Etiology
The most common cause is bacterial, being the most frequent bacteria Neisseria gonorrhoeae and Chlamydia trachomatis.
These germs can enter the female superior genital structures in different ways:
● Spread upward from the uterine cervix. It is the most often implicated mechanism in infection and it is related to sexual transmission.
It usually involves the germs indicated above.
● Spread by continuity from other nearby infectious processes,
as periappendicular abscesses or acute diverticulitis.
● Hematogenous spread. Very rare,
such as tuberculosis.
Risk factors are all activities which may encourage upward spread from the cervix as high frequency sexual relations,
especially in cases of multiple sexual partners by infection from these,
or medical or surgical manipulation of these structures such as the placement of intrauterine devices.
Clinical semiology
It is very nonspecific and variable. Since both clinical and analytical,
to different degrees of manifestation of unspecific symptoms,
among which include fever,
dyspareunia,
hypogastric abdominal pain,
increased adnexal or cervical sensitivity.
It is also possible a completely asymptomatic state.
Therefore,
given the unspecificity of the clinical symptomatology,
it is important to use imaging techniques for the diagnosis.
Imaging
Prior to the advent of imaging techniques,
the diagnosis of pelvic inflammatory disease was performed by laparoscopy.
Thus,
direct visualization of the structures involved in this disease is achieved,
finding purulent exudate and edema.
Currently,
imaging techniques allow knowing the status of internal organs without invasive procedures.
The imaging technique that allows better visualization the upper female genital tractor is transvaginal sonography,
supplemented occasionally with abdominal ultrasound.
However,
the diagnosis is commonly achieved by using computed tomography.
In this paper we focus on the description of the findings of pelvic inflammatory disease on CT based on the severity of the disease.
● Very mild disease. Findings can be very subtle,
and CT can be normal.
● Mild sickness. Discrete inflammatory changes in the pelvic region manifested as thickening,
hyperemia and edema of fascial planes and ligaments,
as the broad ligament or uterosacral ligaments,
with effacement of fat planes between them.
Other findings include reactive lymphadenopathy (often affects abdominal lymph,
to the level of the renal vessels) and the presence of free intraperitoneal fluid,
which frequently accumulates at the pouch of Douglas.
Depending on the affected structure,
you can find.
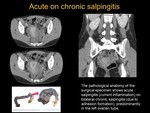
○ Salpingitis (see Figure 1). On these cases fallopian tubes are affected.
Thickening and hyperemia of these structures,
fascial planes and surrounding fat can be observed.
Significant thickening is considered if greater than 5 mm.
○ Oophoritis. It involves inflammation of the ovaries.
They appear enlarged (over 3 cm in diameter) with marked enhancement after contrast administration due to hyperemia.
Another characteristic finding is the presence of multiple cysts of small size (between 2 and 10 mm diameter).
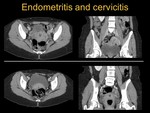
○ Endometritis (see Figure 2).
It is characterized by enhancement of the myometrium or endometrium after contrast administration and presence of fluid within the endometrial lumen.
○ Cervicitis (see Figure 2).
In the case of inflammation affecting the cervix.
● Serious illness. It is not very frequent in our environment.
However,
given its severity,
it is important to identify it.
If the inflammatory process progress,
related radiological signs appear,
like abscess formation.
These may affect only the fallopian tube.
In that case,
it is called pyosalpinx.
 ○ It should not be confused with hydrosalpinx. In this case occurs an obstruction to drainage of the fluid secreted by the tubes (one of its causes is the formation of adhesions inside these structures,
by previous inflammatory processes).
In the case of hydrosalpinx,
the contents of the tube will be liquid (hypodense and homogeneous) unlike pus (denser and heterogeneous).
Moreover,
the walls of the tube should not show increased contrast uptake (because there is no hyperemia).
○ It should not be confused with hydrosalpinx. In this case occurs an obstruction to drainage of the fluid secreted by the tubes (one of its causes is the formation of adhesions inside these structures,
by previous inflammatory processes).
In the case of hydrosalpinx,
the contents of the tube will be liquid (hypodense and homogeneous) unlike pus (denser and heterogeneous).
Moreover,
the walls of the tube should not show increased contrast uptake (because there is no hyperemia).
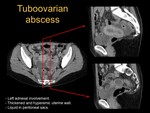
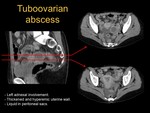
○ Another possibility is that the inflammatory process combines affection of tubes and ovaries.
In this case,
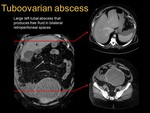
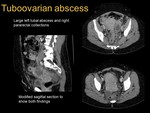
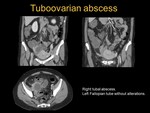
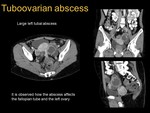
it is possible to develop a tuboovarian abscess (see images 3,
4,
5,
6,
7 and 8).
If pus is retained in the uterus,
it is called pyometra.
● Involvement of adjacent structures. In cases of severe disease,
it may secondarily affect other structures.
To assess this involvement it is especially useful the CT,
since ultrasound is very limited.
○ Affectation of the digestive tract. Inflammation can secondary affect loops of gut and colon.
As a result it can appear an obstructive syndrome.
■ Acutely, obstructive symptoms can be both mechanical and paralytic caused by bowel loops and colon irritation from adjacent inflammatory disease.
■ Chronic inflammation produced by pelvic inflammatory disease produces adhesions that can lead to mechanical obstruction.
○ Affectation of the ureters. Similarly to digestive tract,
it can be affected both acute and chronically.
In this case,
it will appear hydroureter or ureterohydronephrosis,
depending on the severity and course of the disease.
○ Affectation of the peritoneum. It may produce local inflammation and peritonitis.
Through peritoneum,
inflammation can spread to other organs.
Severe peritonitis would be developed in case of breakage of tuboovarian absces.
● Affectation of remote structures. This impairment can be assessed only by CT.
○ Thrombosis or thrombophlebitis of the gonadal vein. As a result of the inflammatory process,
a hypercoagulable state would appear.
This can lead to in thrombosis or thrombophlebitis of gonadal veins.
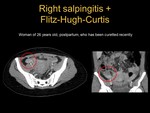
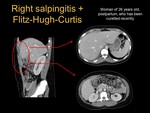
○ Fitz-Hugh-Curtis syndrome (see pictures 9 and 10). It is caused by the arrival of the bacteria responsible for the PID to the perihepatic space.
They can reach this region through paracolic or lateroconal fascia,
through vascular structures (gonadal veins) or lymph leak.
In imaging studies inflammation of fat and increased uptake of the liver capsule is observed.
It is also possible to see cholecystitis-like findings,
as thickening of the wall of the gallbladder and inflammatory changes in perivesicular fat.
Treatment
Treatment is different depending on the severity of diagnosed pelvic inflammatory disease.
It is therefore important to establish the proper diagnosis.
● For milder forms of the disease,
treatment is oral antibiotic therapy.
If there is no improvement,
parenteral treatment should be administered.
● If intraabdominal abscesses or collections are discovered,
percutaneous or surgical drainage will be required.
● In cases of severe disease,
hysterectomy and / or oophorectomy will be needed.