This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Fistula, Embolisation, Contrast agent-other, Complications, MR, Lymphography, CT, Lymph nodes, Interventional non-vascular, Abdomen
Authors:
A. Witteler, N. Acar, A. M. Ranft, J. Altenbernd, T. Schwenzer, S. Rohde; Dortmund/DE
DOI:
10.1594/ecr2015/C-1442
Findings and procedure details
In a patient (age 63 years,
female) a radical hysterectomy and lymphonodectomy was performed due to uterine cervix carcinoma.
After surgery high amounts of chylous ascites and transvaginal loss of ascites (2000 ml/d) occurred.
Due to the catabolic situation as a result of the loss of lipids the intended chemoradiation could not be started and the postoperative recovery was delayed.
The initial conservative treatment was not effective.
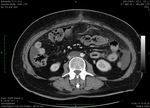
The postoperative CT scan (Fig.
6) showed a small fluid collection in the retroperitoneal space between the inferior V.
cava and the Aorta abdominalis.
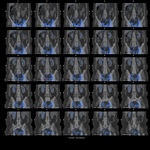
The lymph scintigraphy (Fig.
4 and 5) could not detect the location of the lymph fistula as there was a destruction of the iliacal lymph vessels due to the surgery.
Therefore a classical lymphography was not performed.
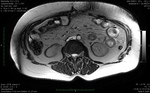
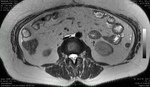
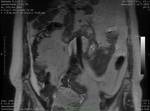
The abdominal MRI (Fig.
1-3) confirmed the retroperitoneal fluid collection,
but could not show the location of the leakage.
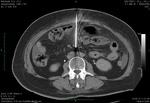
As an interdisciplinary decision a CT-guided puncture of the fluid collection was performed (Fig.
7 and 8).
A 17G-needle with a sharp inner needle was used to penetrate the abdominal wall.
For the passage of the peritoneal cavity the inner needle was exchanged to a blunt inner needle in order to avoid a damage to the mesenteric vessels and the intestine.
Directly anterior to the collection the sharp inner needle was reinserted for the puncture of the fluid collection.
The fluid that was aspirated was chylous fluid.
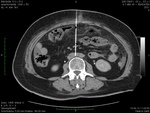
The injection of a small amount of contrast agent was performed (Fig.
9 and 10).
The delayed CT scans could show the location of the lymph fistula (Fig.
11 and 12).
As a first attempt occlusion of the fistula with a blood patch via the diagnostic needle was performed.
The ascites production and vaginal fluid loss was stopped for almost a week.
As the symptoms of the lymph fistula occurred again a new CT scan was acquired and showed again the lymphocele.
A surgical attempt to stop the fistula was not successful.
Therefore another CT-guided puncture of the fluid collection was done.
Via the needle the fluid was removed and a small amount of Ethoxysclerol and Histoacryl (mixed with Lipiodol (1/5)) was injected.
Afterwards the ascites production and the vaginal fluid loss were stopped and did not occur again.