This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Breast, Oncology, Ultrasound, Elastography, MR, Diagnostic procedure, Cancer, Neoplasia
Authors:
O. Catalano1, R. Fusco2, M. Di Bonito1, A. Nunziata3, V. Nunziata1, S. Filice1, A. Petrillo1; 1Naples/IT, 2Naples, It/IT, 3Ercolano/IT
DOI:
10.1594/ecr2016/C-0519
Results
We enrolled 22 pts.
not consecutive undergoing radical mastectomy,
quadrantectomy,
or wedge resection.
Two cases were excluded for incompleteness or inadequacy of the preoperative data and one case was excluded because the suspicion of malignancy was not confirmed at final pathology.
The final study group consisted of 23 malignant lesions (1-4/pt.,
mean 1.2) in 19 patients (26-88 years old,
mean 56).
The location was:
- 10 central
- 8 retro-parareolar
- 5 peripheral.
The morphological pattern was:
- 11 ill-defined,
nodular
- 9 well-defined,
nodular
- 3 diffuse.
The histotype was:
- 15 infiltrating ductal carcinomas
- 7 infiltrating lobular carcinomas
- 1 in situ ductal carcinoma.
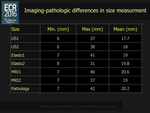
The measurements are shown in Fig. 12 and Fig. 13.
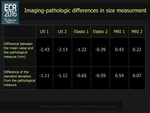
MRI gave the lowest measurement error,
compared with the pathological reference,
in terms of mean and standard deviation (Fig. 14).
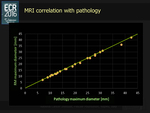
This is also shown by the dispersion graphic of the three modalities (Fig. 15),
( Fig. 16).
The correlation of the three imaging modalities (mean between the measures from the two operators) with the pathological standard gave a Pearson Coefficient of 0.893 for US,
0.886 for elastography,
and 0.998 for MRI.
The Mann Witney test gave a p value >0.05 (0.3674 between US and MRI,
0.5309 between US and elastography,
and 0.8432 between elastography and MRI).
To evaluate the difference between the median mismatch value for the three imaging modalities we employed the Kruskall Wallis test (Fig. 17).
The p value was <0.0001 The Intraclass Correlation Coefficient (ICC) between the three modalities was 0.89 (0.987 for US,
0.991 for elastography,
and 0.996 for MRI.
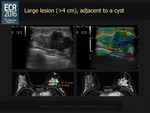
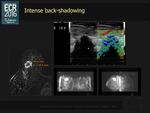
In performing this study we had the following difficulties:
Measuring breast cancer is relevant for several aspects:
- size is a key aspect in establishing the T staging parameter (Fig. 23)
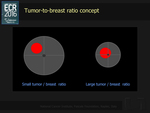
- tumor size and tumor-to-breast size influences the surgical choice (Fig. 24)
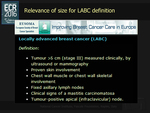
- size is a key aspect in defining a breast cancer as locally advanced and consequently in decided for a neoadjuvant treatment before surgery (Fig. 25)
- current oncological criteria in establishing the response to treatment of the lesions are based on their number and size
- size correlates with patient prognosis.