In HD an average of 5.7 cycles of chemotherapy were conducted per patient (range 2-12 cycles),
in NHL – 7.9 cycles (range 4-18).
Radiotherapy was applied in 15 (79%) patients with HD and 16 (52%) patients with NHL.
Total number of CT examinations performed in 50 patients was 665.
It was performed 13.3 CT exams in average per patient.
32 (64%) patients underwent 10 or more CT exams,
10 (20%) patients underwent 20 or more exams.
The biggest proportion of CT examinations was carried out during chemotherapy (244 exams,
37%),
followed by examinations after treatment (198 exams,
30%),
before treatment (169 exams,
25%) and for radiotherapy planning (54 exams,
8%).
Distribution of CT studies by time period is presented in Table 1.
Table 1: Number of CT examinations per patient by time period.
|
Time period
|
Lymphoma type
|
|
All lymphomas
(n = 50)
|
HD (n = 19)
|
NHL
(n = 31)
|
|
Before treatment
|
3.4 (1-6)
|
3.5 (2-6)
|
3.3 (1-6)
|
|
During chemotherapy
|
4.9 (0-24)
|
4.7 (0-13)
|
5.0 (0-24)
|
|
Radiotherapy planning
|
1.1 (0-3)
|
1.7 (0-3)
|
0.7 (0-3)
|
|
After treatment
|
4.0 (0-14)
|
4.1 (0-1)
|
3.9 (0-14)
|
|
All periods
|
13.3 (3-29)
|
14.0 (5-26)
|
12.9 (3-29)
|
Footnote.
Value outside the parentheses is a mean number of examinations,
values in parentheses - the interval.
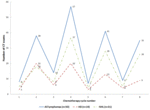
In the course of chemotherapy CT was most often performed after 4 cycles,
followed in descending order of frequency after 6,
2 and 8 cycles (Figure 1).
Multiplicity of greatest number of CT examinations to two chemotherapy cycles is explained by the fact that to determine tumor sensitivity to a specific schema of chemotherapy at least two cycles must be conducted.
In the absence of treatment effect as seen with CT,
chemotherapy schema might be changed with next CT after two successive cycles.
Data on the number of CT examinations by body region performed during the entire period of diagnosis,
treatment and monitoring are presented in Table 2.
CT of the thorax was the most often examination regardless of lymphoma type followed in the order of decreasing frequency by CT of abdomen,
pelvis and neck.
Table 2: Number of CT examinations by body region.
|
Body region
|
Lymphoma type
|
|
All lymphomas
(n = 50)
|
HD (n = 19)
|
NHL (n = 31)
|
|
Neck
|
55 (9)
|
32 (13)
|
23 (6)
|
|
Thorax
|
252 (40)
|
113 (45)
|
139 (37)
|
|
Abdomen
|
190 (30)
|
64 (25)
|
126 (34)
|
|
Pelvis
|
128 (21)
|
42 (17)
|
86 (23)
|
|
All exams
|
625 (100)
|
251 (100)
|
374 (100)
|
Footnote.
Value outside the parentheses is a number of exams,
value in parentheses is a percentage of the total number of exams in this type of lymphoma.
Based on data on number of CT examinations by body region effective dose per patient has been calculated (Table 3).
Table 3: Effective dose from CT examinations in mSv per patient by time period.
|
Time period
|
Lymphoma type
|
|
All lymphomas
(n = 50)
|
HD (n = 19)
|
NHL (n = 31)
|
|
Before treatment
|
23.0 (6.9-43.4)
|
23.8 (13.9-35.6)
|
22.5 (6.9-43.4)
|
|
During chemotherapy
|
32.8 (0-173.6)
|
31.9 (0-88.2)
|
33.4 (0-173.6)
|
|
Radiotherapy planning
|
4.7 (0-16.5)
|
6.5 (0-16.5)
|
3.6 (0-14.8)
|
|
After treatment
|
26.1 (0-100.7)
|
25.4 (0-77.3)
|
26.5 (0-100.7)
|
|
All periods
|
86.7 (21.7-209.2)
|
87.6 (34.6-176.8)
|
86.1 (21.7-209.2)
|
Footnote.
Value outside the parentheses is a mean dose,
values in parentheses - the interval.
The collective effective dose in this study was 4.3 Sv,
the mean dose per patient – 86.7 mSv and was not different in HD and NHL.
37 (74%) patients received more than 50 mSv during the entire time period,
14 (28%) patients – more than 100 mSv,
6 (12%) patients – more than 150 mSv and 1 (2%) patient – more than 200 mSv.
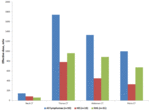
The contribution of the main types of CT examinations by body region to collective radiation dose is shown in Figure 2.
According to ICRP at doses above 100 mSv the risk of deterministic effects of irradiation and of the development of cancer increases.
For this reason,
the maximum value for a reference level is 100 mSv incurred either acutely or in a year [3].
In our study,
effective dose accumulated during one year from initial CT examination exceeded 100 mSv in 6 patients.
3 of these patients had HD and 3 others NHL; one patient had stage III disease and 5 patients stage IV; 6 cycles of chemotherapy were prescribed to one patient,
8 cycles to three,
12 and 18 cycles to one patient each.
It’s obvious that this group of patients had most advanced disease and most intensive treatment prescribed which explains a big number of CT scans and a high level of irradiation.
Given the collective radiation dose of 4.3 Sv in 50 patients,
0.176 additional cases of cancer associated with exposure during CT examinations can be expected which is equivalent to risk of 0.35% or 1 per 256 patients.
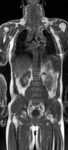
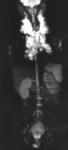
In patients with systemic oncologic diseases such as lymphoma who underwent multiple CT examinations during course of diagnosis,
treatment and follow-up potential of other non-irradiating diagnostic imaging techniques such as diffusion-weighted MRI should be evaluated (Figures 3-6).