We present the new use of Cone Beam Computed Tomography scanning to image the wrist in patients with Rheumatoid Arthritis as an alternative to Magnetic Resonance Imaging and plain film radiography.
Rheumatoid Arthritis (RA) is a chronic,
systemic,
inflammatory disorder of unknown aetiology that primarily affects the joints.
Left untreated,
the natural history of this arthritis involves progressive destruction of cartilage with bone erosions leading to significant deformity and physical disability.
Early diagnosis and aggressive treatment to achieve disease remission is imperative to prevent this outcome.
Despite this understanding,
~75% of RA patients exhibit erosive joint damage within 2 years of diagnosis.[1] Detecting bone erosions on imaging therefore has significant prognostic implications and should prompt the treating Rheumatologist to reconsider the Disease Modifying Anti-Rheumatic Drug (DMARD) regime.
Furthermore,
in undifferentiated inflammatory arthritis,
the detection of erosions predicts RA onset with a sensitivity of 100% and specificity of 78%.[1] Imaging of RA forms part of treatment planning and current options are plain film radiography,
Magnetic Resonance Imaging,
and occasionally conventional Computed Tomography.
Plain film radiography represents the historical gold standard for detecting bone erosions in RA,
however,
it is an insensitive modality detecting an abnormality only once 20-30% of the bone volume is lost.[2]
Magnetic Resonance Imaging (MRI) detects erosions involving <20% of bone volume loss.
This translates to erosions being visible on MRI a median of 2 years before being detected on plain x-ray.[3] However,
there are a number of limitations to the routine use of MRI to image RA.
In particular,
the availability of MRI is limited in the public hospital system.
Costs of MRI are generally high.
In addition,
a number of patient factors may contraindicate MRI including indwelling metallic devices and claustrophobia.
Conventional Computed Tomography (CT) has long been recognised for its ability to profile cortical bone.[1] It therefore follows that CT provides a sensitive modality with which to detect bone erosions in RA.
Conventional CT,
however,
is associated with a relatively high radiation dose compared to plain radiography.
Cone Beam Computed Tomography (CBCT) has been used for over a decade to obtain high resolution tomography of the dentition,
but only recently been introduced in a form that permits assessment of the extremity bones.
At five times less ionising radiation (1.7mGy,
with an effective dose of 0.0085mSv) and three times the spatial resolution of conventional CT,
it has the potential to be far more sensitive than plain x-ray for detecting bone erosions in RA,
without the logistic limitations of MRI,
and with similar order of magnitude radiation dose as plain film.
Fortunately,
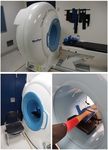
Austin Health Radiology is one of the few departments worldwide to possess one of these CBCT machines (Fig. 1).
CBCT of the wrist enables three plane,
isotropic voxel,
high spatial resolution (~70 micron) and low dose (1/5 conventional CT) imaging.
Our purpose was to assess performance of CBCT imaging of the wrist in patients with RA in detecting erosions compared to the current gold standard of Wrist MRI.
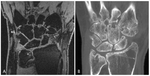
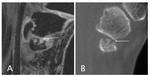
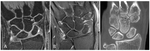
Figures 2-4 demonstrate the appearance of erosions using CBCT compared to MRI (Fig. 2; Fig. 3; Fig. 4).
No study in the current literature has documented the efficacy of CBCT in assessing erosions in RA.
This audit therefore aims to compare the images of a small number of RA patients who have already undergone imaging of the wrist with both CBCT and MRI.