways,
pineal region,
and the ventricles.
Clinical features
- The clinical presentation is more subtle than that of TBM.
- The common presenting symptoms are headache,
intracranial hypertension,
seizures,
focal neurological signs,
and papilledema; fever may be present.
Radiological patterns: Fig.
6
CT: Fig.
7
- Hypodense to hyperdense round or lobulated nodule/mass with moderate to marked edema.
- Ca++ uncommon.
- Solid or ring-enhancing "Target sign".
MRI: Fig.
7=>11
T1
- Non caseating granuloma: Hypointense to brain.
- Caseating granuloma with solid center: Hypointense or isointense to brain.
- Caseating granuloma with necrotic center: Hypointense or isointense to brain with central hypointensity.
- Caseating granulomas may have hyperintense rim.
T2 and FLAIR
- Non caseating granuloma: Hyperintense to brain.
- Caseating granuloma with solid center: Iso- to hypointense to brain.
- Caseating granuloma with necrotic center: Central hyperintensity with hypointense rim.
- Hypointense rim + surrounding edema common.
DWI
- May show hyperintense center of tuberculoma (may be hyper: restriction diffusion,
or hypo: increasing diffusion).
T1C+
- Noncaseating granuloma: Nodular,
homogeneous enhancement.
- Caseating granuloma with solid center: Peripheral rim enhancement.
- Caseating granuloma with necrotic center: Peripheral rim-enhancement,
central low signal.
Differential diagnosis
The differential of tuberculomas is essentially in the differential of ring-enhancing lesions,
and includes:
* Neurocysticercosis.
* Cerebral toxoplasmosis.
* CNS cryptococcosis
* Bacterial cerebral abscesses.
TUBERCULOUS ABSCESS
Tuberculous abscess formation is a rare complication,
observed in less than 10% of all patients with CNS tuberculosis.
Clinical features
- The TB abscess have a more accelerated clinical course than tuberculomas,
usually presenting acutely with fever,
headache,
and focal neurological signs.
Radiological patterns
CT
- Hypoattenuating lesions with surrounding edema,
mass effect,
and ring enhancement.
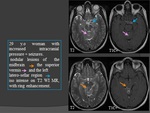
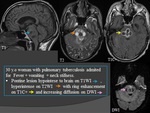
MRI: Fig.
12,
13
- Similar in appearance to liquid-centered caseating tuberculomas,
although they tend to be larger and are more often multiloculated.
- MRS: TB abscess has prominent lipid,
lactate but no amino acid resonances.
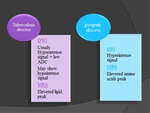
Differential diagnosis
Pyogenic abscess: Fig.
14,
15
- Pyogenic and tubercular abscesses may be differentiated by their unique metabolite pattern with recognition of amino acids,
acetate,
and succinate in pyogenic abscesses and lipid peak in tubercular abscesses.
In DWI,
pyogenic abcess show hypersignal,
when diffusion signal is variable in tuberculous abscess.
Primary or metastatic tumors
- Typically multiple lesions at the corticomedullary junction with significant edema.
- MR Spectroscopy shows increased Cho,
decreased NAA,
+/-lactate.
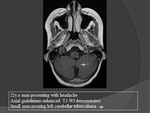
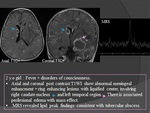
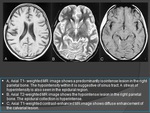
TUBERCULOUS ENCEPHALITIS (Fig.
16)
- Signs and symptoms: fever,
headache,
vomiting,
altered mental status,
irritability,
apathy.
- Severe unilateral or bilateral cerebral edema is seen on neuroimaging.
- Demyelination related T2 hyper intensities on MR imaging.
SPINAL TUBERCULOSIS
The most frequent site of spinal tuberculosis is the thoracolumbar junction .
The incidence decreases above and below this level.
However,
any segment of the spine can be involved.
Clinical features
- Often nonspecific clinical manifestations: spinal pain,
neurologic deficits…
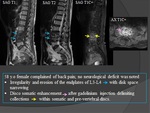
Radiological patterns
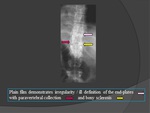
PLAIN FILM: Fig.
17
- Plain radiography is insensitive to the early changes of discitis / osteomyelitis,
with normal appearances being maintained for up to 2 - 4 weeks.
- Thereafter disc space narrowing and irregularity / ill definition of the end-plates can be seen.
- In untreated cases,
bony sclerosis may begin to appear in ~ 10 - 12 weeks.
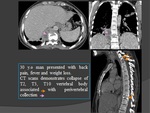
CT: Fig.
18
- CT findings are similar to plain film,
but more sensitive to earlier change.
Additionally surrounding soft tissue swelling,
collection and even epidural abscesses may be evident.
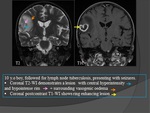
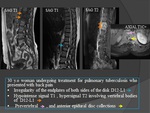
MRI: Fig.
19,
20,
21
This is the imaging modality of choice due to very high sensitivity and specificity.
Signal characteristics include:
T1
- Low signal in disc space (fluid).
- Low signal in adjacent endplates (bone marrow oedema).
- Loss of medullary fat high signal.
T2 : (Fat Sat or STIR especially useful)
- High signal in disc space (fluid).
- High signal in adjacent endplates (bone marrow oedema).
- Loss of low signal cortex at endplates.
- High signal in paravertebral soft tissues.
T1 C+ (Gd)
- Peripheral enhancement around fluid collection(s).
- Enhancement of vertebral endplates.
- Enhancement of perivertebral soft tissues.
- Enhancement around low density center indicated abscess formation (hard to distinguish inflammatory phlegmon from abscess without contrast).
Differential diagnosis
Pyogenic vertebral osteomyelitis
Rare spinal infections :
- Brucellosis.
- Fungal disease.
- Echinococcosis.
Other entities that may mimic tuberculous spondylodiscitis
- Vertebral body metastases.
- Primary vertebral neoplasm (lymphoma,
multiple myeloma, chordoma).
- inflammatory spondylodiscitis.
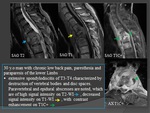
TUBERCULOUS MYELITIS
Tuberculousmyelitis usually occurs as a secondary event in the course of common forms of tuberculous meningitis.
Clinical features
- Radicular pain.
- Paraparesis.
Radiological patterns
The cervico-thoracic segment of the spinal cord is most commonly involved.
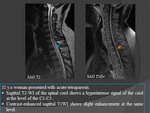
MRI: Fig.
22,
23
Diffuse cord swelling with signal abnormality.
Most spinal cord lesions appear as :
T1
- Isointense to hypointense.
T2
T1C+
- Segmental enhancement which may persist for several months.
Differential diagnosis
- Bacterial infection : e.g.
neuroborreliosis...
- Viral infection : e.g.
CMV...
- Parasitic infection : e.g.
toxoplasmosis...
- non-infectious inflammatory disease: e.g. sarcoidosis...
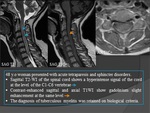
CALVARIAL TUBERCULOSIS
Isolated calvarial tuberculosis is a rare condition; and commonly occurs secondary to hematogenous spread from primary focus elsewhere.
Clinical features
- In most cases discussed in the literature,
patients present with painless scalp swelling and,
at times,
a discharging sinus in the scalp.
- Initial presentation with seizures ,
motor deficits ,
or other manifestations of meningitis is uncommon.
Radiological patterns
- Frontal and parietal bones are most commonly involved followed by occipital and sphenoid bone.
- Calvarial tuberculosis may present as a subgaleal swelling (Pott’s puffy tumor) with a discharging sinus when the outertable is involved.
- Inner table involvement which is relatively more common is associated with formation of underlying extradural granulation tissue.
- Both tables involvement is not uncommon.
PLAIN FILM
- Areas of rarefaction are seen early in the disease,
which develop into punched-out defects with a central sequestrum later on.
- Both osteolytic and osteoblastic areas may be seen.
- Rarely,
sclerosis may be seen and indicates secondary infection.
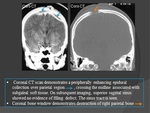
CT: Fig.
24
- Soft tissue swelling with accompanying destruction of one or both skull tables.
- A bony sequestrum may also be seen.
- Spread of the disease process to the extradural space,
meninges,
and brain parenchyma.
- Epidural granulation tissue appears as crescentic or lentiform low-attenuation collection.
The Surrounding meninges enhance intensely following contrast medium administration.
- Reveals evidence of meningitis and parenchymal disease.
MRI: Fig.
25
The highly specific imaging characteristics of MRI can,
in most cases,
lead to a conclusive diagnosis.
- T2WI show a high-signal-intensity soft tissue mass within the defect in bone .
- This may project into the subgaleal and/or epidural spaces and show peripheral capsular enhancement on the contrast-enhanced image.
Differential diagnosis
- Pyogenic osteomyelitis.
- Calvarial metastases.
- Multiple myeloma.
- Benign primitive osseous tumors: Hemangioma,
Giant cell tumor,
Aneurysmal bone cyst,
Langerhans cell histiocytosis.