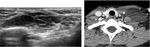
Appearance of Normal Thymus
Ultrasound
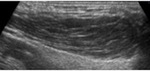
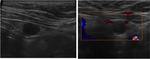
The thymus has a hypoechogenic and slightly heterogeneous echotexture.
In infants it shows multiple thin echogenic lines and branchings.
In older child and adults we identify multiple hyperechogenic foci which give to the thymus a distinct appearance that resembles a "starry sky".
(Fig 3)
In adults the thymic parenchyma may be more echogenic due fatty infiltration.
(Fig 3)
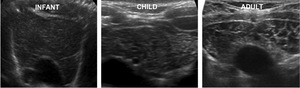
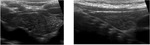
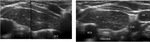
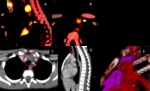
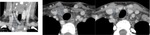
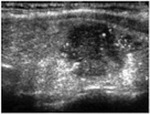
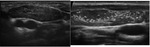
Fig. 3: Ultrasonographic images of a normal thymus in an infant, a child and an adult.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
Computed Tomography
The thymus size and shape can vary greatly even among individuals in the same age group.
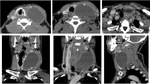
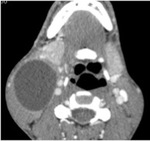
Thymus has a soft tissue density on CT images and usually presents with a triangular bilobed shape with straight or concave borders.
The bilobed shape can be better appreciated on coronal images.
(Fig 4)
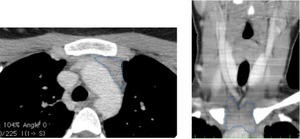
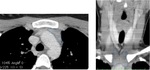
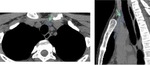
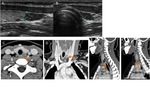
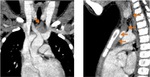
Fig. 4: Axial and reconstructed coronal CT images show the normal appearance of thymus (dashed line).
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
The cervical thymic anomalies can be classify:
1) Superior cervical extension of the thymus
2) Ectopic cervical thymic tissue
3) Cyst thymic
1) SUPERIOR CERVICAL EXTESION OF THE THYMUS
Superior cervical extension of the thymus corresponds to the presence of thymic tissue extending above the manubrium,
in the midline,
to the lower anterior cervical region.
This thymic tissue is in direct continuity with the mediastinal thymus.
It is a normal finding frequently observed in child and young adults.
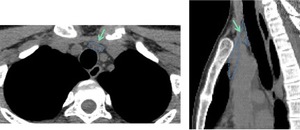
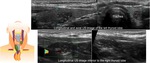
Fig. 5: Axial and reconstructed sagittal CT images of a 12 years old girl referred to our Department for the assessment of a mass in the thoracic inlet that appears when she coughs. A soft tissue elongated image extending above de manubrio, anterior to the trachea and in continuity with the mediastinal thymus was demonstrated, corresponding to a cervical extension of the thymus.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
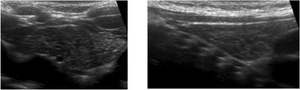
Fig. 6: Corresponding axial and longitudinal US images of the same patient presented in Fig 5, show the normal echotexture (“starry sky") of the cervical component of the thymus.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
The thymus is a very malleable tissue and does not cause compression or displacement of the adjacent vessels and airway (Fig 7).
This feature can be appreciated during sonographic examination; cardiac pulsations and respiratory motions may be transmitted to the thymus modifying its shape.
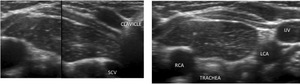
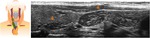
Fig. 7: Longitudinal and axial US images of a 9 months old girl referred to our department for the assessment of an anterior cervical mass . Images show the normal echotexture of the cervical component of the thymus. No displacement or compression of the adjacent structures is observed.
(SVC: subclavia vein, RCA: right catotid artery; LCA: left caroty artery, IJV: intern jugular vein).
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
FDG accumulation in the thymus can be observed in young adults after chemotherapy.
The metabolic activity of the thymus in the first years to puberty and the occurrence of thymus hyperplasia after chemotherapy are possible causes for the FDG uptake.
Superior cervical extension is a frequent imaging finding and should not be misinterpreted as malignancy or metastatic disease.
(Fig 8)
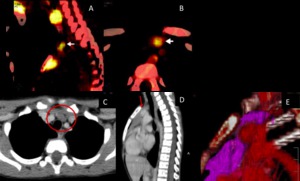
Fig. 8: Sagittal (A) and axial (B) PET-CT images of 28 years old man demonstrated a nodular FDG-uptake in the anterior lower neck in the midline region. Axial (C), sagittal (D) and tridimensional reconstructed (E) CT images after IV contrast demonstrated that the FDG-uptake corresponded to the superior extension of the thymus.
References: Courtesy of Dr Miguel Francisco Neto, Dr.Cristiane Wosny, Dr. Regina Lucia E. Gomes e Dr. Rodrigo Gobbo Garcia)
Although islands of residual functional tissue can be found in the thymus in histologic studies of older patients,
reactive thymus hyperplasia is a phenomenon observed specially among younger individuals.
It seems to be independent of the primary tumor histologic type and the chemotherapeutic regimen.
Among patients who undergo chemotherapy,
approximately 1/5 may develop reactive thymus hyperplasia.
FDG accumulation in the thymus is suspected to be related to a malignancy if the activity reaches the concentration in the bladder or cerebellum or if the thymus loses its characteristic shape.
It is imperative to interpret the imaging findings in the setting of clinical data.
2) ECTOPIC CERVICAL THYMIC TISSUE
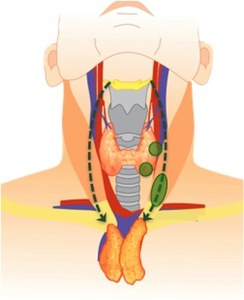
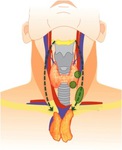
Fig. 9: Ectopic cervical thymic tissue frequent sites.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
Ectopic cervical thymic tissue is rarely reported in medical literature,
but it should be included in the differential diagnosis of neck masses,
especially in children.
Solid forms result from either a complete or partial interruption of the thymic primordia descent into the mediastinum or from sequestration and failure of involution of thymic remnants along the thymopharygeal duct path.
An entire thymic lobe (Fig 10 and 11) or some of its tissue (Fig 12) can be arrested in the cervical region.
Anatomically,
the arrested thymic tissue is usually in the lateral aspect of the neck.

Fig. 10: 15 years old female referred for evaluation of a cervical mass. Longitudinal US images show the “starry sky” appearance of the thymus. The ectopic thymic tissue has poor vascularization on US Doppler image.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
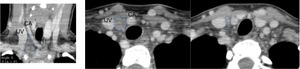
Fig. 11: Coronal and axial CT images after IV contrast agent in a 15 years old female. Ectopic cervical thymic tissue is identify in the right lower neck, between the internal jugular vein (IJV) and common carotid artery (CA) (dashed line).
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil

Fig. 12: (A and B) Longitudinal and axial US images show a hypoechogenic and slightly heterogeneous nodule with multiple hyperechogenic foci situated adjacent to lower pole of the left thyroid lobe in a 11 years old boy. (C - F) Corresponding axial, coronal axial sagittal CT images after IV contrast agent show a nodular soft tissue image adjacent to lower pole of the left thyroid lobe.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
In the differential diagnosis of the image in fig 12 was included: a enlarged parathyroid gland,
hypoechogenic thyroid nodule,
lymphadenomegaly and ectopic thymic tissue.
An ultrasound-guided fine needle aspiration (FNA) biopsy was performed to establish the diagnosis.
(Fig 13)
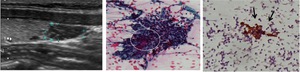
Fig. 13: Photomicrography of the FNA cytology demonstrated (A) numerous lymphocytes (thymocytes) and a large epithelial cell (circle). Cytokeratin immunostaining shows an epithelial cells intensely positive for cytokeratin, characteristic finding of the thymic epithelial cells (arrows).
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
Most of the ectopic cervical thymic tissue are unilateral,
more commonly reported on the left side and in male patients.
(Fig 14)
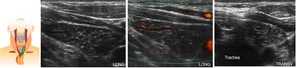
Fig. 14: 14 years old male. US images show ectopic thymic tissue in the left lower cervical neck (resembling a “starry sky”). The ectopic thymic tissue has poor vascularization on US Doppler image.
References: department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
Rarely ectopic thymic tissue can be identify into the thyroid gland (Fig 15,
16 and 17).
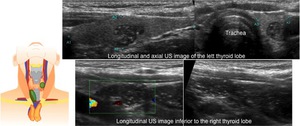
Fig. 15: The sonographic evaluation of a 7 months old boy demonstrated:
- Intrathyroidal ectopic thymic tissue in the left thyroid lobe
- Ectopic thymic tissue situated inferior to the right thyroid lobe
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
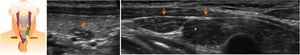
Fig. 16: Longitudinal US images in a 5 years old girl. Ectopic thymic tissue is identify in the posterior aspect of the left thyroid lobe. It is also demonstrated ectopic thymic tissue inferiorly of the left thyroid lobe. Notice that the ectopic tissue has the same echogenic pattern of the thymus.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
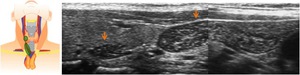
Fig. 17: Longitudinal US images in a 12 years old girl. Ectopic thymic tissue is identify in the posterior aspect of the right thyroid lobe. It is also demonstrated ectopic thymic tissue inferiorly to the right thyroid lobe. Notice that the ectopic tissue has the same echogenic pattern of the thymus.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
Ectopic thymic tissue can be found along the path of the thymopharingeal duct.
(Fig 18,
19 and 20)
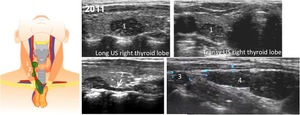
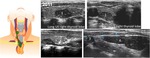
Fig. 18: Ectopic thymic tissue is identified inside the right thyroid lobe and along the path of the thymopharyngeo duct in a 5 years old boy. Intrathyroidal thymic tissue is attached to an inferior island of ectopic tissue by a band of thymic tissue (white arrow).
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
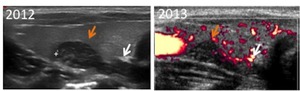
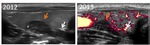
Fig. 19: Sonographic images of the same patient presented in Fig 18, performed one (2012) and two years (2013) after the first evaluation (2011), do not demonstrate size or morphologic changes in the ectopic thymic tissue.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
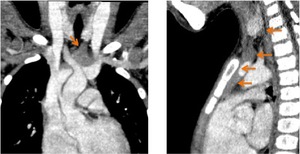
Fig. 20: Reconstructed coronal and saggital CT imagines demonstrate ectopic thymic tissue in the pathway of the thymopharyngeo duct. A continuous band of thymic tissue is identified extending from the anterior mediastinum to the posterior aspect of the left thyroid lobe.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
The following image (Fig 21) show a 131I whole-body scanning of a patient that underwent total thyroidectomy in the year of 2012 for papillary thyroid carcinoma in the left thyroid lobe,
with extracapsular invasion and a positive level VI lymph node.
The 131I whole-body scanning after surgery revealed an abnormal 131I uptake in the left cervical region (Fig 21).
CT images showed a soft tissue image exerting slight extrinsic compression in the left tracheal wall.
Residual thyroid tissue and central lymph nodes metastasis were considered in the differential diagnosis.
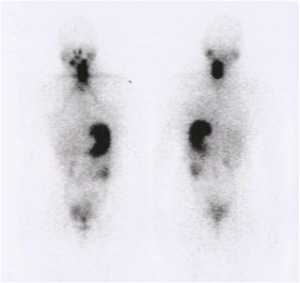
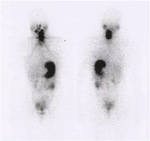
Fig. 21: 131I whole-body scanning revealed an abnormal 131I uptake in the left cervical region.
References: (Courtesy of Dr Marília D’Elboux Guimarães Brescia)
The patient underwent surgery.
It was demonstrated that the 131I uptake in the left cervical region corresponded to an ectopic thymic tissue.
(Fig 22)
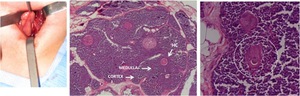
Fig. 22: Photomicrographs of the surgical specimen demonstrated the two anatomically and functionally distinct regions in the thymus, the outer cortex (more darkly staining region) and and the inner medulla (lighter staining region). The cortex stains more darkly than the medulla, because it contains more lymphocytes (thymocytes).
Hassall’s corpuscles (circle) are a characteristic feature of thymic medulla. These structures are only found in the thymus and are composed of a concentric arrangement of flattened thymic epithelial cells. The center of Hassall’s corpuscles is keratinized.
References: (Courtesy of Dr Marília D’Elboux Guimarães Brescia, Dr Adriano Ibrahim Asse Lopes)
The main differential diagnosis of he ectopic cervical thymic tissue include:
- Enlarged parathyroid (Fig 23): It can be found in the same location.
At US images usually presents more homogeneous and has high vascularity on US Doppler images.
- Thyroid nodule (Fig 24): Intrathyroid thymic tissue is usually identified in infant and younger children while thyroid nodule are more frequently found in adults.
Ectopic thymic tissue has the same echogenic pattern of the normal thymus.
- Lymphadenopathy (Fig 25): Usually there is more than one enlarged lymph node.
- Lipoma (Fig 26)
3) CERVICAL THYMIC TISSUE
The pathogenesis of cervical thymic cyst remains controversial. Segments of the thymopharingeal duct may persist as vestigial cavitary formation.
These vestigial structures are lined by epithelial cells.
Persistence of the thymopharyngeal duct remnants is the most commonly accepted theory regarding the pathogenesis of the thymic cyst within the head and neck region.
Alternatively,
some investigators believe they are acquired originating from cystic degeneration of Hassall corpuscles and the epithelium reticulum of the ectopic thymic tissue.
Cervical thymic cysts are usually considered congenital and detected during the first two decades of life.
They are more common in male and usually present as a slow growing,
painless mass.
Cervical thymic cysts can be located anywhere from the pyriform sinuses to the anterior mediastinum,
although they are more frequently found in the left side and the lower half of the neck (Fig 27).
Approximately 50% of all cervical thymic cysts extend into the mediastinum (Fig 28).
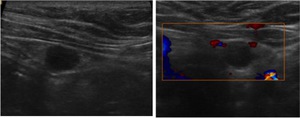
Fig. 27: Longitudinal and axial US images show a anechoic unilocular cyst situated in the thoracic inlet on left.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
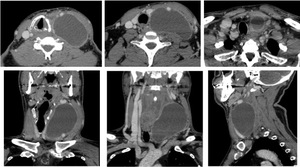
Fig. 28: The axial, coronal reconstructed and sagittal recontructed CT images after IV contrast administration showed a large, unilocular, cystic mass medial to the carotid space and ECM with extension into the superior mediastinum. After IV contrast administration there is a thin peripheral rim of enhancement that can be present in thymic cysts.
References: Department of Radiology, Clinics Hospital, University of São Paulo, SP, Brazil
The main differential diagnosis include:
- Branchial cleft cyst (Fig 29): it is usually situated in the upper half of the neck.
It can be found in the same location,
but rarely extends to mediastinum.
Also signs or symptoms of inflammation are frequently present.
- Thyroglossal duct cyst: it almost always found in the midline,
at the level or below hyoid.
It is usually smaller than thymic cyst.
- Cystic hygroma (Fig 30): usually lateral in location,
tends to be more difuse,
soft in consistency and it is seen early in infancy.