Purpose
Breast cancer is a heterogeneus disease.
Nowadays immunohistochemical patterns are very important to classify the tumors acording to their aggressivity and prognostic factors.
In particular,
Luminal A tumors can have a very good prognosis,
while triple-negative and pure Her-2 cancers can be very aggressive.
Both mammography and tomosynthesis are very sensitive to spiculations,
but not as sensitive to detect masses in dense breasts.
However,
US can detect masses in dense breasts,
but fails to asses spiculations and distortions.
Our purpose was to assess the influence...
Methods and materials
This retrospective,
single-centre,
lesion-based study was approved by the IRB.
277 cancers,
histologically confirmed,
were reviewed from October 2011 to September 2016.
Out of them,
30 pure intraductal cancers were excluded.
Our final sample consisted on 247 invasive cancers.
All of them were previously studied with mammography,
tomosynthesis ans US.
Imaging evaluation
Both DM and DBT studies were performed using a Siemens Mammomat Inspiration unit (Siemens Medical Solutions,
Erlangen,
Germany).
Standard 45 mediolateral oblique (MLO) and craniocaudal (CC) DM views were acquired.
Given that our...
Results
Among the 247 cancers reviewed,
there were 208 invasive ductal carcinomas (IDC),
36 invasive lobular cancers (ILC) and 3 malignant phyllodes tumors.
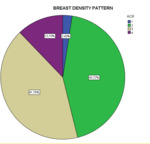
The distribution of the density pattern of the breasts was as follows:
ACR a: 6 (2.4%)
ACR b: 108 (43.7%)
ACR c: 103 (41.7%)
ACR d: 30 (12.1%)
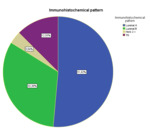
The distribution of the immunohistochemical patterns of the lesions was as follows:
Luminal A: 127 (51.4%)
Luminal B: 80 (32.4%)
Pure Her-2: 9 (3.6)
Triple negative: 31 (12.6 %)
The mean size of the tumors...
Conclusion
Additional US significantly increased the sensitivity of mammography in all immunohistochemical patterns.
For Luminal A cancers:
Whatever the combination of mammography plus an additional technique,
the sensitivity is significantly higher than for mammography alone(MXUS (84%) and MXDBT (78%) vs MX (46%); p<0.001 for both comparisons).
At comparingMXUS vs MXDBT no significant differences were found (p=0.185).
This means both combinations worked similarly.
For Luminal Bcancers:
Whatever the combination of mammography plus an additional technique,
the sensitivity is significantly higher than for mammography alone(MXUS (90%) and MXDBT...
References
-Molecular subtypes and imaging nphenotypes of breast cancer Nariya Cho; Ultrasonography 35(4),
October 2016
-Triple-Negative Breast Cancer: Correlation between MR Imaging and Pathologic Findings
Takayoshi Uematsu et al; Radiology: Volume 250: Number 3—March 2009
-Estrogen Receptor–Negative Invasive Breast Cancer: Imaging Features of Tumors with and without Human Epidermal Growth Factor Receptor Type 2 Overexpression
Yingbing Wang et al; Radiology: Volume 246: Number 2—February 2008
-Multimodality Imaging of Triple Receptor–Negative Tumors With Mammography,
Ultrasound,
and MRI Basak E.
Dogan et al; AJR 2010; 194:1160–1166
-The correlation...