This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Breast, Oncology, Ultrasound, Elastography, MR, Diagnostic procedure, Cancer, Neoplasia
Authors:
O. Catalano1, R. Fusco2, M. Di Bonito1, A. Nunziata3, V. Nunziata1, S. Filice1, A. Petrillo1; 1Naples/IT, 2Naples, It/IT, 3Ercolano/IT
DOI:
10.1594/ecr2016/C-0519
Aims and objectives
We know that US has the tendency to underestimate the size of breast malignancies (Fig. 1),
particularly in the case of:
- lobular tumors
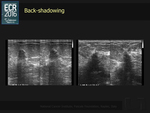
- “vertical” lesions (back shadow)
- retroareolar lesions
- spiculated lesions
- non mass-like lesions
- lesions with large in situ components.
Back-shadowing is present in 35% of breast cancers,
is not specific for malignancy,
and correlates with the desmoplastic reaction (Fig. 2).
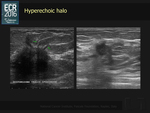
The hyperechoic peritumoral halo may be thick or thin and is due to the tumor infiltration (spiculations) and/or to the desmoplastic reaction and/or to the peritumoral edema (inflammation) and lymphedema (lymphatic ducts obstruction) (Fig. 3).
The key problem is to understand where does the tumor end and the fibrosis and/or in situ component start.
Previous studies tried to use 3D to improve US measurement of tumor size,
but ineffectively (Fig. 4).
We know that the elastographic behavior of breast lesions is influenced by several factors (breast density,
lesion depth,
lesion histotype,
etc.).
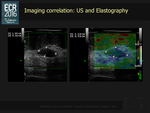
However elastography may theoretically allow to better display the local extent of breast cancer into the perifocal tissues and consequently improve the measurement accuracy.
The 2013 EFSUMB guidelines for elastography do not consider the extent assessment among the recommendations for this US technique (Fig. 5).
The purpose of our study was to evaluate the potential of elastography in the accurate assessment of breast cancer size preoperatively (Fig. 6).