Results:
The mean follow-up period was 13.0 months.
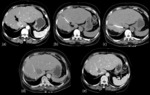
We ran a enhanced CT scan to evaluate the technical success rate of the combination therapy.
On the CT scan,
80 cases were induced to complete necrosis and 6 cases of incomplete necrosis by one session got additional another session (mean 1.07 session per mass).And then induced to complete necrosis at the first day after the additional session on CT scan as all the 86 cases of tumors were induced to complete necrosis meaning 100% procedural success rate.
As we ran an enhanced CT scan one month after the procedure to evaluate primary technical effectiveness,
83 out of 86 cases were induced to complete necrosis and 3 cases to incomplete necrosis,
meaning 96.6% primary technical success rate.
Within follow-up period we found total 9 cases(10.4%) of local recurrence in procedure site,
33 cases(45.8%) of new HCC on other sites of livers and 7 cases(9.7%) of extrahepatic metastasis(figure 2).
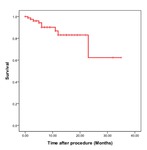
Cumulative local recurrence free survial rate were 90.2%,
83.1% and 62.3% for 6 month,
12 month and 24 month after the procedure respectively(figure 3).
We evaluated poor prognostic factors for cumulative local recurrence free survial rate through univariate analysis.
Statistically significant factors are two,
incomplete necrosis by one session combination therapy needing additional session and the size of tumors more than 3cm(figure 4).
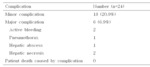
24(27.8%) cases developed complications after the procedure,
18 out of 24 cases were relieved by conservative treatment and 6 cases with major complication needed additional treatment or procedure.
Out of 6 cases with major complication,
there were 2 cases of active bleeding in the procedure site,
2 cases of the necrosis of the adjacent liver parenchyma,
one case of pneumothorax and one liver abscess.
There were no complication related deaths as all relieved by additional treatment and procedure(figure 5).
Discussion:
RFA is widely used as a one of the non-operative local treatments to treat HCC when it is impossible to get a surgical resection because of patient's poor hepatic function while get diagnosed.
Especially to small HCC ,
the prodecure has been reported to have outstanding effects and safety(7,8).
The principle is inserting an electrode releasing high frequency wave around 460kHz into tumor region,
so the ions of the tissue surrounding the electrode is agitated,
generating frictional heat by which the tissue is induced to coagulation necrosis(9).
If the tumor is a single nodule less than 5cm or if the number of tumors were three or less and all less than 3cm,
RFA is prefered to PEI because of its low number of session times and high rate of complete necrosis.
Some studies reported that the rate of complete necrosis was 88-98% in small HCC and 80-90% in 3-5cm HCC(10-13).
While RFA has some limitations in tumor size and location,
also has been reported to have slightly high complication rate 0-12% and 0.1-0.5% mortality rate.
According to the report of Livraghi(15),
the complete necrosis rate was 90% in less than 3cm,
71% in 3-5 cm and 45% in more than 5 cm.
So tumors larger than 5 cm have decreased treatment effects.
If tumors are located under hepatic capsules or infiltrate it,
we need to coagulate the capsule for complete necrosis,
but it could lead to complications like bleeding due to capsular necrosis or seeding of tumor and also makes it hard to reserve safety margin.
When tumors are adjacent to a large-diameter intrahepatic vessels,
complete coagulation is hard because of the heat-sink effect and injury of blood vessels can happen(16,17).
Also If the tumors are close to major organs like gall bladder,
kidney,
diaphragm,
adrenal gland or colon,
because of the difficulty to insert electrode and the possibility to injure major organs,
these tumors are included to high-risk group for RFA.
So we tried to combine RFA with PEI easily accessible by 21-22 gauge fine needle to improve the treatment outcome as reserving safety margins of RFA high-risk group tumors,
increasing the range of coagulation and reducing local recurrence rate(figure 6).
In some studies,
RFA after the vessels inside tumors necrotized with PEI can have low incidence of heat-sink effect and safely extend the range of coagulation better than RFA alone(18,19).
In this study,
to analyze treatment outcome of combined use of RFA and PEI to HCC of RFA high-risk group,
we took a CT scan on the first day and then a month after the procedure.
6 cases of incomplete necrosis on enhance CT of the first day got RFA one more session,
then all 86 cases were induced to complete necrosis meaning 100% technical success rate.
Also 83 cases were found induced to complete necrosis on CT scans of a month after the procedure,
showing high primary technical success rate.
This result is similar to that of Wong(20) report.
Local recurrence due to not reserving enough safety margin is the main reason of the failure of local treatment of HCC.
Also around 20% recurrence rate of small HCC less than 3cm has been reported(12).
In this study,
there have been 9 cases(10.4%) of local recurrence within follow-up period.
This result is similar to those of other studies reporting that combined use of RFA and PEI is better than RFA alone on the point of local recurrence rate(21).
Cumulative local recurrence free survial rates were 90.2%,
83.1% and 62.3% for 6 month,
12 month and 24 month after the procedure respectively.
It is higher the rates of a few other studies(20).
There are some factors for the better outcome.
One factor is that the mean size of the tumors in this study(2.4cm) was smaller than that of other reported studies(2.8cm) and our well experienced intervention practitioners may be one of the factors.
We evaluated poor prognostic factors for cumulative local recurrence free survial rate through univariate analysis.
Statistically significant factors are two,
incomplete necrosis by one session of combined procedure needing additional session and the size of tumors more than 3cm.
It is similar to the results of other known studies(20).
At first we thought presence of portal vein tumor thrombosis at the time procedures performed as statistically significant bad prognostic factor.
But it was valid only for 6 months of follow-up period so we excluded it in this study.
The number of cases developing complications from the procedure was 24(27.8%) and most complications were relieved by conservative treatment.
No patient died from the procedure.
Still we didn't directly compare the complication rate to that of RFA alone group,
it is similar to the complication rate reported in other studies.
So combined use of RFA and PEI is thought to be a safe procedure.