Procedure details
Technique of multidetector computed tomography angiography (MDCTA)
In our institution MDCTA are performed on a 64-slice scanner (LightSpeed VCT,
GE Healthcare,
Milwaukee,
USA).
Patients are placed in a supine position with their legs and their feet held together without tapes.
1. First of all it is necessary to talk to the patient and ask which leg hurts more and/or sooner when at rest and/or walking.
2. Anteroposterior and lateral scout images are then obtained from the dome of the diaphragm,
or from the head (when the neck and thorax are also acquired),
to the toes.
3. First the bolus-test slice (SmartPrep,
GE Healthcare) is placed on the ankle at a level located 2cm proximal to both malleolus.
4. Then we proceed with the injection of small quantitative of contrast material for bolus test: 20ml of contrast media (320-400 mg Iodine/ml) at 4ml/sec followed by 40 ml of saline flush at 4ml/sec.
The bolus test technique allows the exact assessment of the time needed by the contrast media to reach the ankles.
The bolus test has to be assessed visually by the technician or radiologist since the distal vessels are too small to place a ROI,
furthermore in PAD patients the ROI may be placed in a vessel that in fact is occluded.
Knowing the delay time that contrast material needs to reach the ankle and,
calculating from the side with the longer delay (usually the side that the patient has indicated),
we add 5/10 seconds for appropriate assessment of the distal feet vessels.
We add 5 or 10 seconds according to the delay needed by the bolus test to reach the ankle,
when longer delays from the injection time are needed (>45 seconds) we add 10 seconds for optimal depiction of the feet vessels.
5. The CT acquisition start timing,
knowing the true individual for each patient delay of peak peripheral enhancement,
can be easily calculated subtracting from the bolus test delay+5/10 seconds the MDCTA acquisition scan time,
using the following formula:
(BT delay+5/10s) - MDCTA acquisition scan time = Delay,
after contrast media injection start,
of CT scan time start.
At this point in some cases when the delay needed by the contrast media to reach the feet is important (>50 seconds) it is necessary to slow down the acquisition time of the CT.
The objective is to start the CT acquisition time at latest about 30/40 seconds following contrast media injection to have a good and homogeneous arterial phase from the start (neck vessels or upper abdomen) to the feets.
6. In our institution the 64-slice MDCTA (VCT,
GE) scan protocol is defined within the main following parameters:
Table 1.
Scan protocol
|
kV
|
100/120
|
|
mA
|
150/500 with automatic in plane and Z exposure correction
|
|
Gantry rotation time
|
0,4 - 0,7s
|
|
Table movement
|
34/55mm for tube rotation
|
|
Scan Time
|
12 - 35s
|
7.
Once the acquisition time is defined and the delay known it is however useful to use a Smart Prep slice at the level of the upper abdominal aorta or thoracic aorta to check the correct arrival of the contrast media bolus.
8.
Finally the real exam contrast media bolus is injected and the MDCTA acquisition is obtained with an average of 120ml of contrast media (320-400mg Iodine/ml) injected at 4ml/sec followed by 40ml of saline flush at 4ml/sec.
9.
Depending on the clinical context a further portal phase of the abdomen (or other phases as needed) can also be planned to allow better assessment of liver parenchyma.
Depending on the user experience the scan room time for patient is about 15 minutes,
the time needed to optimize with the bolus test the CT acquisition is in our opinion justified by a better and faster manipulation (Volume rendering,
Maximum intensity projection,
MPR,
automatic arterial run off softwares) and interpretation of the MDCTA.
Imaging Findings
Normal arterious vessels anatomy of lower limb
Our technique allows minimizing the contrast enhancement of venous vessels,
therefore a straightforward analysis of lower limbs vessels with automatic programs is usually feasible.
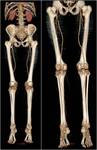
The normal anatomy is well known and anatomical variants are possible although rare Fig. 1 .
The anatomy to be known and followed in reporting in PDA studies is usually:
- Supraortic vessels,
thoracic aorta
- Abdominal aorta,
celiac trunk,
superior mesenteric artery,
renal arteries,
inferior mesenteric artery.
- Left run off: common iliac artery,
internal iliac artery,
external iliac artery,
femoral artery,
deep femoral artery,
superficial femoral artery,
popliteal artery,
anterior tibial artery,
common peroneal artery,
peroneal artery,
posterior tibial artery,
dorsal and plantar feet arteries.
- Right run off: common iliac artery,
internal iliac artery,
external iliac artery,
femoral artery,
deep femoral artery,
superficial femoral artery,
popliteal artery,
anterior tibial artery,
common peroneal artery,
peroneal artery,
posterior tibial artery,
dorsal and plantar feet arteries.
Findings obtained in patients with PAD
The delay for peak enhancement at the ankle level varies significantly within patients in our experience (range 30-90 seconds). Therefore it is necessary to tailor the CT acquisition to each patient transit time,
which is correlated with the PAD extension.
In emergency settings the bolus test technique is also feasible although time consuming and may be applied only in selected cases.
In some cases the depiction of the bolus test delay may be difficult,
particularly in those patients with diffusely calcified lower limbs arteries.
Diffuse calcification and stenosis of lower limbs arteries are particularly common in diabetic patients,
in some diabetic patients the assessment of the enhancement of the bolus test of contrast media in the heavily calcified vessel may be therefore problematic.
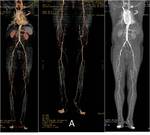
A cranio caudal approach can be usually followed in the assessment and reporting of MDCTA studies.
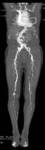
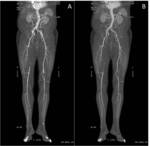
The scan extension as previously discussed can be optimized if necessary to cover the whole arterial system from the carotid arteries to the feet ( Fig. 2 and Fig. 3 ).
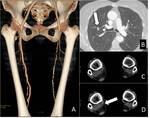
It is important to assess the subclavian arteries to rule out thrombosis that may be well associated with subclavian steal ( Fig. 4 ).
Patients with known or unknown aortic coarctation may as well undergo MDCTA studies for PAD ( Fig. 5 ).
If needed it is possible to perform with the same bolus test and the subsequent same contrast media complete bolus injection an evaluation of the coronary arteries (with cardiac gating) and of the abdomen and lower limbs arteries.
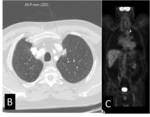
It is usually useful to extend the CT acquisition to the thorax (if not already requested by the referring physician); in some cases previously unknown pulmonary cancers may be found since PAD patients often have a smoking history ( Fig. 6 ,
Fig. 7 ; Fig. 8 ).
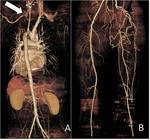
Thoracic and/or abdominal aneurysm increase the delay needed by the contrast media to reach the feet,
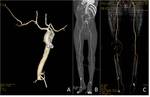
with our bolus test the correct timing even in these patients is possible ( Fig. 9 ).
Abdominal aneurysms following endovascular repair and all the arterial run off may be well shown ( Fig. 10 ).
Particular difficult to assess are patients with Leriche Syndrome (occlusion of the abdominal aorta) in these cases the bolus test technique allows as well the correct timing of CT acquisition ( Fig. 11 ).
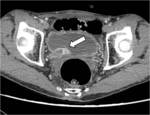
Bladder tumors are easily imaged as well as incidental findings in patients undergoing PAD assessment,
it has to be noticed that the bolus test gives a small urographic phase that is then depicted in the arterial acquisition of the MDCTA ( Fig. 12 ).
A common pattern of PAD is obstruction of the superficial femoral artery with collaterals at the obturator (Hunter) canal ( Fig. 13 ).
Always,
and particularly in diabetic patients,
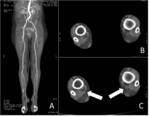
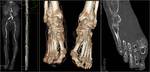
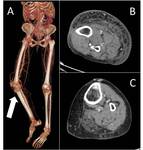
it is important to assess soft tissues and the bone as ulcers and osteomyelitis are of particular concern in patients with PAD.
Please note that in osteomyelitis because of the infection a faster transit time is present on the affected side with early venous enhancement ( Fig. 14 ).
As in osteomyelitis also fasciitis may cause hyperemia and faster venous return,
in these cases it is difficult to avoid venous contamination ( Fig. 15 ).
In diabetic patients the bone has to be assessed not only for osteomyelitis but also for diabetic arthropathy ( Fig. 16 ).