RESULTS
Of the 1245 vacuum-assisted biopsies,
45 yielded FEA (3.6 %).
Thirty-four of 45 FEA were obtained under stereotactic guidance (75 %) and 11 under sonographic guidance (25 %).
Clinical Findings
The average patient age was 49 years (range,
37-67 years).
FEA was found during the staging of a synchronous cancer in the same breast in two patients.
One patient had a history of previous cancer in the contralateral breast.
Six patients had familial history of breast cancer.
Six of the 45 lesions were palpable.
Imaging Findings
All 45 patients underwent a mammogram and 13 patients an ultrasound as well.
Mammography
Mammographic breast composition displayed a type 4 pattern (extremely dense) in two of 45 patients (4.4%),
a type 3 pattern (heterogeneously dense) in 22 patients (51%),
a type 2 pattern (scattered fibroglandular densities) in 18 patients (40%),
and a type 1pattern (fatty) in two patients (4.4%).
In one patient mammogram could not be reviewed because it was performed at another institution.
On mammography,
42 flat epithelial atypia lesions were visible,
and 3 were occult.
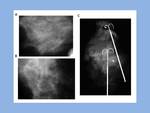
Flat epithelial atypia appeared as microcalcifications in 31 of the 45 lesions (69 %),
as a mass without calcifications in 5 lesions (11%),
as a mass with calcifications in one lesion (2%),
as a distortion without calcifications in two lesions (4.5%),
as a distortion with calcifications in one lesion (2%),
as an asymmetry with calcifications in one lesion (2%) and as a asymmetry without calcifications in one lesion (2%).
Thirty of the 31 cases of microcalcifications were BIRADS 4 (6 BIRADS a,
11 BIRADS b and 12 BIRADS c),
and one was catalogued as BIRADS 5.
In one patient BIRADS classification could not be assigned because mammogram was performed at another institution.
The distribution according BIRADS for the rest of 11 also lesions visible on mammography was as follows: one case of BIRADS 2 (a hialinized fibroadenoma),
four BIRADS 3 and six BIRADS 4 (1 BIRADS a,
2 BIRADS b and 3 BIRADS c).
The mean lesion size of the 42 lesions seen mammographically was 1.3 cm (range,
0.3-4.0 cm).
Sonography
Sonography was performed in 13 lesions: nine masses,
three distortions and one asymmetry.
Among these,
all lesions except three masses had a mammographic correlation.
Most masses displayed and oval shape (9/13 [69%]),
with circumscribed margins (7/13 [54%]) and hypoechoic echotexture (7/13 [54%]).
For the three lesions only visible on sonography,
one was classified as BIRADS 3 and two as BIRADS 4a.
The mean lesion size of the 13 lesions was 1.7 cm (range,
0.8-3.5 cm).
Imaging-guided Needle Biopsy
Of the 45 lesions biopsied,
32 (71%) were visible on mammogram only (all cases of microcalcifications and one case of asymmetry with microcalcifications) and were biopsied under stereotactic guidance,
eight (6 masses and two distortions: 18% ) were seen on mammogram and ultrasound and biopsied under ultrasound guidance,
two (one distortion and one asymmetry: 4%) were seen on mammogram and ultrasound and biopsied under stereotactic guidance and three (three masses: 7%) were seen only on ultrasound and biopsied under ultrasound guidance.
With respect to stereotactically VAB of microcalcifications,
complete removal was achived in 35% (11/31).
In another 16% (5/31),the percentage of microcalcifications removed was more than 75%.
Assesment After Imaging-Guided Biopsy
Surgical Excision
Twenty-six of 45 patients (58%) underwent surgical excision without a follow-up interval.
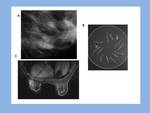
Surgical pathology confirmed the diagnosis of FEA in eight cases (31%)(Fig.3).
Atypical ductal hyperplasia (ADH) was found in six lesions (23%),
lobular neoplasia in four lesions (15%) and five cases proved to be benign at excision (19%).
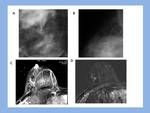
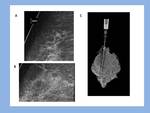
Surgery revealed two cases of DCIS (8%) and one case of infiltrating ductal carcinoma (IDC) (4%)(Fig.4,5 y 6).
The three cases of carcinoma were large groups (2.7,
3.5 and 4 cm) of microcalcifications BIRADS 4c biopsied under stereotactic guidance.
One patient had history of previous cancer in the contralateral breast.
In all cases the percentage of microcalcifications removed was less than 75%.
Follow-up
In nineteen lesions (42%),
an imaging follow-up was decided.
One of them,
a mass of 1.3 cm biopsied under sonographic guidance,
underwent surgical excision ten months later because after a complete excision,
a sonographic evaluation revealed a new 0.5 cm mass at site of biopsy.
Surgery yielded FEA.
The other eighteen patients underwent a minimum 2 years´ imaging follow-up (27 -76 months),
with no significant change documented.