Fig.
1
IMAGING PROTOCOLS
All patients were examined on a 1.5T whole body MR system using a 5 -element surface array coil.
Image acquisition was perfomed ECG triggered and in breath hold.
The examination protocol included morphologic,
fucntional,
perfusion and tissue characterization imaging along cardiac axes.
- Morphology and function was assessed using cine steady state free precession (SSFP) sequences.
- Fast spin-echo T2-weighted sequences or short tau inversion recovery (STIR) sequences were used to detect edema and inflammation.
- Iron in the myocardium was quantified by measurin T2* using multi-echo GRE sequences obtained in a single breath hold.
- Phase contrast imaging allows quantitative assessment of low across the atrioventricular valves.
- If arrhythmogenic right ventricular dysplasia was suspected,
a fast spin-echo T1 sequence was also obtained.
- Myocardial perfusion was assessed at rest using 2D saturation recovery gradient echo (GRE) sequences after injection of 0.1 mmol/kg of gadolinium.
- Myocardial late gadolinium enhancement was assessed using 2D inversion recovery GRE sequences in four chamber view,
two chamber view and shor axis views 10 minutes after injection of 0,2 mmol/kg of gadolinium.
PRIMARY CARDIOMYOPATHIES
The Wolrd Health Organization recognizes four forms of cardiomyophaties: dilated,
hypertrophic,
restrictive and arrhythmogenic right ventricular cardiomyopathy.
Left ventricular non-compaction cardiomyopathy increasingly is being recognized as a fifth form.
Dilated cardiomyopathy
Dilated cardiomyopathy (DCM) is the most common form of cardiomyopathy in children,
characterized by dilatation and systolic dysfunction of the left ventricle (LV) or both ventricles,
in the absence of congenital,
valvular or coronary artery disease or any systemic disease known to cause myocardial dysfunction.
Epidemiology
- Annual incidence: 0,58/10.000 children.
- More common in boys (age < 1 year-old) than children.
Etiology
- Most of them are idiopathic,
followed by familial forms (6,8%) due to inborn erros of metabolism mainly regarding metabolic disorders,
oxidative phosphorylation defects and systemic carnitine deficiency.
- Myocarditis is commonly associated with DCM in children.
- Genetic causes account for more than 30-35% of cases.
- DCM is the most genetically heterogeneous of all cardiomyopathies with all Mendelian patterns of inheritance represented.
Clinical
Infants and children usually present with signs of congestive heart failure.
Symptoms in infants:
- Tachypnea,
labored breathing,
poor apetite,
and slow weight gain.
Symptoms in children:
- There may be signs of poor exercice tolerance and gastrointestinal distress.
- In more severe cases,
patients may experience syncope,
arrhythmias or sudden cardiac death.
Diagnosis
Diagnostic criteria:
- Exclusion of potencial secondary causes of ventricular dilatation and dysfunction.
- LV ejection fraction <45%
- LV end-diastolic dimensions >117% of the predicted value by the Henry formula
Familial DCM:
- Two or more affected individuals in a single family or in the presence of a first-degree relative of a DCM patient,
with well-documented unesplained sudden death at < 35 years of age.
MRI findings
Cardiac MRI has gained an important role in the diagnosis of patients presenting with systolic heart failure.
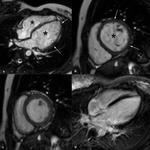
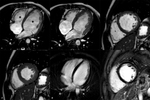
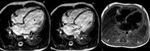
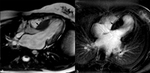
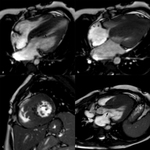
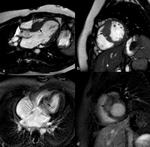
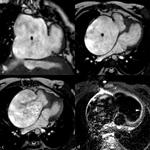
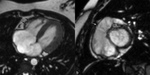
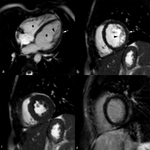
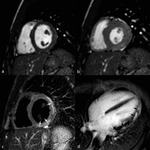
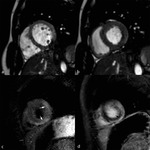
- Dilatation and systolic dysfunction of LV or both ventricles (Fig. 1 Fig. 2 Fig. 3)
- Myocardial wall thinning (diastolic wall thickness < 5.5 mm) in advanced cases (Fig. 1)
- Late gadolinium enhancement (LGE) is uncommon (16% of cases): mid-wall,
focal patchy,
RV insertion site and transmural patterns.
Risk markers of sudden death
- Left ventricular ejection fraction less than 35%.
- There are limited data to suggest that the presence of myocardial fibrosis and associated LGE is a predictor of risk of future arrhythmia and sudden cardiac death.
- Unlike adult patients,
the absence orf LGE is not an independent predictor of LV reverse remodeling during follow up.
Hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy (HCM) is defined by the presence of unexplained myocardial hypertrophy in the absence of cardiac or systemic cause.
it is the second most common form of hearth muscle disease and comprises abouy 35-40% of cardiomyopathies in children.
Epidemiology
- Annual incidence: 0,47/10.000 children.
Etiology
- Genetic origin,
including association with inborn errors of metabolism,
neuromuscular disorders and malformation syndromes.
- Non-genetic causes are rare in children,
although transient LV hypertrohphy can occur in response to some enviromental trigers,
such as in infants of diabetic mothers.
- Most cases of HCM in children are caused by dominant mutations in cardiac sarcomere protein genes.
Clinical
- Children <1 year of age often have symptoms of congestive heart failure.
- Older children may be remain asymptomatic and have normal life expectancy.
Symptoms in children:
- Dyspnea,
chest pain,
pre syncope,
syncope,
exercise intolerance or palpitations.
Symptoms in infants:
- May be more difficult to detect.
- Difficult breathing,
poor growth,
escessive sweating or crying and agitation during feeding.
Rarely,
HCM may present with cardiac arrest and sudden cardiac death (SCD).
It is the most common cause of premature SCD due to malignant ventricular arrhythmias.
Diagnosis
- To meet diagnostic criteria in children,
LV wall thickness by any imaging technique must be greater that 2 standard deviations above normal population mean for age and body surface area.
(Fig. 4 Fig. 5 Fig. 6)
- Identification of familial gene allows close following of those children who carry the gene for an early diagnose if they develop the disease.
MRI findings
Cardiac MR imaging has evolved into a multiparametric imaging modality allowing a truly comprehensive of disease,
providing information of cardiac phenotype,
its functional and hemodynamic characterization,
presence and extent of microvascular dysfunction and myocardial fibrosis.
There is a great variability of HCM phenotypes with onset at virtually any age,
including in utero:
- The "classic" HCM phenotype of a non-dilated LV with diffuse septal hypertrophy is the most common in children (Fig. 5)
- More rarely,
hypertrophy is localized in the anterior wall,
the apex or in the mid left ventricle (Fig. 4 Fig. 6)
Other morphologic and functional manifestation include:
- Abnormalities in appearance,
number and implantation of papillary muscles.
- Anterior mitral valve leaflet elongation (Fig. 5)
- Deep myocardial crypts in HCM patients and in genotype-positive family members (Fig. 7)
- Left atrial remodeling.
- Areas of LV noncompaction at inferior and lateral apical segments may represent a marker of genetic transmission in family members without hypertrophy.
- Apical aneurysms.
- LV outflow obstruction.
- Diastolic dysfunction.
- Areas of diminished myocardial perfusion by microvascular ischemia
- Isolated or multiple patchy myocardial LGE by myocardial fibrosis.
(Fig. 6)
-
- Recent studies suggest lower LGE prevalence in children than adults.
- LGE is most common in the interventricular septum.
(Fig. 6)
Risk markers for sudden death
Risk death or heart transplantation factors in pediatric population include:
- Diagnosis of HCM at less than 1 year of age,
children inborn errors of metabolism,
lower weight,
congestive heart failure and higher LV end-diastolic lateral or septal wall thickness at the time of cardiomyopathy diagnosis.
- The presence and extent of myocardial LGE and LV apical aneurysms in mid ventricular or apical HCM are associated with adverse events.
Larger researches and longer follow-up are required to evaluate the progression of HCM in childhood.
Restrictive cardiomyopathy
Restrictive cardiomyopathy (RCM) is among the rarest heart muscle disease in children characterized by enlargement of both atria and both ventricle, restrictive physiology and normal systolic function and size.
Epidemiology
- Annual incidence: 0,03-0,04 cases / 10.000 children.
- Less than 5% of all pediatric cardiomyopathies.
- Idiopathic RCM has been described in all ages children and may be slightly more common in girls.
Etiology
- Non infiltrative
-
- Idiopathic (most common),
familial (30%),
post cardiac transplant
- Infiltrative
-
- Amyloidosis (rare in children),
sarcoidosis,
hemochromatosis,
Gaucher,
Hurler and Fabry disease
- Endomyocardial
-
- Endomyocardial fibrosis (most common cause in certain tropical areas,
Loeffler endocarditis,
pseudoxanthoma elasticum and drugs).
(Fig. 8)
- Mixed restrictive-hypertrophic phenotypes occur (30%).
- Most cases of RCM (including idiopathic ones) are not known to be inherited.
Clinical
- In children the first symptoms are often related to problems other than the heart:
-
- History of repeated lung infection or asthma are frequent
- Ascites,
hepatomegaly and edema
- Related to heart:
-
- Signs of heart failure,
syncope (10%) or sudden death (28%)
- Prognosis for the pediatric patient is poor,
with 2-year survival rates of 50%
Diagnosis
Early diagnosis is difficult due to the lack of heart symptoms
- Marked enlargement of both atria,
normal size of both ventricles and normal heart function.
(Fig. 8)
- In more advanced disease states,
increment of pulmonary artery pressure.
- Echocardiography and MRI are very useful in distinguishing RCM from constrictive pericarditis.
MRI findings
- Marked atrial enlargement with normal size of both ventricles and normal heart function.
(Fig. 8)
- MR is a useful technique for the diagnosis of endomyocardial fibrosis
-
- High T2 or STIR signal intensity in the endocardial and subendocardial right and left of apical walls and inflow portions.
- Cavitary thrombus as a hypointense band on cine.MRI images
- Endomyocardial LGE by fibrosis.
(Fig. 8)
- MR plays an important role in the detection and quantification of cardiac iron deposition:
-
- Iron myocardial deposition causes a decrease in T2* relaxation time,
which can be detected by multi-echo gradient sequences.
- The measurements are performed in short axis at the mid-ventricular level in the interventricular septum.
- T2* > 20 ms: no iron deposition is detected; T2* ≤ 20 ms: iron deposition is detected; T2* < 10 mseg: high risk of heart failure.
Risk markers for sudden death
- Signs or symptoms of ischemia:
-
- Chest pain,
syncope,
or both
Arrhythmogenic right ventricular cardiomyopathy
Arrhythmogenic right ventricular cardiomyopathy (ARVC) is characterized by progressive fatty or fibro-fatty replacement of the right ventricular (RV) myocardium,
but this has been shown to also extend into the LV in some cases.
Epidemiology
- Although ARVC is rare,
it is thought to be responsible for 20% or more of sudden cardiac deaths among young individuals.
Etiology
- Inherited cardiomyopathy predominantly associated with mutations in desmosomal genes with incomplete penetrance and variable expressivity.
Clinical
- Ventricular electrical instability,
often occurring before structural abnormalities.
- It is exceedingly rare to manifest clinical signs or symptoms of ARVC prior to 12 years of age.
Diagnosis
- Based on a combination of so-called major and minor criteria proposed by the International Task Force in 1994 and modified in 2010 that include
-
- Structural,
functional,
electrocardiographic,
arrhythmic,
genetic,
and histological abnormalities.
- In pediatric patients,
diagnosis remains challenging
-
- Children who are gene positive for ARVC may not exhibit all phenotypic features until adulthood.
- Today,
genetic testing and cardiac MRI play and important role in the diagnosis.
MRI findings
The revised Task Force criteria for the diagnosis of ARVC by MRI include:
- Morphologic features:
-
- Right ventricular dilatation.
Common but nonspecific.
(Fig. 9)
- Myocardial thinning.
Focal wall thickness < 2 mm.
- Systolic small multiple outpouchings with an appearance of focal crinkling (“accordion sign").
It is an early sign of ARVC in asymptomatic patients.
(Fig. 9)
- Signal intensity anomalies:
-
- Fat and fibrosis detection by noninvasive imaging is not part of the Task Force Criteria and,
in clinical practice,
the unequivocal detection of RV fatty infiltration of by MRI is often challenging.
- Fatty infiltration with RV thickness ≥ 6 mm,
but without regional or global functional abnormalities,
is considered distinct from fatty RV in ARVC.
Fatty infiltration is seldom the only abnormality.
- LGE by myocardial fibrosis.
-
- Enhancement of the RV is challenging because of the thin thickness of the RV free wall and the presence of a layer of epicardial fat that also shows high-intensity signals.
- Left ventricular LGE usually at inferolateral wall and inferior wall-septal junction.
- Functional features:
-
- Regional RV dysfunction: akinetic or dyskinetic wall motion (most sensitive and specific finding).
- Regional LV dysfunction.
- Progressive RV systolic disfunction and dilatation.
Risk markers for sudden death
- Unexplained syncope,
RV dilatation,
LV involvement and asymptomatic mutation carriers.
Non-compacted cardiomyopathy
Non-compacted cardiomyopathy (NCC) is a genetically and clinically heterogeneous cardiomyopathy characterized by numerous prominent trabeculations,
progressive myocardial dysfunction and malignant ventricular arrhythmias
Epidemiology
- NCC accounts for approximately 9% of newly diagnosed cardiomyopathies
- It can presents isolated or in combination with DCM,
HCM or with congenital heart defects
-
- Ebstein's anomaly or complex cyanotic heart disease.
Etiology
- It may be sporadic or a familial disease,
with autosomal recessive,
X-linked recessive,
or autosomal dominant inheritance.
- Incidence of death and transplantation: 18%
-
- Higher mortality in first year life (30%)
Clinical
- Asymptomatic during life.
- Asymptomatic or symptoms of heart failure symptoms,
arrhythmias,
thromboembolism and sudden cardiac death.
- Symptoms in adolescence and adulthood.
Diagnosis
- Ratio of non-compacted to compact myocardium:
-
- Echocardiography: > 2.0 at the end of systole.
- MRI: > 2.3 at the end of diastole on short-axis plane.
(Fig. 10 Fig. 11)
- Usually involves the LV: apical,
mid-inferior,
and mid-lateral myocardial segments.
- Involvement of both ventricles or isolated RV aslo can be seen.
MRI findings
- Imaging hallmark of non-compacted cardiomyopathy
-
- Increased myocardial thickness with a two-layer structure,
a thin compacted subepicardial layer and a thicker,
non-compacted subendocardial layer.
(Fig. 10 Fig. 11)
- The ratio of non-compacted to compacted myocardium on short-axis plane at the end of diastole is > 2,3.
- Chamber dilatation and systolic dysfunction are common findings.
- LGE involving non-compacted and normal segments
-
- Prevalence of LGE (25 %) is lower in children than adults
Risk markers for sudden death
Risk death or heart transplantation factors in pediatric population include:
- Cardiac dysfunction,
chamber dilatation and ventricular arrhythmias.
- LGE is associated with ventricular arrhythmias and ventricular dysfunction.
SECONDARY CARDIOMYOPATHIES
Myocarditis
Pediatric myocarditis is a rare inflammatory myocardial disorder typically caused by a viral infection.
It is an important cause of morbidity and mortality in children and it may lead to acute heart failure,
dilated cardiomyopathy,
and sudden cardiac death.
Epidemiology
- Newborns,
infants and immunocompromised patients have increased susceptibility to myocarditis.
Etiology
- Adenovirus and enterovirus infections (coxsackievirus),
although many infectious organisms commonly seen in infants and children have been implicated in the disease.
Clinical
- Few or no symptoms in mild forms.
- In severe cases,
heart failure and progress to death usually weeks after the initial viral infection and prodromal symptoms.
- Neonates may seem irritable,
be in respiratory distress,
and exhibit signs of sepsis.
- Signs in infants include failure to thrive,
anorexia,
tachypnea,
tachycardia,
wheezing,
and diaphoresis with syncope.
- Complete recovery of ventricular function has been reported in 50% of patients.
- Some patients develop chronic myocarditis:
-
- An association has been suggested between myocarditis and dilated cardiomyopathy.
- Those who develop dilated cardiomyopathy may require a heart transplant.
Diagnosis
- Accurate diagnosis of myocarditis is challenging because the severity and type of symptoms is quite variable.
- No single test can confirm or exclude the diagnosis with certainty.
-
- Endomyocardial biopsy,
the most widely accepted standard,
still suffers from sampling errors which reduce sensitivity,
suboptimal inter-observer agreement,
and the risk of complications
- In clinical practice,
history,
test results,
and clinical course are all integrated to make the diagnosis.
MRI findings
Studies about the utility of MRI in pediatric acute myocarditis are few.
- Left systolic disfunction (most common),
increased LV end diastolic and systolic dimensions,
segmental wall motion abnormalities and pericardial effusion.
- Focal or global myocardial signal increase on T2-weighted images at early disease.
(Fig. 12 Fig. 13)
- Normal signal intensity on T2-weighted sequences in the healing phase.
- Late gadolinium-enhanced sequence is key to detect lesions of acute myocarditis
-
- Subepicardial enhancement foci and sparing of the subendocardial layers.
(Fig. 12 Fig. 13)
Risk markers for sudden death
Wide spectrum of mortality and morbidity statistics
- Coxsackievirus B infection
-
- Mortality rate is higher in newborns (75%) than in older infants and children (10-25%)
- Left ventricular ejection fraction<30% and LGE on MRI are predictors of poor outcome. (Fig. 12 Fig. 13)