Plain radiograph may help to diagnose teratoma showing tooth components or nonspecific calcifications.
It is seen as a cystic adnexal mass with some mural components (mural hyperechoic Rokitansky nodule) with ultrasound (preferred for no ionising radiation).
CT images demonstrate calcifications,
fat or fat-fluid level or Rokitansky protuberances.
Finally,
MRI is really sensible identifying fat components.
Malignant transformation should be suspected when the size exceeds 10cms or soft tissue parts of the neoplasm have an irregular shape or invade contiguous structures.
We will proceed to explain the characteristic findings in several imaging modalities:
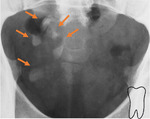
- PLAIN RADIOGRAPH FINDINGS:
Calcium shows the greatest radio-opacity on plain radiographs.
We may suspect the presence of mature cystic ovarian teratoma on plain radiograph,
if we identify a calcified density in female pelvis region.
In 31% of the cases of mature cystic ovarian teratoma,
we may be able to see teeth components (figure 2).
Rudimentary bone or curvilinear capsular that have been calcified may be seen in mature cystic teratoma.
Mature cystic ovarian teratoma may contain sebum that mimic low density fat and being recognizable on plain radiographs.
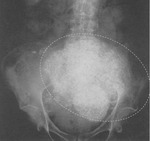
Uterine fibroid is another female pelvis lesion which may calcify.
We can differentiate it from mature cystic teratoma because of its calcifications have a spotted or dotted shape (figure 3).
- ULTRASOUND FINDINGS:
Ultrasound (US) is the imaging modality for initial diagnose.
Nevertheless,
US has several limitations for the diagnosis of this type of tumors with a sensibility and a specificity from 58% to 99%.
This wide range depends on the experience of sonographer so it is an “operator dependence” technique.
Typically mature cystic teratoma is seen as a cystic adnexal mass with some echogenic components within.
There are not interior vascularity (color Doppler).
If there are color Doppler within lesion,
we should exclude malignant disruption.
There are three US typical patterns:
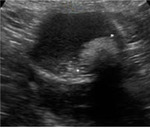
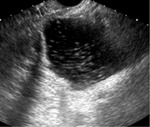
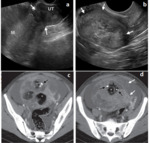
- Cystic lesion with a mural hyperechogenic nodule called Rokitansky: Rokitansy nodule (or dermoid plug) contains hair and/or sebaceous components.
Plump of hair absorbs and reflects sound at US,
the net effect is a focal hyperechogenic area that gradually attenuates sound and results in a characteristic gradual acoustic shadow (figure 4).
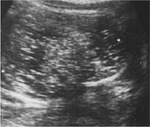
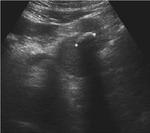
- Diffusely or partially echogenic mass with posterior sound attenuation due to sebaceous material and hair within the cyst lesion,
only superficial part of the cyst is seen -called the tip of the iceberg sign (figure 5).
- Multiple thin echogenic fine lines and dots caused by the hair into the surrounding fluid (anechogenic) generate an US image called "dermoid mesh” sign or dot-dash pattern (figure 6).
Other US features include intense acoustic shadowing within cyst owing to calcifications (tooth components) (figure 7) or the presence of fluid-fluid levels due to sebum floating in aqueous liquid.
Some studies reflect that in 74% of the mature cystic teratomas,
at least two of the above characteristic features are detected,
allowing experienced sonographers to make the correct diagnosis with a high positive predictive value.
- CT FINDINGS:
CT has a high sensitivity in the diagnosis of cystic teratomas though it is not routinely recommended for this purpose owing to its ionizing radiation.
The presence of fat attenuation within a cyst,
calcified wall,
Rokitansky nodules or tufts of hair on CT images is highly suggestive of mature cystic teratoma.
The presence of most of the above components is diagnostic of ovarian cystic teratomas in 98% of cases.
According to some studies,
most tumors measure 4-17 cm (average size: 8cm),
septa may be thin and the wall of the cyst,regular and not thick (2-5 mm).
The main CT findings of mature cystic teratoma include:
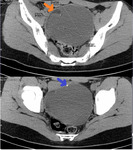
- Presence of fat attenuation components (figure 8): it has been reported that in more than 90% of cases,
fat attenuation has been seen on CT images; so its presence within an ovarian tumor is highly specific to mature cystic teratoma.
Fat attenuation may be identified as a round mass floating in the interface between two liquid components,
in the Rokitansky nodule or like a fat-fluid level (figure 9).
Fat attenuation components may also be seen in other ovarian tumors such as teratoma or lipoid tumor.
- Rokitansky nodule (figure 9): it is quite common to be found (in some series in 98% of cases).
It is seen as a protuberance projecting into the lumen of the cyst with a regular border and an oval shape.
Its average diameter is 28 mm (from 10 to 45 mm).
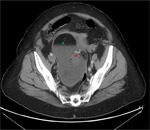
- Calcifications (Figure 8) or tooth components (figure) most often are found within mural nodules,
but they also may be seen in cystic septa or walls.
Although the presence of fat is a reliable sign of mature cystic teratoma,
the presence of calcium is less specific and can also be seen in ovarian cancer.
- Tufts of hair also may be identified on CT images.
- MR FINDINGS:
MR evaluation usually tends to be reserved for difficult cases but it is exquisitely sensitive to fat components.
Moreover,
it is especially indicated to differentiate fat from blood.
MR has some limitations in detecting calcium components.
Enhancement is also able to identify solid invasive components in malignant disruptions processes.
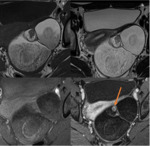
At MR imaging,
the sebaceous component has very high signal intensity on T1-weighted images,
similar to retroperitoneal fat.
The signal intensity of the sebaceous components on T2-weighted images is variable,
usually similar to fat.
Some hemorrhagic lesions,
most prominently endometriomas,
have the same combination of different signal intensities on T1- and T2- weighted images owing to blood.
Sequences with frequency-selective fat saturation will suppress the high signal of fat (sebaceous component) in teratomas helping to distinguish them from hemorrhagic lesions (figure 10).
It is not recommended the use of STIR (short-inversion-time inversion recovery) sequences due to that both,
hemorrhagic components of endometriomas and sebaceous components of mature cystic teratomas,
may present suppression signal.
Approximately 8-15% of these tumors contain very few or microscopic fat within the cystic cavity or in the wall.
In these cases,
gradient-echo imaging with an echo time in which fat and water are in opposite phase can differentiate microscopic fat.
COMPLICATIONS:
Mature teratomas,
although benign,
are resected because of potential complications,
including ovarian torsion (most common,
16% of teratomas),
malignant transformation (1-4%) or rupture (1-4%).
Other less common complications are infection (1%) or autoimmune hemolytic anemia (<1%).
CT and MR may help in diagnosing these complications.
- OVARIAN TORSION:
The main cyst/mass associated to ovarian torsion is mature cystic teratoma neoplasm.
Moreover,
ovarian torsion is the main complication of ovarian teratoma (16% of ovarian teratomas).
The tumor predisposes the ovary to become twisted around its pedicle,
leading to various degrees of hemorrhagic infarction.
Because of its double irrigation system (from both the uterine and ovarian arteries),
arterial flow is usually maintained until advanced stages,
while venous drainage may be compromised resulting in congestion with subsequent ovary hemorrhagic infarction.
The main factor that predispose to torsion is the size of ovarian tumor (larger than 6cm).
Pelvic ultrasound is the first-line imaging method for the evaluation of suspected ovarian torsion (onset pelvic pain in a female).
CT and MRI are useful if US is not definitive.
When cystic teratomas produce ovarian torsion,
the resultant congestion and edema are manifested in thickening of the cyst wall or engorged blood vessels on the twisted side.
Other findings are deviation of the uterus to the twisted side,
atypical position of twisted ovarian (in the midline and cranial to uterus) and free pelvic fluid.
It is said that if one ovary appears abnormally larger relative to the other side,
torsion may be present.
Nevertheless,
in cases of ovarian neoplasm,
the sign is less specific,
as this enlargement could be the result of the torsion rather than the cause of it.
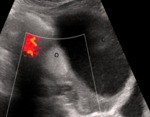
Color Doppler evaluation of the ovary often reveals an absence of blood flow,
a finding classically associated with ovarian torsion (figure 11).
However,
in 54% of patients,
torsion may be present even if arterial waveforms are demonstrated because of the arterial dual supply of the ovary.
The presence of arterial waveforms within the ovary should not sway the diagnosis away from ovarian torsion if other imaging findings and physical examination are consistent with torsion.
Twisted ovarian pedicle is pathognomonic for ovarian torsion,
but not always is demonstrated.
The homogeneous thickening of the wall of the ovarian teratoma,
frequently with lack of enhancement,
may suggest ovarian torsion.
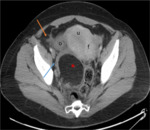
As well as lack of enhancement of the twisted adnexal may be seen on contrast CT images Surrounding fat stranding and free fluid are nonspecific findings (figure 12).
Finally,
>50 HU attenuation of the affected adnexal on non-contrast CT suggests hemorrhagic necrosis.
If torsion is suspected,
it may not be the imaging modality of choice,
as urgent imaging is required (US,
CT).
MR technique is useful if hemorrhagic infarction is suspected.
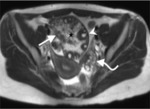
In such cases,
we can see a high-signal-intensity rim on T1-weighted MR images without contrast enhancement due to methaemoglobin presence (figure 13).
A twisted,
necrotic ovary fails to enhance after gadolinium administration.
2.
MALIGNANT TRANSFORMATION:
In 1-4% of cases ovarian cystic teratoma can be the site of malignant transformation.
Malignant transformation typically occurs in the 6th or 7th decade of life.
Squamous cell carcinoma is the most common type of malignant degeneration (more than 80% of cases) and characteristically increases serum squamous carcinoma antigen level in blood.
Malignant transformation typically arises from Rokitansky nodule and may be easily diagnosed if a heterogeneously irregular solid component is present with transmural extension and invasion of adjacent organs.
We may suspect malignant degeneration if the size of the tumor exceeds 10 cm.
The mere presence of enhancement of solid components does not always indicate malignancy but probably reflects the heterogeneity of tissues which may contain enhancing elements.
3.
RUPTURE:
Mature cystic teratoma can rupture,
causing leakage of the liquefied sebaceous contents into the peritoneum and resulting in a chemical peritonitis and the mesentery may be stranded and the peritoneum thickened,
which may mimic peritoneal carcinomatosis.
However,
this is a rare complication,
occurring in less than 1-4% of cases.