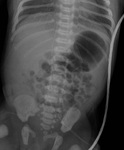
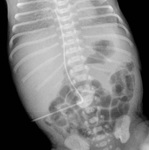
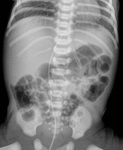
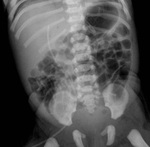
UVC are commonly used in the neonatal period; they can be not correctly positioned and may be associated with significant complications [1]
UVC can be misplaced in various vascular structures as: the superior mesenteric vein,
splenic vein,
superior vena cava,
and internal jugular vein or the left atrium through a patent foramen ovale.
If the UVC perforates an intrahepatic vascular wall,
a hepatic hematoma may result [2].
Because usually fluids are administered through the UVC malposition may arise in extravascular fluid collections.
If the UVC tip reaches the left portal vein but does not continue into the ductus venosus,
the catheter can travel left into the more peripheral left portal vein or right,
where it can eventually course into the right portal vein or hepatofugally into the main portal vein (or potentially farther into the vessels that merge to form the portal vein: the superior mesenteric and splenic veins)[3].
The UVC can also perforate the right or left atrial wall and enter the pericardial space.
Thromboembolic complications of catheterization with UVC in neonates have been well documented [4,
5].
Prenatal anatomy
The right umbilical vein disappears by 6 weeks gestational age.
The left umbilical vein passes upward along the free margin of the falciform ligament.
At the porta hepatis,
it divides into two branches.
The larger is joined by the portal vein,
and the smaller branch continues cranially as the ductus venosus.
The ductus venosus is 1-2 cm long and ends in the left or middle hepatic vein,
very chose to the junction with the inferior vena cava [6].
Blood entering the right atrium is directed toward the foramen ovale by the valve of the inferior vena cava.
The lower bonder of the septum secundum deflects the flow into two unequal streams.
The lesser flow mixes with the venous return from the superior vena cava and passes through the right ventricle,
from where it passes to the pulmonary artery,
ductus arteniosus,
and descending aorta and returns to the placenta through the umbilical artery.
Little blood passes to the lungs because of the high pulmonary vascular resistance.
The main or larger stream passes through the foramen ovale to the left atrium,
mixes with any blood returning from the lungs,
and enters the left ventricle.
The blood passes through the ascending aorta to the head,
neck,
and upper limbs [7].
Post-natal anatomy
The proximal portion of the umbilical artery remains patent and branches into the superior vesical arteries.
The distal part of the umbilical artery extends from the sides of the bladder to the umbilicus.
The artery,
along with the urachus,
becomes obliterated between the 2nd and 5th days after birth,
and they persist as fibrous cords covered with peritoneum,
the medial umbilical ligaments.
The umbilical vein forms the ligamentum teres hepatis in the lower margin of the falciform ligament.
The ductus venosus forms the ligamentum venosus of the liver,
and the ductus arteriosus forms the ligamentum arteniosum,
which connects the left pulmonary artery to the arch of the aorta.
Increasing pressure in the left atrium presses the septum primum against the septum secundum and closes the foramen ovale [7].
The major aortic branches arise at the following vertebral levels (even though there is
considerable variation) : the celiac trunk at T12,
the superior mesenteric artery at T12 to L1,
the renal artery at L1 to L2,
the inferior mesenteric artery at L3,
and the aortic bifurcation at L4.
The single umbilical vein extends from the umbilicus to the left portal vein and initially maintains an anterior,
midline location in the anterior abdominal wall until it courses posteriorly through the liver to the left portal vein.
There is a focal dilatation of the umbilical vein just before its junction with the left portal vein: the umbilical recess [8].
When blood from the umbilical vein reaches the left portal vein,
it is directed to the ductus venosus,
which originates from the left portal vein immediately opposite the insertion site of the umbilical vein and courses cephalad to the inferior vena cava.
In contrast,
the typically paired,
bilateral umbilical arteries initially course posteriorly and caudally to enter the right and left iliac arteries.
Therefore,
the UVC and the umbilical artery catheter can be easily distinguished on abdominal radiographs: the UVC predominantly follows an anterior and cephalad course in the midline umbilical vein until directed posteriorly in the liver,
whereas the umbilical artery catheter is initially directed caudally and posteriorly to enter either the right or left iliac artery before coursing superiorly in the more posteriorly positioned aorta.
Normal Vascular Course of Umbilical Venous Catheters and Normal Radiographic Appearance
In newborn,
the umbilical vein is about 2-3 cm in length; it leads to the left portal vein,
then to the ductus venosus that shunts blood flow directly to the inferior vena cava (IVC).
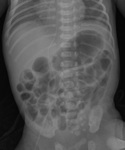
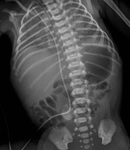
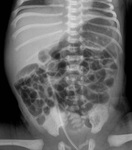
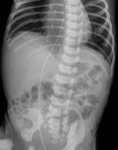
On frontal radiograph,
the UVC is placed on the right of lumbar spinous processes (L3-L4),
it courses posteriorly through the liver (D10-D12) to the left portal vein and then to ductus venosus and IVC (D9) (Fig.2).
To evaluate the UVC placement,
we have to consider its course and tip location,
ideally placed in the atrio-caval junction or in the proximal portion of the IVC (D8-D9).
We summarized these key-points in the flow-chart (Fig.
1).
We asked 10 residents to evaluate the placement of 10 UVC (examples in Fig.3-9) before and after they familiarized themselves with the flow-chart and the anatomical findings.