This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Pathology, Neoplasia, Cancer, Vacuum assisted biopsy, Surgery, Ultrasound, MR, Mammography, Breast
Authors:
ďż˝. S. Okcu1, A. Oktay1, F. Can2, I. G. Bilgen3; 1Izmir/TR, 2Kutahya/TR, 3Bornova/TR
DOI:
10.1594/ecr2015/C-2515
Results
All 33 patients included in the study were female with a mean age of 53 years (range 25 to 77 years).
High-risk lesions diagnosed in these cases were ADH in 16 (4.09%),
intraductal papilloma in 12 (3.06%),
CCL in 4 (1.02 %) and LN in 1 (0.25%) as showed on Figure 1.
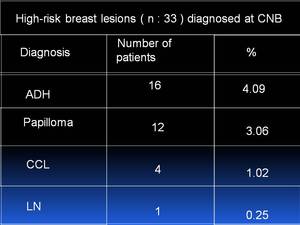
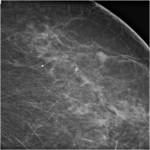
Fig. 1
21 patients (63.6 %) proceeded to excisional biopsy.
10 of them (47.6 %)upgraded to malignancy afterwards while 11 (52.3%) remained to be benign (Fig.2). 9 of the 10 malignancy-upgraded lesions were diagnosed as DCIS/IDC.
The last one upgraded to LN.
Of 11 lesions which did not upgrade to malignancy,
7 were diagnosed as papilloma,
2 were as CCL and 2 were as FBD.

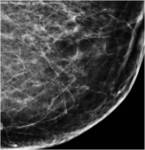
Fig. 2
Of 12 patients scheduled for imaging follow-up,
4 (12.1 %) were lost to follow-up. These were ADH in 2 patients and CCL in 2 patients.
1 of CCL patients was diagnosed with IDC,
3 years later. 8 patients (24.2 %) were followed-up for an average of 26 months either with mammography or US depending on which modality detected the lesion.
Lesion stability was confirmed in 7 patients (2 patients with CCL,4 patients with papilloma and 1 patient with ADH).
Only 1 patient in this group was operated on the sixth month of follow-up,
due to rapid growth and the final diagnosis was benign papilloma.
These findings are summarized on Figure 3.
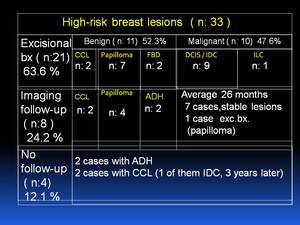
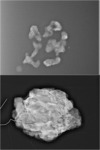
Fig. 3
We found underestimation rates 28.5 % for ADH,
4.7 % for CCL,
4.7 % for LN and 9.5 % for papilloma as shown on Figure 4.
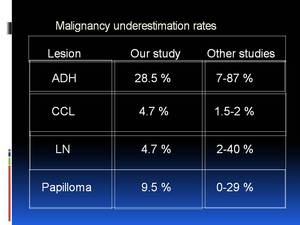
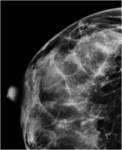
Fig. 4