Study population
This retrospective study was approved by the Institutional Review Board of our institution,
and written informed consent was obtained from all patients.
Between February 2011 to September 2012,
877 women had screening or diagnostic mammograms with fully automated volumetric breast density analysis.
The 17 Patients with a history of breast-conserving surgery,
or mastectomy with breast cancer were excluded,
and final 860 women were included in this study.
The standard craniocaudal (CC) and mediolateral oblique (MLO) views of films were obtained for each breast using dedicated full-field digital mammography (Senographe DS; GE Healthcare,
Milwaukee,
WI).
The mammographic evaluation by radiologists
One radiologist (S.Y.M) who was board certified with 6 year experiences in breast imaging and a 3rd-grade radiology resident (L.H.N) independently reviewed mammographic density by qualitative BI-RADS density classification.
Additionally,
breast dedicated radiologist (S.Y.M) evaluated BI-RADS final assessment based on the mammographic findings.
All readers were blinded to the previous results and information about patients.
We divided the mammographic breast density assessed by Volpara,
according toBI-RADS classification into two groups,
fatty and dense groups to evaluate the association with mammographic BI-RADS final assessment.
Fatty group included category 1 and 2 of BI-RADS density classification,
and dense group included category 3 and 4 of BI-RADS density classification.
After evaluation of mammography of all patients,
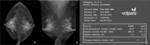
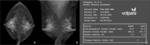
we reclassified agreement and disagreement groups according to agreement between BI-RADS density category(4 grade category) assessed by experienced radiologist and VDG (Figure 1,
2).
The clinic-radiologic factors that can affect difference between agreement and disagreement groups were evaluated.
The patient’s age,
indication of mammography (diagnostic or screening groups according to the purpose of performing mammography),
the mammographic BI-RADS final assessment and the difference in bilateral breast density assessed by VDG were included as clinico-radiologic factors.
We defined difference in bilateral breast density,
when there was more than one grade difference of VDG between right and left breast.
We also defined the mammographic BI-RADS final assessment category 0,
3,
4,
5,
6 as positive finding and category 1,
2 as negative findings.
The mammographic evaluation by fully automated volumetric breast density
For each mammographic image,
we assessed volumetric breast density with commercially available software (Volpara®,
version 1.5.1,
Matakina Technology,
Wellington,
New Zealand).
Volpara is a fully automated,
volumetric breast density assessment software and it provides VBD (volumetric breast density) and VDG (volpara density grade).
Volpara software can work out the mapping from each brightness in the image to a thickness of fibroglandular tissue and thickness of fat that must have been present between the pixel and x-ray source.
Summing those across the image calculates total volume of fibroglandular tissue,
and dividing that by volume of breast (found from the compressed breast thickness and projected area) represents the volumetric breast density.
The breast density result is provided per breast (by averaging the craniocaudal and mediolateral oblique values).
VDG was determined automatically according to VBD values.
VBD of 0~4.7% corresponds to VDG 1,
4.8~7.9% to VDG 2,
8.0~15.0% to VDG 3,
and more than 15.1% to VDG 4 [10]
Statistical analysis
Interobserver agreement about the evaluation of breast density between two radiologists and the agreement between the BI-RADS density category by experienced radiologist and VDG were assessed using kappa statistics (к).
The strengths of agreement were expressed in kappa values: A value of 0.20 or less indicated poor; 0.21–0.40,
fair; 0.41–0.60,
moderate; 0.61–0.80,
good; and 0.81–1.00,
very good agreement [11].
The association of the automated volumetric breast density that was reclassified into fatty or dense with the mammographic BI-RADS final assessment were also evaluated by using the Fisher’s exact test.
The clinico-radiologic factors that can affect difference between agreement and disagreement groups were evaluated by univariate and multivariate analysis.
In univariate analysis,
we used t-test for continuous variable such as age,
and chi-square or Fisher’s exact tests for non-continuous variables that included indication of mammography (diagnostic or screenings),
mammographic BI-RADS final assessment and the difference in bilateral breast density assessed by VDG.
We also performed multivariate analysis to estimate the odds ratio and 95% confidence intervals (CI).
In multivariate analysis,
we included all variables that were used in univariate analysis.
The automated volumetric breast density measurement (VDG) was regarded as reference standard.
Spearman’s correlation coefficient (ρ) was used to evaluate the correlation between the BI-RADS density category and volumetric breast density assessed by the fully automated software.
SAS (version 9.2,
SAS Institute Inc.,
Cary,
NC,
US) and Microsoft Excel (Redmond,
Wash,
US),
were used to perform all statistical analyses.
P-values less than 0.05 were considered significant.