Cancer Immunotherapy refers to any form of cancer treatment that uses the immune system to target cancer cells.
Active immunotherapy using checkpoint inhibitors is an emerging form of cancer treatment which uses monoclonal antibodies to stimulate anti-tumor T-cell activity.
Ipilimumab is a cytotoxic T-lymphocyte antigen-4 (CTLA4) checkpoint inhibitor.
CTLA4 blocks T-Cell activation when it binds to B7.
Ipilimumab,
which binds to CTLA4,
prevents this interaction,
thus stopping the downregulation of the T-cell immune system.
Another immune checkpoint that can be targeted is the programmed cell death protein-1 (PD-1) or its ligand PD-L1,
which normally interact to prevent T-cell activation.
Once this interaction is interrupted there is increased likelihood of triggering the killer effector function of the T-cell and destroying the tumour cell that had previously been protected by the PD-1-PD-L1 interaction.
Examples of a PD1-PDL1 checkpoint inhibitors are nivolumab and pembrolizumab,
which have recently received FDA approval.
A significant increase in overall survival (OS) in melanoma patients on ipilimumab is now well established with recent pooled analysis reporting median OS of 11.4 years and 3 year survival rate of 22% [1].
Anti-PD-1 antibodies such as nivolumab and pembrolizumab have also demonstrated survival benefit in melanoma,
of up to 44%,
and have each also received FDA approval in the treatment of melanoma.
Immunotherapy is not limited to the treatment of melanoma with multiple clinical trials demonstrating efficacy in other cancers,
more commonly lung,
breast,
prostate and renal cancers.
For example,
nivolumab has a significant 1-year OS of 47% in the treatment of non-small cell lung cancer [2].
There are many other clinical trials examining immunotherapy in the treatment of many other solid tumours such as ovarian,
colorectal,
bladder,
brain and squamous cell head and neck cancers [3-5].
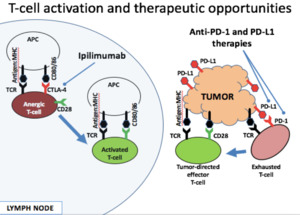
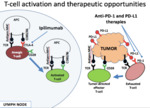
Fig. 1: CTLA4 acts to amplify the activation and clonal expansion of T-cells more centrally.
PD1/PDL1 Modulating T-cell activity within the periphery, including the tumor microenvironment specifically.
Courtesy Dr. Matt Hellman
References: Memorial Sloan Kettering Cancer Center, New York, United States