2.1 A BRIEF HISTORY
In 1877,
Sir James Paget (Fig 1),
a prominent British surgeon and pathologist described ‘osteitis deformans’ in five middle-aged men. Although several reports of middle-aged men whose hats no longer fit had already been published in the literature,
by the end of the century,
the affliction would become widely known as Paget’s disease of bone.

Fig. 1: Sir James Paget (1814 – 1899) by John Everett Millais.
References: http://www.nationalgallery.org.uk/paintings/quinten-massys-an-old-woman-the-ugly-duchess
Paget described the disease as a rare,
slowly progressive inflammatory disorder which did not affect the individual’s overall general health,
but resulted in change in body shape,
size and deformity of affected bones.
2.2 PAGET’S IN CLINICAL PRACTICE
Paget’s disease demonstrates certain geographical and racial characteristics: it is more common in Great Britain,
France,
Germany,
Italy and migrants from these countries while it is particularly rare in Ireland,
sub-Saharan Africa,
the far East and Scandinavia.
Overall incidence of the disease is on a steep decline. Prevalence increases with age – those over 85 years of age are 5 times more likely to be affected than those under the age of 60.
A slight male predominance is also seen with a 3:2 male-to-female ratio reported in the literatute.
This non-inflammatory,
metabolic disorder may affect single or multiple bones in a synchronous or metachronous fashion; polyostotic disease is more often seen.
Patients are frequently asymptomatic and cases are usually discovered incidentally on imaging carried out for other reasons.
The most common manifestation of this disease,
if any,
is pain of the involved bone and adjacent joints. Bone turnover markers,
including bone specific alkaline phosphatase,
reflect the level of osteoblast activation,
and may be used to monitor the level of activity and therapeutic efficacy.
Paget’s disease shows a predilection for the axial skeleton with the skull and vertebral column being the most commonly affected sites.
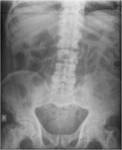
The pelvis is the most commonly affected part of the appendicular skeleton (Fig 2).

Fig. 2: AP radiograph of the lumbar spine showing polyostotic Paget’s disease involving both femora, ilii, T12-L2 and L5 vertebrae
2.3 PATHOLOGY OF PAGET’S DISEASE
In the initial osteolytic phase,
focal excessive osteoclastic action causes bone resorption. In the later (though still relatively early) mixed osteolytic/osteoblastic phase,
excessive osteoclastic activity continues but is accompanied by simultaneous disorganised activation of osteoblasts and fibroblasts resulting in new bone formation.
In time,
osteoblastic activity predominates,
with random deposition of dense but disorganized and structurally weak new bone.
This translates into increasing bone density and thickening of the remaining trabeculae,
giving a classic histological “mosaic pattern” of woven and lamellar bone,
which replaces the organised parallel Haversian systems that characterize normal bone.
Replacement of bone marrow with vascular and fibrous tissue is also seen in this stage.
In the late osteosclerotic “burnt-out” phase,
osteoclastic activity declines and bone turnover may return to an almost normal level.
The thickened trabeculated bone and prominent mosaic pattern persist,
and there is restoration of the marrow.
Histopathological appearances of Paget’s disease closely mirror radiological features; imaging studies can be used to stage Paget’s disease as well as monitor disease activity.