This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
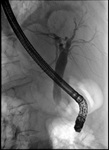
Gastrointestinal tract, Fluoroscopy, Endoscopy, Cholangiography
Authors:
E. Saukko1, A. Henner2, S.-M. Ahonen2; 1Turku/FI, 2Oulu/FI
DOI:
10.1594/ecr2015/C-0236
Results
A response rate of 100% was achieved in this study.
Most of the respondents were female (90%,
n=9) and 60% (n=6) of all persons were under 50-years.
The respondents̕ positions in hospital were radiographer (70%,
n=7) or registered nurse (30%,
n=3).
Half of the respondents (n=5) had over 10 years of experience on ERCP.
The ERCP procedures were carried out in Finnish hospitals both in X-ray departments (n=6) and endoscopy units (n=4).
An annual ERCP case volume varies according to the size of the each hospital,
as follows: 100-199 (n=3),
200-299 (n=3),
300-399 (n=1),
400-499 (n=2) and ≥500 (n=1).
The X-ray equipment used in ERCP consists of a stationary fluoroscopic X-ray system (n=2),
multipurpose (c-arm) fluoroscopy system (n=6) or mobile c-arm unit (n=3),
with X-ray tube located above (n=1) or under (n=10) the patient table.
In one large hospital,
two different fluoroscopic systems were used in performing ERCP.
A radiographer was a part of ERCP team in seven out of ten hospitals and a radiologist was involved in ERCP in one hospital.
Fluoroscopic equipment was operated by endoscopist (n=6) or by radiographer (n=5),
but the endoscopist was a person who pressed the foot pedal to release an X-ray beam in each hospital.
DAP-meter and LIH (last-image hold) function was found from all fluoroscopy sysems used in ERCP.
Patients were usually examined in the prone position during ERCP.
Radiation protection practice in ERCP was evaluated from the workers and patient perspective.
Protective lead aprons (100%) with thyroid shield (100%) and leaded glasses (90%) were worn by staff during their work in controlled areas.
Protection from scattered radiation was operated by the mobile shields (70%),
lead curtains (90%) and ceiling-mounted protective shield (90%).
Table 1 presents the diversity of radiation protective equipment used in ERCP in Finnish university and central hospitals.
Protection of the patient during ERCP varied significantly between the hospitals.
The use of a pelvic lead shield during ERCP was relatively low and a lead shield for protection of breast tissue in female patients was not used at all.
The use of the radiation dose reduction techniques during ERCP varied greatly among the hospitals,
as well.
Pulsed fluoroscopy was used in most of the hospitals (n=9),
but the pulse rate varied greatly,
from 1.5 fps to 15 fps.
Fluoroscopy pulse rate was not modified at all during the ERCP in almost all of the hospitals.
The results showed that a purpose of available fluoroscopy modes such as low,
medium and high,
was unclear for the respondents.
There were many missing answers related to question about fluoroscopy modes.
Collimation to the anatomic region of interest was done only in half of the hospitals (n=5) and additional radiographic images were taken during ERCP in seven hospitals (Fig.
2).
Magnification mode seems to be quite common in the ERCP.