Anatomy of the major salivary glands
The paired parotid,
submandibular and sublingual glands make up the major salivary glands.
Further minor salivary glands are found over the palate,
lips,
cheeks,
tonsils and tongue.
2
The parotid glands are the largest salivary glands and secrete only serous fluid.
Each gland is positioned between the ramus of the mandible and the styloid process, with the duct opening lateral to the second upper molar tooth.2 The internal jugular vein,
external carotid artery and facial nerve traverse through the gland.
The gland can be divided in to superficial and deep lobes by drawing a line from the posterior aspect of the mandibular ramus to the mastoid process.
As the parotid develops it is encapsulated in the second trimester of pregnancy and incorporating lymphatic tissue,
therefore lymph nodes can be seen within the parotid parenchyma.
The other salivary glands do not contain lymph nodes,
however lymphocytes are encountered.3
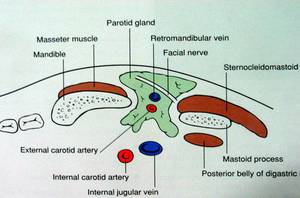
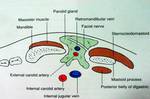
Fig. 1: Anatomy of the parotid gland in axial section
References: Ahuja, A. T., & Evans, R. M. (Eds.). (2000). Practical head and neck ultrasound. Cambridge University Press.
The submandibular glands are found along lingual surface of the body of the mandible,
palpable inferolaterally to mylohyoid.
The duct is around 5cm long and runs between the mylohyoid and hyoglossus muscles.2
The sublingual glands are the smallest of the major salivary glands,
found deep within the sublingual space between the genioglossus muscle and mandible.2 Each gland has between 8-20 small ducts which open either side of the frenulum.
Several of the ducts may also have a common drainage pathway with the submandibular duct.
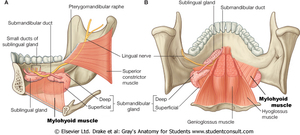
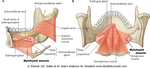
Fig. 2: Anatomy of the submandibular and sublingual glands
References: Elsevier Ltd. Drake et al: Gray's Anatomy for Students. www.studentconsult.com
Ultrasound assessment of the major salivary glands
The glands are best visualised with a high frequency transducer (10-15MHz) with assessment in two perpendicular planes.
In addition, a curvilinear lower frequency (5-10MHz) can be used to assess the deep aspect of the parotid gland.
The submandibular duct is best assessed firstly in a coronal plane with the probe perpendicular to the mandible.
In this position the mylohyoid and hyoglossus muscles can be identified. The probe is then turned parallel to the mandibular body, providing an ideal position along the submandibular duct as it runs between the mylohyoid and hyoglossus muscles.
Tip: The lingual vein can be easily mistaken for the submandibular duct as it runs in the same plane.
Ensure that any tubular structure does not have flow in it and cannot be followed past the gland.
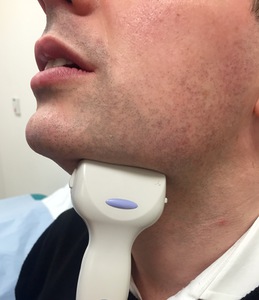
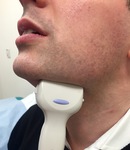
Fig. 3: Ultrasound probe position for visualisation of the submandibular duct.
The use of a sialogogue can be particularly useful in assessment of the ducts (Fig. 4).
Care should be taken when scanning to apply very gentle pressure so not to obscure a dilated duct.
The patient can also be asked to 'blow out the cheeks' to improve the view of the parotid duct opening and visualise a stone within the duct.
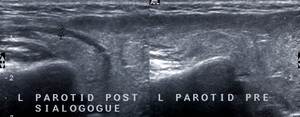
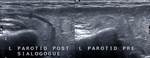
Fig. 4: Parotid gland duct post and pre sialogogue
Benign Pathology of the Salivary Glands
Sialolithiasis
The clinical history is usually of recurrent pain and swelling of the affected gland,
particularly before meals.
80% of salivary stones are found within the submandibular gland,4 of which 80-90% are radiopaque.
The submandibular gland is more prone to stone formation because of the alkaline nature of the saliva which is thick and viscous,
and also due to the dependent position of the gland.3
20% of calculi are found in the parotid gland,
of which 50% are radiopaque.4
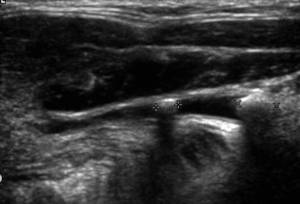
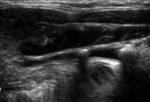
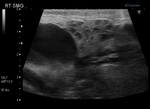
Fig. 5: Ultrasound of the submandibular duct demonstrating two ductal calculi with posterior acoustic shadowing
Tip: 25% of patients with stones will have multiple calculi,
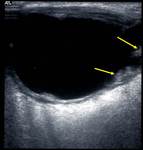
therefore it is important to assess both sides ( Fig. 5, Fig. 6 ).3
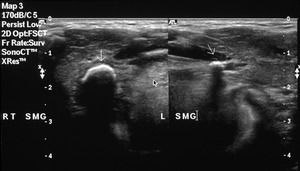
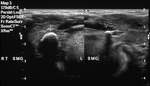
Fig. 6: Ultrasound of both submandibular glands demonstrating bilateral calculi (arrows)
Tip: Ductal dilatation can also be cause by a stricture or an obstructing mass lesion.
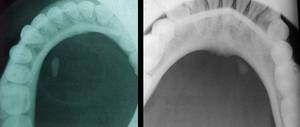
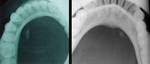
Fig. 7: Plain occlusal radiographs demonstrating distal submandibular duct stones
It is possible to demonstrate distal ductal calculi with plain film radiographs which may be difficult to visualise with ultrasound ( Fig. 7 ).
Sialadenitis
Acute:
Acute bacterial sialadenitis presents as a painful swelling commonly associated with purulent discharge.
Most commonly caused by oral Streptococci,
anerobes and Staphylococcus aureus,
potentially with areas of focal abscess formation4.
The symptoms are almost always unilateral.
Viral infection primarily affects the parotid causing pain,
fever and swelling,
and most commonly due to mumps.
Infection results in unilateral then bilateral swelling ( Fig. 8 ).
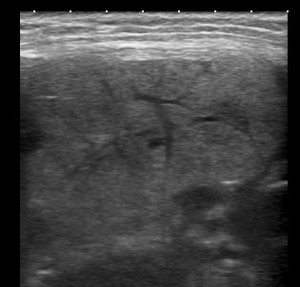
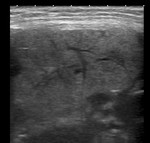
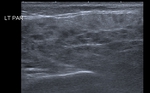
Fig. 8: Ultrasound of the left submandibular gland demonstrating acute sialadenitis
Chronic / Recurrent:
Chronic infection may be due to poor oral hygiene or secondary to chronic inflammation,
for example as a result an obstructing stone or stricture.
The salivary gland appears small and hypoechoic.
This is also observed in the frail elderly population who are prone to dehydration.
Recurrent disease results in ductal dilatation and ballooning of the alveoli called sialectasis.
Systemic disease - Sjögren's Disease
Sjögren's is an autoimmune disease which affects the secretory glands,
resulting in a dry mouth and dry eyes.
It affects women nine times more often than men.
On ultrasound the salivary glands may be enlarged,
having hetergenous appearance with multiple small areas of hypoechogenicity,
Fig. 9.
Labial gland biopsy is commonly used for diagnosis and demonstrates lymphocytic infiltrates.
Tip: Patients with Sjögren's have 5% risk of lymphoma arising within the gland.
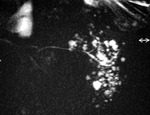
Sjögren's produces a characeristic appearance on sialogram with multiple ductal system cavities, Fig. 10.
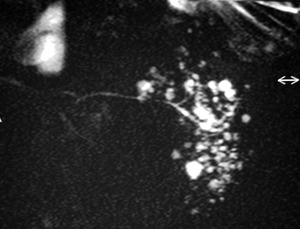
Fig. 10: MR sialogram - Sjogrens syndrome
Systemic disease - HIV
Severe immunodeficency presents in the salivary glands,
commonly associated cervical lymphadenopathy.
Patients present with diffuse salivary enlargement,
mixed solid and/or cystic lesions and both focal (parotid) and local (cervical) lymphadenopathy.
On ultrasound the salivary glands are enlarged with a hetergenous appearance and multiple cysts.
Multiple small areas of hypoechogenicity and small intra-glandal lymph nodes are also observed.
Cystic lesions
The majority of cystic lesions within the major salivary glands are benign.
However,
cystic lesions pose a diagnostic challenge where the walls of the lesion is irregular,
nodular or the lesion contains a solid component.
Frequently FNAC will be inaccurate if the wall is not appropriately sampled.
Underlying malignancy needs to be carefully considered.
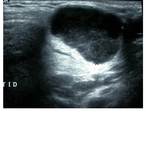
Tip: Always be suspicious of the cystic lesion in a salivary gland - mucoepidermoid tumours are the most common type of salivary malignancy and can be predominantly cystic, Fig. 13, Fig. 14.
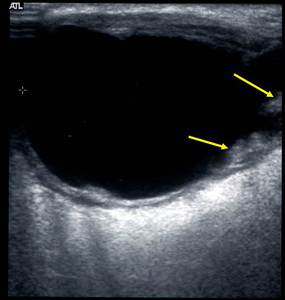
Fig. 13: Cystic lesion within the parotid gland (see also MRI), pathology proven mucoepidermoid tumour.
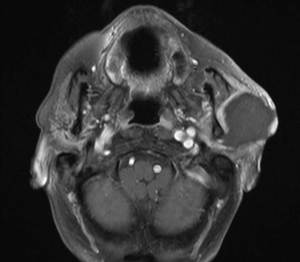
Fig. 14: Cystic lesion of the left parotid gland (see also ultrasound image), pathology proven mucoepidermoid tumour.
Ranula
A ranula is a mucocoele of the floor of the mouth arising from the sublinligual gland.
A 'plunging' ranula represents a lesion that extends deep to mylohyoid and presents as both an intra-oral and extra-oral swelling.
Benign parotid tumours
Tip: Remember the rule of 80% for benign salivary lesions
80% of salivary gland masses are benign
80% are found within the parotid gland
80% lie within the superficial lobe
80% are pleomorphic adenomas
Pleomorphic adenomas are usually lobulated,
well defined masses with a clear outline and posterior acoustic enhancement.
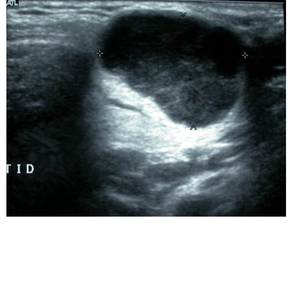
Fig. 12: Ultrasound parotid - Pleomorphic adenoma
If the lesion is large or poorly visualised MR can help to delineate the lesion.
Reassuring features on MR are
- A low signal rim
- Round/lobulated mass
- High signal T2
Of the remaining 20% of masses 10% are Warthins,
and of these 10-20% are bilateral.
Sialosis
Non-inflammatory swelling of the major salivary glands,
usually bilateral and most commonly affects the parotid.
Associated with endocrine abnormalities,
such as diabeties,
chronic alcohol abuse but often idiopathic.