This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Computer applications, Oncology, MR-Diffusion/Perfusion, Computer Applications-Detection, diagnosis, Neoplasia, Abscess, Metastases
Authors:
G. C. Manikis1, K. Nikiforaki1, G. Ioannidis1, N. Papanikolaou2, K. Marias1; 1Heraklion/GR, 2Lisbon/PT
DOI:
10.1594/ecr2017/C-2964
Results
Synthetic Data
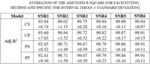
The fitting accuracy of each fitting scheme is displayed in Fig. 1.
All data exhibited an overall adj-R2 above 90% and surpassed more than 98% for the five out of six SNR groups. Repeatability and variability measures were applied to the four examined methods to confirm robustness in their fitted results and not for comparative purposes (see Fig. 2). Repeatability and goodness of fit levels of the proposed and the standard fitting scheme exhibited no significant changes,
excluding thus any other factor of influence in the results.
The optimization scheme reduced the relative fitting error especially in cases where noise affects significantly the diffusion signal.
A noticeable change on the relative error,
when the proposed optimization scheme was applied in both partial and complete fitting,
was observed in the low SNR range (see Fig. 3).
For D and f there was an insignificant number of pixels converging to the upper bound values that only surpassed a maximum level of 2% and 1.5% for the lower SNR range,
indifferently of the method.
For all SNR intervals there was significant reduction of the percentage of D* erroneously attributed the upper boundary value (38% to 17% from the lowest SNR level to the highest) as seen graphically in Fig. 4 and Fig. 5.
Clinical Data
Apart from synthetic data,
the optimization fitting scheme was applied and tested on clinical 1.5T MRI data on highly perfused abdominal organs,
such as the liver and pancreas using in-house software [5].
Image acquisition has the same b-value set as the synthetic,
while the measured SNR of the specific ROIs lies in the SNR1 range.
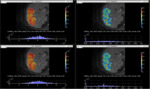
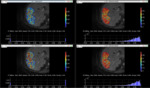
As seen in Fig. 6 both standard and proposed complete fitting schemes showed same results for D and f in case of liver parenchyma.
The upper bound percentages of the fitted D* reduced by 48% with mean value of adj-R2 equal to 95% and 94% in case of CP and CS respectively (see Fig. 7).
Similarly,
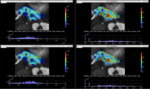
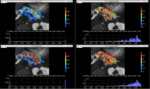
when CP and CS were applied to pancreatic areas,
both standard and the proposed scheme showed equivalent results for D and f (see Fig. 8) but a reduction of 75% for the upper bound percentages of the fitted D*was achieved (see Fig. 9).