The sonographic evaluation of the liver starts with the analysis on B-mode of it's margins,
size,
echotexture and the study of the hepatic veins and retro-hepatic inferior vena cava (IVC).
In the acute form of Budd-Chiari ultrasound shows hepatomegaly and ascites.
If non diagnosed and succesfully treated,
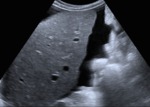
with time the liver develops signs of chronic hepatopaty such as blunt edges,
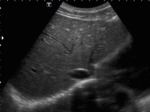
jagged outline and heterogeneous echotexture (fig.1) with signs of portal hypertension (increased diameter of portal,
splenic and superior mesenteric veins,
ascites and splenomegaly).
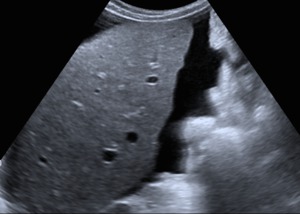
Fig. 1: B-mode ultrasound. Longitudinal view of right liver's lobe, which presents blunt edges, irregular margins, mild heterogeneous ecotexture and is surrounded by ascites.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
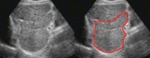
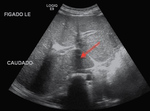
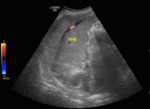
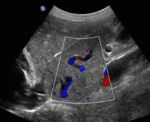
As the segment I (caudate lobe) has an independent vein drenage it is spared from the disease process and becomes hypertrophied (fig.2 and 3) to compensate for the loss of normal liver parenchyma, while the other segments suffer from the drenage impairment.
This caudate's hypertrophy is also observed in other types of hepatic diseases.
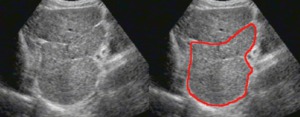
Fig. 2: B-mode ultrasound. Longitudinal view of the lateral segment of the left lobe and segment I (delineated in red), separated by the fissure of venous ligament. In this image a large (hypertrophied) segment I is seen.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
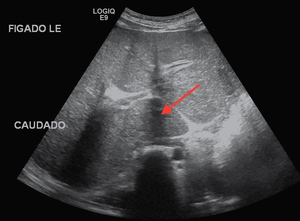
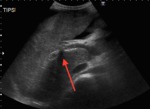
Fig. 3: B-mode ultrasound - subcostal view. The red arrow points to a prominent segment I.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
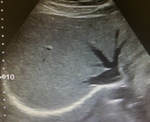
A scan is performed to evaluate the three hepatic veins (right,
middle and left) and it's anatomical variations in all their extension,
both on B-mode (fig.4 and 5) and color Doppler (fig.6).
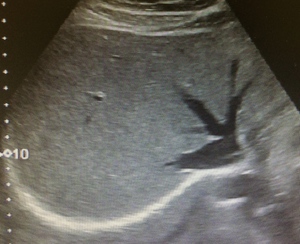
Fig. 4: B-mode ultrasound. Oblique view of the upper part of the liver demonstrate the normal (and typical) confluence of the three major hepatic veins into IVC.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
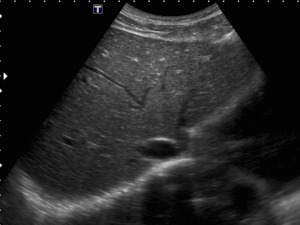
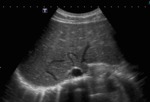
Fig. 5: B-mode ultrasound . Subcostal view of the liver showing the section in which it would be expected the confluence of the hepatic veins into the inferior vena cava (ICV). Only the left vein is slighted depicted, with a reduced caliber.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
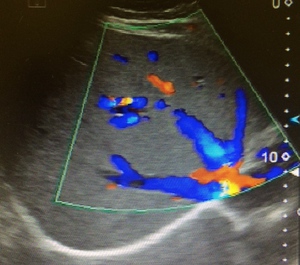
Fig. 6: Color Doppler ultrasound. Normal confluence of the three major hepatic veins into the cava vein. A mainly antegrade (to the heart), multi-phasic, homogenous flow is seen with patent veins in all extension (not demonstrated).
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
In Budd-Chiari the Doppler assessment shows the absence of flow in one or more hepatic veins,
partially or enterily,
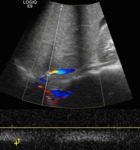
which contains hypoechogenic material (thrombus) and a maintained or slight increased calibre (fig 7) in the acute form.
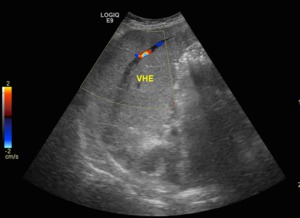
Fig. 7: Color Doppler ultrasound. Longitudinal view of liver's left lobe. Hypoechogenic material is seen in most of the left hepatic vein's lumen (partial thromboses). Note that the velocity rate is set at an extremely low rate.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
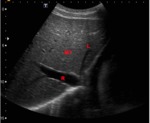
In the chronic form the obstructed hepatic veins shows a small calibre with no flow and sometimes are not well seen (fig 8).
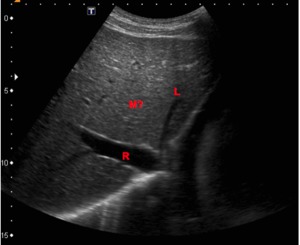
Fig. 8: B-mode ultrasound (subcostal view of the liver). Although the right hepatic vein is normal (red "R"), the left hepatic vein (red "L") has a small caliber and in the normal anatomic place of the middle hepatic vein (red "M) nothing is seen.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
The spectral wave of the patent remaining veins is altered,
loosing the typical breath oscilation (fig 9).
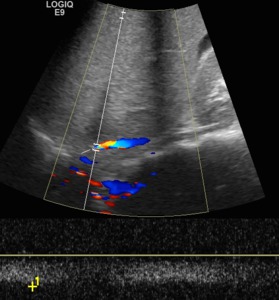
Fig. 9: Triplex Doppler ultrasound. Right parasagital view - longitudinal inferior vena cava posterior to the liver. A thin IVC is seen. Instead of the normal multiphasic spectral pattern (according to cardiac cycle and respiratory variation), a monophasic form is seen, resulting from thrombosis of two hepatic veins.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
Intrahepatic shunts are seen,
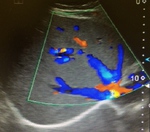
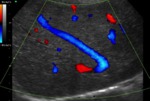
often in a "comma" shape (fig 10 and 11) which is a very classical feature in Budd-Chiari's disease.
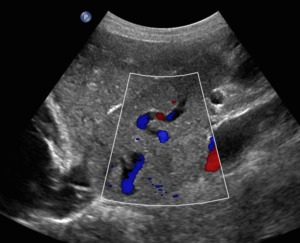
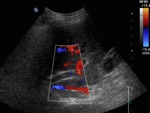
Fig. 10: Color Doppler - longitudinal view of the segment I. The curvilinear shape are typical in intra-hepatic shunts.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
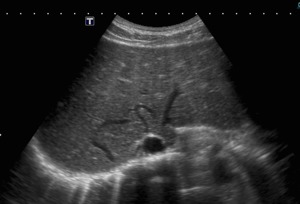
Fig. 11: B-mode ultrasound. The collaterals in "comma" shape near the cava vein are seen in this patient with complete blockage of the hepatic veins.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
Sometimes the collateral vessels can mimic a patent hepatic vein (fig 12),
which can be a pitfall.
These vessels drains to any other patent vein,
whether portal or systemic4.
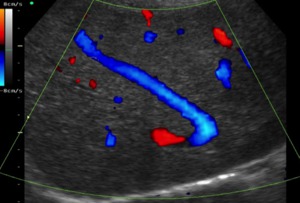
Fig. 12: Color Doppler ultrasound. In the subcostal view a colateral mimicking the middle hepatic vein is seen. Note that the vessel doesn't reach the IVC, instead it turns in a "hook" or "hockey stick" shape.
References: Marcelino ASZ, Chammas MC, Macedo TAA, Cerri GG. Anormalidades vasculares, in: Chammas MC, Cerri GG. Ultra-sonografia abdominal. 2th edition. Ed. Revinter. p143. Brazil
When vein port thrombosis also occurs in a patient with Budd-Chiari,
as a consequence of portal hypertension,
the prognosis is very poor.
In the treated Budd-Chiari,
if made early and successfully,
the liver shows no signs of pathology,
with reversal of hepatomegaly,
ascites and thrombosis.
In other cases it's seen a recanalization of some of the veins and the signs of liver disease can develop.
In case of TIPS treatment is important to check if the portal-IVC flow is patent and free.
TIPS impairments can mostly be due to break,
obstruction (fig 13) and stenosis (fig 14 and 15).
In B-mode the aspect of the TIPS is checked and with Doppler direction of flow and velocities are analised.
The normal findings in a TIPS are: pulsatil flow,
similar velocities whithin the TIPS and the direction of the flow should go from the portal branch to the stent.
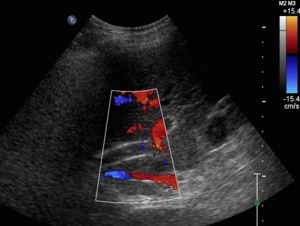
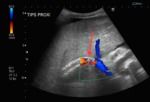
Fig. 13: Color Doppler ultrasound. Despite the low velocity scale, absence of flow is seen inside the TIPS. The normal velocity in a TIPS ranges among 90-190cm/s.
References: Instituto de Radiologia - Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo - Brazil
As an alternative treatment to more severe cases a liver transplant can be performed.
In this case the follow up is the same as in any other liver graft.