Virtual Biopsy guided core biopsy was performed both in ex vivo (chicken-breast with olives with pit as mimicking lesions) and in vivo on 20 patients already scheduled for core biopsy.
On 15 patients the Virtual Biopsy was performed directly with 2D scans,
on 5 patients the Virtual Biopsy was used with the fusion between the real-time 2D scan and the already acquired 3DPan volumes of the same patients.
On the ex vivo phantoms,
both Virtual Biopsy and fusion imaging with 3DPan and 2D acquisitions were performed.
The 3DPan technology enabled a wider panoramic view of the area of intervention.
A proper MCS was used in order to counteract involuntary patients movements.
The MCS (used only in “in vivo” tests) was placed on the patient’s sternum and there fixed with plaster strips.
The patients and the chicken-breast phantoms (CBP) were positioned on a non-metallic table (due to reduce any possible interference for the Virtual Navigator electromagnetic reference space).
A.
Ex vivo test
The ex-vivo performance tests of the Virtual Biopsy tool were performed on the CBP with an olive (with pit) as lesion-like target (LLT).
Two CBP were created: one with a single LLT and another CBP with four different LLTs.
Both 2D B-Mode scans and 3DPan (B-Mode only) of the CBP were acquired with custom color volumetric targets,
in order to better identify the interesting areas.
Regarding the 3DPan US,
each CBP was scanned longitudinally,
acquiring three US volumes (22 seconds scan time for each US 3D acquisition).
The acquired US volumes were then fused together with 3DPan tool,
in order to obtain a panoramic volume of almost half CBP containing the LLT.
The obtained Pan volume was achieved with the “Auto” gluing algorithm.
A surface shift after the US volumes gluing was noted: the reason of this shift can be found in the pressure applied on the probe during the CBP volume acquisitions.
Different tissue densities of the CBP areas can lead to different compressions during scanning.
The Auto gluing algorithm,
recognizing and matching the inner structures of the scanned volumes (focused on the re-alignment of inner structures) and leaving a discontinuity reconstruction only at the surface level,
considered the “less interesting” part of the reconstructed volume.
The LLT and its surrounding tissues were examined also using elastosonography; tissue stiffness evaluation and the relative stiffness measurements (ElaXto Ratio) were performed on the LLT and the surrounding CBP areas.
In terms of elasticity,
the olive,
with respect to the surrounding chicken-breast,
resulted 7 times harder,
as measured with the ElaXto Ratio,
where two Z-zones (Z1 and Z2) were traced on the ElaXto image and then the system provided a strain ratio,
related to the tissues included in the traced Z-zones.
The resulting value is directly proportional to the tissue elasticity included in zone Z2,
compared to the one of zone Z1.
The elastosonography evaluation of the LLT and the surrounding structures of the CBP stiffness was performed also during real-time simultaneous visualization of 2D US scan,
fused with the glued volume US.
Elastosonography helped the operator to clearly detect the LLT,
being stiffer than the CBP surrounding tissues.
Bi-dimensional US elastosonography examination was performed in different directions,
scanning the CBP on several planes containing different LLT views,
in order to include the whole area around the LLT.
Once the 3DPan volumes were acquired,
the 2D scans were fused in real-time with the panoramic vision of the CBP area containing the LLT which was sampled using the CIVCO eTRAX Needle Guidance System.
The biopsy was planned and executed using the Virtual Biopsy tool both on the 2D scan alone and also on the 3DPan fusion when pre-acquired.
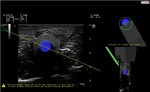
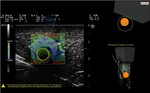
Needle insertions were performed in plane and out of plane: proper graphical indications of the correct or incorrect trajectory of the needle were given to the operator in real-time (Fig.
4).
In our tests,
once the planning path and insertion point were decided,
the operator switched off the US reference image inserting the needle,
following only the Virtual Biopsy graphical indications (the system gives to the operator also the information of the distance from the target of the needle tip in cm).
See Fig.
5.
The US reference image was switched-on again only when the target was hit,
according to the Virtual Biopsy graphical indications (Fig.
6).
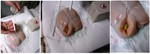
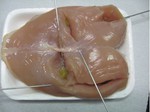
After the biopsy procedure,
the CBP was cut in close proximity of the LLT,
paying attention not to move the LLT itself and observing if the target was hit in the center as expected (Fig.
7).
The same test was performed also on a CBP with 4 LLTs.
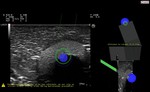
The insertion of the needle was performed also out of plane (Fig.
8) and with the real-time fusion of the pre-acquired 3DPan of the CBP area containing the LLT to be biopsied (Fig.
9).
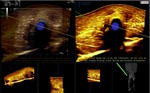
Elastosonography was used in order to check the elasticity of the tissues around the LLT (Fig.
10).
After the needle insertion (also in this case performed with the US reference image switched-off),
the CBP was cut in order to directly check if the target was hit in the center (Fig.
11)
B.
In Vivo test
In vivo core biopsies were performed with BARD Magnum 15mm 14 gauge and with Hospital Service Spring Biopsy needle PRECISA.
Both core biopsy tools were electromagnetically tracked within the Virtual Navigator reference space using the CIVCO VTrax.
For the Hologic ATEC 12cm 9 Gauge with Suros Hologic suction unit a CIVCO 653-002,
Sterile ATEC vacuum-assisted breast biopsy tracking bracket was used for its Virtual Navigator real-time tracking.
The in vivo tests were performed during routine US breast examinations,
related to suspected breast lesions.
The MCS was used and positioned on the patient’s sternum in order to counteract involuntary movements.
Virtual Biopsy test procedure was similar to the one for the in ex vivo tests.
Core breast biopsies were performed both on 2D US scans alone and in 5 cases also through real-time fusion with previously acquired 3DPan volumes of the area to be biopsied.
Virtual Navigator 3DPan tool fused different 3D US B-Mode and/or three dimensional Color Doppler or Power Doppler volume acquisitions: in our tests only B-Mode acquisitions were performed.
3DPan tool made the fusion of two or more US volumes captured by an electromagnetic tracked free-hand acquisition; in order to ensure a visual continuity to the acquired volumes,
a proper level of overlapping of one volume with the adjacent one was needed (5mm were considered sufficient).
The scanning velocity during Virtual Navigator 3DPan acquisitions didn’t affect the reconstruction,
as in the conventional 2D US panoramic imaging not electromagnetically tracked,
where the quality and the dimension – length - of the final merged image is related to the acquisition scanning velocity.
Furthermore,
Virtual Navigator electromagnetic tracking technology enabled monodirectional scanning,
without paying attention to the velocity of the transducer movement.
Two US volumes (15 seconds maximum scan time each) were acquired,
using large width array LA923 on 3 subjects,
then fused together with 3DPan tool and finally navigated with the more ergonomic LA533 without any re-synchronization procedure.
On 2 subjects the Virtual Navigator 3DPan tool was employed for the fusion of three volumes (15 seconds maximum scan time each) obtained directly with LA533 probe.
The probe choice for the 3DPan volume acquisition depended on the breast dimensions,
morphology and the area to be reconstructed.
The reconstruction of the axilla needed a large amount of gel.
Virtual Navigator 3DPan acquisitions were performed taking care to maintain an overlapping region among the different US volume acquisitions and to limit as much as possible the shadowing effect,
which is due to poor probe-tissue coupling with consequent reduction in image quality,
in order to obtain high quality B-Mode imaging in all the examined volumes.
The scanning of the same volume from two different starting points was avoided in order not to confuse the reconstruction algorithm.
This happens,
for example,
when conventionally scanning an elongated breast: the nipple area was imaged from bottom to top and vice versa,
acquiring the same structures twice.
The complete duration of the US breast examination was increased by about 5 minutes,
due to the 3DPan acquisitions.
Custom color volumetric targets,
visible on both 2D US,
3DPan volume and Virtual Biopsy environment,
were used in order to better identify the interesting areas.
Color Doppler,
Power Doppler,
Pulsed Wave Doppler evaluations were performed also during real-time simultaneous visualization of 2D US scan fused with the glued volume US,
in order to make a hemodynamic assessment of the lesions and of the surrounding areas.
Elastosonography was used in order to recognize breast stiffer regions and to perform elasticity measurement among different tissues.
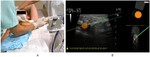
Virtual Biopsy tool was used in core biopsy procedures guiding both with 2D US scans only and,
in case of the real-time fusion,
with pre-acquired 3DPan volumes (Fig 12).
The acquisitions and the core biopsies were performed by the expert and by the non-expert operators.
All in vivo and ex vivo tests were successful: Virtual Biopsy enabled the correct core biopsy procedure both in ex vivo and in vivo for all the tests and both for the experts and for the novices.