The demographic,
clinical,
laboratory and microbiology data for the patients with PM are summarized in Table 2 .
A review of the medical records showed that most patients had documented chronic medical problems.
One patient,
case 1 had not any,
when PM criteria were found,
but diabetes mellitus was discovered two years later (See Table 1 ).
Eighteen patients had one or more underlying medical problems that could have been contributed to the development of PM.
These included diabetes mellitus (DM) (n=8),
malignancies including lung,
prostate and colorectal adenocarcinoma,
neuroendocrine tumor,
pleomorphic sarcoma,
and myelodisplastic syndrome (n=6); autoimmune disease,
ANCA-vasculitis and Langerhans cell histiocytosis (n=3); chronic renal insufficiency (n=3); underlying infections (n=2 had endocarditis); corticosteroids therapy (n=4); intravenous drug use and alcoholism (n=3) Table 1

Table 1: Underlying medical problems. M: male, F: female; DM: Diabetes mellitus, HCV: Hepatitis C Virus, HIV: Human Immunodeficiency Virus, COPD: Chronic obstructive pulmonary disease; ANCAs: Anti-neutrophil cytoplasmic antibodies.
Fever (n=10),
pain (n=11) and swelling (n=6) accounted for the commonest complaints at presentation.
In the 10 patients with fever,
the presence of localized redness and or heat,
or leukocytosis (white blood cells count higher than 109/L) were highly suggestive of infection or inflammation Table 2 .
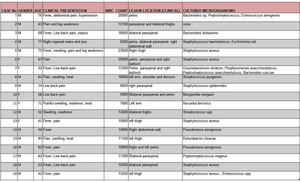
Table 2: The demographic, clinical, laboratory and microbiology data.
M: male, F: female; WBC: White blood cells.
The causative organisms were identified upon culturing of blood (n=2) or pus material (n=16).
Results of the cultures demonstrated that Staphylococcus species (n=7; S.
aureus: 5), Streptococcus sp (n=2), Pseudomona aeruginosa (n=2), Nocardia farcinica (n=1), Enterobacter cloacae (n=1), Morganella morganii (n=1), Peptostreptococcus magnus (n=1), Bacteroides distasonis (n=1).Four patients had more than one organism in the cultures (See Table 3 ).
Culturing proved negative in one patient.
At contrast enhanced-CT,
eighteen patients had at least one abscess (stage 2-3),
while one had no abscess (stage 1,
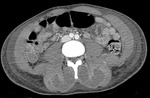
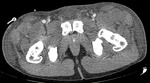
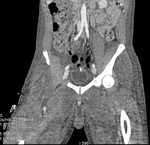
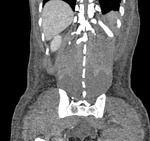
Fig. 1 Fig. 2 Fig. 3 Fig. 4).
In patient without abscess,
enlargement and decreased attenuation in muscle,
subcutaneous changes and extension (Involve more than one muscle bundle) were identified.
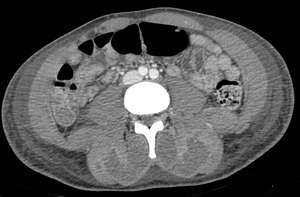
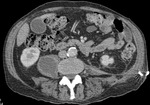
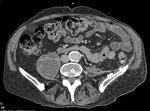
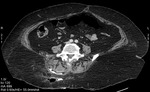
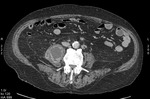
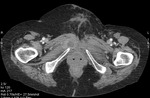
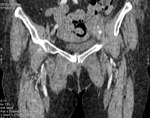
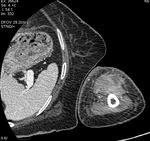
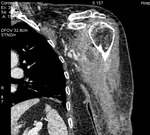
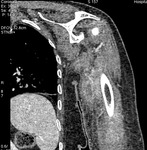
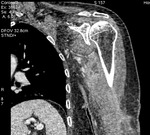
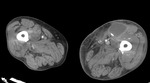
Fig. 1: Case 2. Pyomyositis of bilateral paraspinal and both thighs at its invasive or early stage (no abscess formation). Contrast-enhanced axial CT.
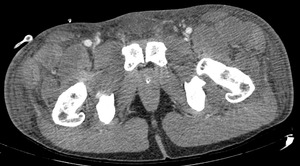
Fig. 2: Case 2. Pyomyositis of bilateral paraspinal and both thighs at its invasive or early stage (no abscess formation). Contrast-enhanced axial CT.
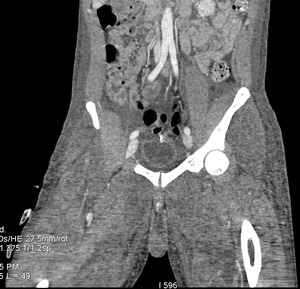
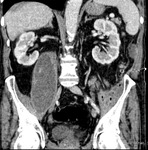
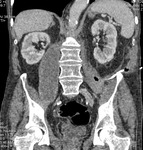
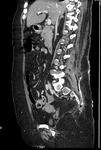
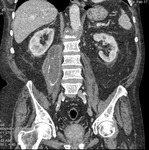
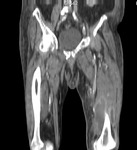
Fig. 3: Case 2. Pyomyositis of bilateral paraspinal and both thighs at its invasive or early stage (no abscess formation. Contrast-enhanced coronal CT.
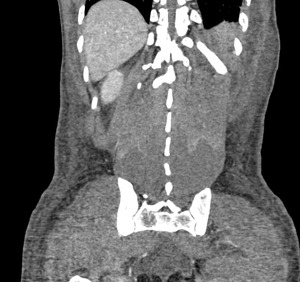
Fig. 4: Case 2. Pyomyositis of bilateral paraspinal and both thighs at its invasive or early stage (no abscess formation). Contrast-enhanced coronal CT.
In the 18 cases with abscess formation,
contrast-enhances CT studies demonstrated rim enhancement of the abscesses.
We included associated findings consistent with multiple/non-multiple abscesses (n=11/7) and extension into more than one muscle bundle (n=16).
The maximal diameters in three dimensions are showed in Table 3 .
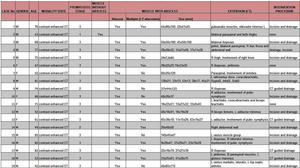

Table 3: Contrast-enhanced CT findings of affected muscle, extension and intramuscular abscesses in patients with pyomyositis
L: Left, R: Right; SupraS: Supraspinatus , InfraS: Infraspinous , SubS: Subscapularis.
Involvement of subcutaneous tissues was (6/19; 31.5%),
joints or bone (8/19; 42% Fig.
Fig. 9,
Fig. 10,
Fig. 11,
Fig. 12 ,
Fig. 13,
Fig. 14 and Fig. 17,
Fig. 18 ),
venous thrombosis (1/19; 5.3%).
Necrotizing fasciitis was excluded in all patients.
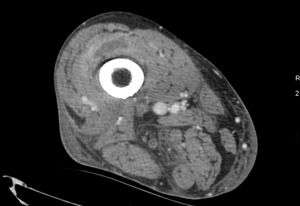
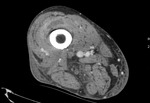
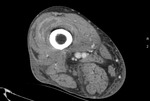
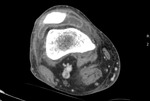
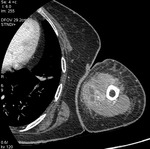
Fig. 9: Case 5. Pyomyositis of right thigh at its suppurative phase, multifocal abscess formation and involvement of right knee. Cultured microorganism Staphylococcus aureus. Contrast-enhanced axial CT.
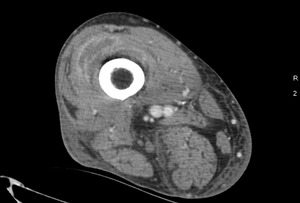
Fig. 10: Case 5. Pyomyositis of right thigh at its suppurative phase, multifocal abscess formation and involvement of right knee. Cultured microorganism Staphylococcus aureus. Contrast-enhanced axial CT.
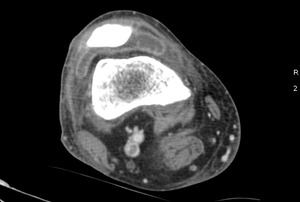
Fig. 11: Case 5. Pyomyositis of right thigh at its suppurative phase, multifocal abscess formation and involvement of right knee. Cultured microorganism Staphylococcus aureus. Contrast-enhanced axial CT.
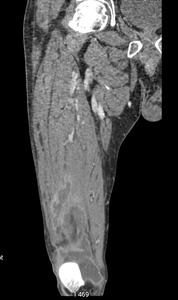
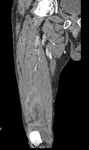
Fig. 12: Case 5. Pyomyositis of right thigh at its suppurative phase, multifocal abscess formation and involvement of right knee. Cultured microorganism Staphylococcus aureus. Contrast-enhanced coronal CT.
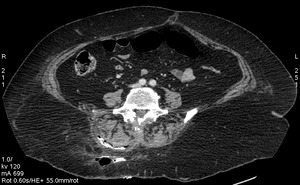
Fig. 13: Case 7. Pyomyositis of bilateral paraspinal muscles at its suppurative phase, multifocal abscess formation, gas and involvement of lumbar vertebra. Multiple anaerobic microorganisms were cultured. Contrast-enhanced axial CT.
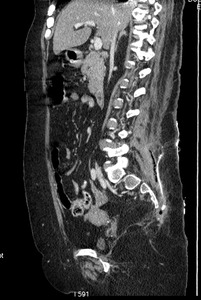
Fig. 14: Case 7. Pyomyositis of bilateral paraspinal muscles at its suppurative phase, multifocal abscess formation, gas and involvement of lumbar vertebra. Multiple anaerobic microorganisms were cultured. Contrast-enhanced sagital CT.
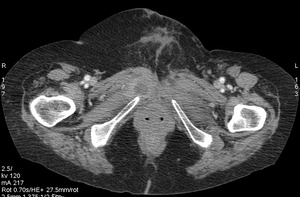
Fig. 17: Case 10. Pyomyositis of right adductor at its suppurative phase, with abscess formation and involvement of pubic symphysis. Cultured microorganism Morganella morganii. Contrast-enhanced axial CT.
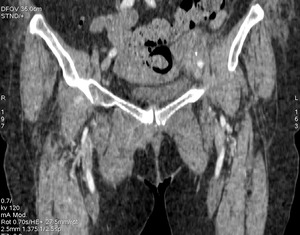
Fig. 18: Case 10. Pyomyositis of right adductor at its suppurative phase, with abscess formation and involvement of pubic symphysis . Cultured microorganism Morganella morganii. Contrast-enhanced coronal CT.
Lesion location was upper (n=2 Fig. 19,
Fig. 20,
Fig. 21,
Fig. 22,
Fig. 23 and Fig. 24); lower extremities (n=5 Fig. 9,
Fig. 10,
Fig. 11,
Fig. 12 and Fig. 25 ,Fig. 26) and trunk muscles (n=12 Fig. 1,
Fig. 2,
Fig. 3,
Fig. 4,
Fig. 5,
Fig. 6,
Fig. 7,
Fig. 8 and Fig. 13,
Fig. 14, Fig. 15, Fig. 16, Fig. 17, Fig. 18 ).
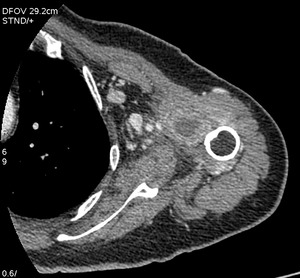
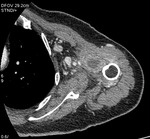
Fig. 19: Case 11. Pyomyositis of left brachialis, coracobrachialis and biceps brachialis at its suppurative phase, with abscess formation. Cultured microorganism Nocardia farcinica. Contrast-enhanced axial CT.
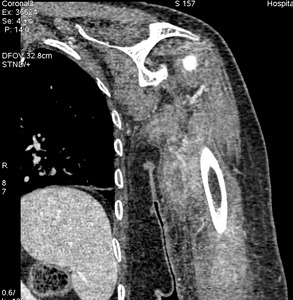
Fig. 23: Case 11. Pyomyositis of left brachialis, coracobrachialis and biceps brachialis at its suppurative phase, with abscess formation. Cultured microorganism Nocardia farcinica. Contrast-enhanced coronal CT.