Before all procedures all patients were evaluated by a multidisciplinary team composed by radiologist,
oncologic paediatrics,
paediatric surgeon and anaesthesiologist.
A thorax CT scan or PET-CT scan [18] was performed for each patient as previous imaging investigation.
Informed consensus was obtained from parents and children were involved in the explication of the procedure.
This was fundamental for the collaboration of little patients during procedures only under local anaesthesia.
For each patient coagulation profile was checked (platelets ≥ 25000 mm3 and INR <1,5).
For CT-guided procedures we obtained low-radiation dose protocol using a 64-slice CT scanner.
Patients’ position was prone,
supine or lateral decubitus,
depending on the location of the lesion.
A scan was obtained to calculate the needle point of entry and its path.
We marked the entry point with a felt-tip pen using the laser grid of the gantry.
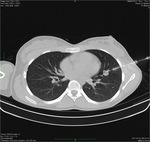
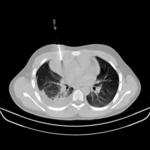
In the case of lung nodules we always chose the shortest transthoracic distance from the target tissue and the pleura avoiding vital structures; we obtained sequential CT images after each manipulation of the needles (between 3 and 10 images).
All biopsies were performed applying the coaxial technique to diminish the number passes through the visceral pleura,
reduce the risk of pneumothorax and obtain a higher number of specimens.
Coaxial technique has been used since 1990’s [19] for biopsies of small pulmonary nodules in children and permitted to obtain adequate cores without significant morbidity.
In our case,
after injection of subcutaneous lidocaine,
we inserted a puncture sheath (16 G) and a semiautomatic biopsy hand with quick release mechanism (18 G),
obtaining almost three samples for each patient,
soaked in jars of formalin and sent to laboratory investigation.
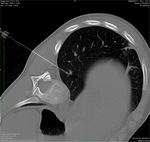
The localisation of lung nodule before surgery previewed the CT guided positioning of two 20 G hook wires for each nodule.
The introducer needle was inserted through the skin,
and after sequential CT images control to confirm the position of needle beyond the nodule,
it was removed over the hook wire.
A final image control was obtained to confirm the correct position of hook wires.
Then the patient was transferred to surgery room.
In only one patient we performed US-guided to biopsy an anterior mediastinal mass; in this case we apply a needle bracket to the linear probe (9 MHz) and performed biopsy with coaxial technique.
In the majority of cases reported in literature thoracic biopsies required general anaesthesia [20],
especially in patients younger than 15 years old.
According to all multidisciplinary group,
we preferred to perform procedures under sedation or local anaesthesia,
depending on the compliance of patients.
Anesthesiological evaluation was obtained for all patients,
but in our group only four biopsies required sedation; in the other biopsies,
performed using only local anaesthesia,
there was excellent compliance of patients.
In any case during all procedures patients were monitored by the anaesthesiologist.
Nodules localisation with hook-wire was performed immediately before surgery,
using the same sedation for the intervention.
Adequate core biopsies were obtained in all patients; in one case histological examination showed false negative results and surgical evaluation was performed.
The hook wires were successfully positioned in all cases preventing more invasive intervention; their exact location was also confirmed by pathological examination Post procedure period was always normal; we observed two perilesional haemorrhages and one pneumothorax,
but none of them required treatment.
All biopsied patients avoided other invasive investigations,
except the non-diagnostic case who underwent to thoracotomy.
Both hook wires positioning were targeted and useful for lung lesions finding during the surgery.