1.
Importance of Ischemia-guided Revascularization
Quantitative assessment of coronary stenosis that revealing significant stenosis is important,
and it proved to improve the overall patients’ survival (1,
2).
Therefore,
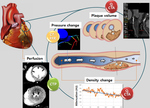
the detection of “hemodynamically” significant stenosis is the key point when we encounter the coronary CT angiography (CTA) for the patients with suspected coronary artery disease. We are expecting the functional assessment techniques,
quantitative CTA,
CT perfusion (CTP),
and CT-derived fractional flow reserve (CT-FFR),
will overcome the limitation of visual assessment (Fig 1).
2.
Quantitative CTA
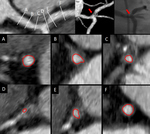
- Plaque Volume : Using the cross-sectional images of the coronary artery obtained at 1 mm interval (Fig 2),
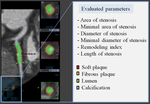
plaque analyses including area,
diameter and length of stenosis,
and plaque characterization (soft,
fibrous,
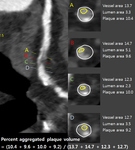
or calcified plaques) are assessed (Fig 3).The percent aggregated plaque volume (%) is obtained by the summation of plaque volumes at every 1 mm interval of the stenotic area,
divided by the total vessel volume (Fig 4).
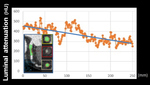
- Transluminal attenuation gradient (TAG) : Transluminal attenuation gradient (TAG) is the contrast opacification gradient through the coronary artery on CTA (Fig 5).
Linear regression analysis of the TAG of coronary artery has been proposed based on concept of the fall off of the contrast opacification in the distal coronary artery beyond the significant stenosis (3,4).
The integrated protocol using CTA,
CTP,
and and TAG showed superior diagnostic performance to each technique,
CTA plus TAG or CTA plus CTP (5).
3.
CT Perfusion
The rationale of CT perfusion (CTP) to evaluate myocardial ischemia is that decreased perfusion of myocardium in the area of stenotic vessels results in reduced the concentration of contrast in the myocardial tissue during the first pass circulation.
By calculating the time attenuation curve of myocardium,
quantitative assessment of myocardial flow could be performed.
Stress myocardial CTP can provide an incremental value over CTA alone,
especially in patients with a high calcium score. The accuracy of CTP to detect myocardial ischemia is higher than SPECT (6-8),
magnetic resonance perfusion imaging (9).
- Perfusion CT Protocol : In our hospital,
stress- and rest- CTP are performed using a second-generation dual source CT scanner (Definition Flash,
Siemens,
Forchheim,
Germany).
We performed a stress CTP first,
and then,
rest CTP is obtained ten minutes after the adenosine discontinuation.
During adenosine infusion (140 μg/kg/min for 5 minutes),
stress CTP is acquired using a retrospective electrocardiography (ECG) gated scan.
- CTP visual assessment : CT data is reconstructed on a workstation using a smooth kernel (B10f) at multiphase cardiac CT (0% - 90% of R-R interval,
10% increment).
A 10-mm-thick multi-planar reformatted image is generated with a narrow window (W) and level (L) setting (W200/L100) for improving the contrast-to-noise ratio.
The true perfusion defect may defined as a low density lesion appertains to the coronary territory,
persistently visualized throughout the whole multi-phase cardiac cycle on cine images (Fig 6).
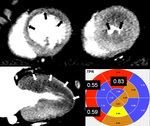
- Quantitative Analysis of CTP : For quantitative analysis,
we use customized software for assessing myocardial density of 16 segments and into three myocardial layers.
The myocardial CT density in both the stress (Densitystress) and rest (Densityrest) phases are measured.
The transmural perfusion ratio (TPR) is a good quantitative parameter although it showed lower diagnostic accuracy than visual assessment of CTP for hemodynamically significant stenosis.
TPR is calculated as the ratio of the subendocardial density to the subepicardial density in all segments of the short-axis images (10).
The myocardial perfusion reserve index (MPRI) on static CT perfusion imaging is obtained in each myocardial segment as follows: (Densitystress – Densityrest)/Densityrest × 100 %.
4.
CT-based FFR
Fractional flow reserve (FFR) is the ratio of mean pressure distal to the coronary stenosis versus the flow in the normal vessel,
hypothetically,
mean aortic pressure.
Using invasive FFR,
the differentiation of hemodynamically significant stenosis that needs to do a revascularization could be determined (Fig 7).
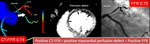
On CT,
after semi-antomated segmentation of coronary arteries,
generation of 3-dimentional (3-D) model of coronary trees can be used to calculate computational fluid dynamics.
With the 3-D flow simulation of coronary artery using the theoretical blood model as a Newtonian fluid,
the computation of coronary CTA data could provide CT-based FFR value.
Because CT-FFR can simulate the indirect ischemia condition showing adenosine-induced hyperemia,
neither additional scan nor adenosine infusion required.
The diagnostic threshold value of ischemia is less than 0.8.
However,
it would not be adjusted in poor image quality,
stent,
or CABG graft state.
The diagnostic performance of CT-FFR has been shown up to 86-93% of sensitivity and 54-82% of specificity (11-14).
5.
Limitations
The positive predictive value of coronary CTA is still low.
Calcified plaques or coronary stent can cause blooming artifact,
and that bring the low positive predictive value of coronary CTA,
although a recent study demonstrated an iterative reconstruction method to reduce the limitation (15).
The quantitative evaluation of coronary plaque imaging could be improved by slice to slice comparison with the results of dedicated automated quantitative software with intravascular ultrasound, and virtual histology.
Several practical limitations of CT-based myocardial ischemia evaluation are the pseudo-defect of CTP,
and low performance of CT-FFR in a patient with poor image quality,
stent or CABG state.
In practice,
these are rarely encountered; however,
their impact can be diminished by integrating the three methods,
quantitative CTA,
CTP and CT-FFR.
Other limitations of CT should also be kept in mind,
the increased radiation dose from the acquiring multi-phase images,
increased image acquisition time and contrast usage.
However,
radiation dose reduction can be achieved by using a low dose CT,
prospective ECG-gated CT or iterative reconstruction methods.
Concerning the image acquisition time,
the combination protocol for assessment of CTP and CT-FFR could be used to reduce the overall acquisition time up to 15 minutes.
With the one shot contrast usage,
quantitative evaluation of CTA and CT-FFR could be performed by using the rest perfusion CT.
Finally,
with the trade-off of spending more interpretation time by scrutinizing review of the multi-phase images and requires additional reconstruction,
the diagnostic performance of CT could be optimized.