The primary aim of a breast screening programme is to reduce mortality from breast cancer through early detection.
The key factors necessary to achieve this goal,
are a high acceptance by the target population,
and a high level of quality of the entire screening process.
The radiologist has a role of primary importance,
taking the greatest overall responsibility for mammographic image quality,
and diagnostic interpretation.
Although the efficacy of mammography is well documented,
its use as a modality for mass screening has recognized limitations.
Approximately 10%–20% of breast cancers are not routinely detected by mammography.
Interval cancers (IC) are defined as breast cancers arising after a negative screening episode and before the next scheduled screening round.
Interval cancers are inevitable in a screening programme,
but their number should be kept as low as possible because a high proportion of interval cancers will reduce the effectiveness of screening and the potential mortality reduction will be lowered.
The desirable rate of IC in a screening programme should be inferior to 1/1000 women screened.
Radiologists in each unit must ensure that a suitable mechanism exists for the audit of all interval cancers by reviewing the screening mammography (first without seeing the presentation mammograms taken at the time of diagnosis) in order to make a provisional classification,
and then reviewing the screening mammogram again together with the diagnostic mammogram to make a new and definitive classification which may be different to the provisional one.
We can classify interval cancers in one of the following categories ( Table 1):
Unclassified (NC): mammography was not performed at the time of diagnosis or symptomatic mammograms were not available at review and therefore the presence of mammographic signs of malignancy cannot be verified.
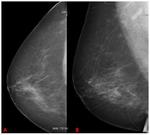
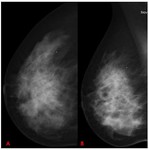
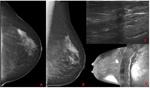
Occult interval cancer (OIC): neither the screening mammogram nor the mammograms performed at the time of diagnosis demonstrate any abnormality that could be interpreted as representing malignancy ( Fig. 1 Fig. 2)
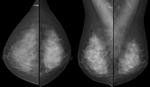
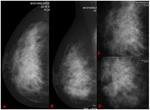
True interval (TIC): The screening mammogram is normal,
no reason for assessment ( Fig. 3 Fig. 4 ).
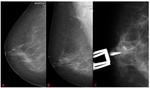
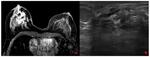
Minimal signs (MS): There is a possible subtle abnormality on the screening mammogram.
This would not necessarily be regarded as warranting assessment.
A brief description of the lesion and its position should be noted ( Fig. 5 Fig. 6 Fig. 7 ).
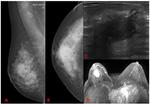
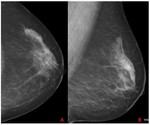
False negative (FN): An abnormality is clearly visible and warrants assessment.
Description and position should be given.
This category shouldn´t represent more than 20% of all IC ( Fig. 8 Fig. 9 ).
Our purpose is to retrospectively evaluate the IC rate in our screening program in Cantabria (Spain) during the last three rounds (2007-2012),
its classification according the four subtypes (true interval,
false negative,
minimal sign and occult interval cancer) and its distribution according to mammogram modality: analogue,
direct digital and indirect digital.