This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Interventional non-vascular, Genital / Reproductive system male, Ultrasound, MR, Biopsy
Authors:
G. Bizzarri1, A. Bianchini1, D. Valle1, L. Di Vito1, L. Velari1, L. Lodigiani1, A. Dell'Era1, V. Anelli2; 1Albano Laziale/IT, 2Rome/IT
DOI:
10.1594/ecr2017/B-0390
Methods and materials
For the present study a MyLabTwice ultrasound scanner (ESAOTE,
Italy) equipped with an EM tracking system and Virtual Navigation (VN) software was used (Fig 2).
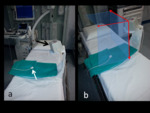
The procedure was performed on 20 patients (average age 75) with an end-fire (3-9 MHz) transrectal probe with single use guiding system and a reusable tracking bracket for magnetic sensor (CIVCO,
USA) (Fig 3).
All the patients enrolled had a preliminary mpMRI or at least bi-parametric MRI performed within one month of the biopsy.
MRI images were loaded onto a US scanner and evaluated with navigation software for the presence of abnormal signal intensities (Fig 4),
and if suspicious lesions were identified they were targeted (Fig 5).
Images were also evaluated as regards the presence of cystic lesions.
Patients received a double antibiotic prophylaxis (Ciprofloxacina 500 mg x2 starting 1 day before and continuing for a total of 5 days and Ceftriaxone 1g e.v.
just before the procedure).
Common coagulation parameters were evaluated within one week of the procedure.
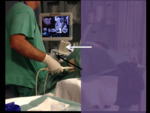
With the patient in the left-side decubitus,
the support for the magnetic generator was fastened under the knees so that the generator was no more than 20-30 cm away from the perineal region (Fig 6).
TRUS guided periprostatic nerve block anesthesia (mepivacaina 2% 10ml.) was performed.
Spatial co-registration was obtained overlapping the midline sagittal scans,
including the urethra.
The navigation modality was activated (Fig 7) and the co-registration accuracy was evaluated using,
if present,
cystic lesions visible on both US and T2W MRI images (Fig 8).
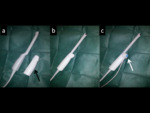
The targeted biopsy was performed with at least 2 samples for each target using a fully automatic 180 mm.
18G Trucut-needle (Fig 9).
A systematic biopsy was then carried out with the same needle.
The time required for co-registration was recorded.