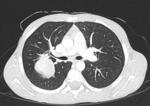
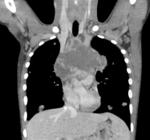
Percutaneous transthoracic procedures are commonly performed in adult patients with lung nodules or mediastinal masses.
Needle biopsies permit to obtain an histological diagnosis which is fundamental to improve therapeutic planning and determine the prognosis of patients.
Hook wire positioning is used to spare lung tissue when surgical resection of nodule is required.
Even different studies confirm their safety and feasibility in adults,
there is little literature about transthoracic procedures in paediatric population.
Paediatric thoracic pathology is routinely detected using multidetector CT,
which permits depiction also of small structures [1].
Focal lung paediatric pathology includes benign nodules such as hamartomas,
chondromas,
granulomas,
IMTs (inflammatory myofibroblastic tumours) [2-4],
while malign nodules are frequently metastases (10-30% of paediatric solid tumours) [5],
especially from osteosarcoma,
hepatoblastoma and Wilms tumour [6],
but also primary malignancies like carcinoid tumours,
adenocarcinoma and bronchoalveolar carcinomas [7].
Mediastinal space-occupying lesions in the anterior compartments in paediatric patients include lymphoma,
bronchogenic or pericardial cysts,
thymic diseases and germ cell tumours (GCTs 6-18% of paediatric mediastinal neoplasm) [8,9].
Thymoma incidence is higher between the 4th and 5th decade,
but even if it is uncommon in children there are few cases reported [10].
CT technique is the most frequently chosen for transthoracic procedures because it offers high quality images and in case of needle biopsies it allows sparing of lung tissue and time in alternative to surgery.
Nowadays patients’ radiation exposure can be highly reduced using proper parameters of tube current and voltage [11].
Ultrasound is less specific in the determination of masses and nodules,
but it uses non-ionizing radiations.
Types of lesions most frequently detectable with US are subpleural lesions and huge mediastinal masses.
The most frequent complications reported for transthoracic biopsies are described for whole population (paediatric and adult patients) and are pneumothorax (5-64%),
haemorrhage along the needle path or in perilesional lung tissue and haemoptysis (5-7%) [12-15].
Pneumothorax is more frequent if there is emphysema or the lesion is less than 2 cm deep from the pleura.
It requires chest tube drainage in 2-17% of cases.
It can be seen during the procedure,
immediately after,
or later at chest x-ray control.
In our case patients underwent a control chest radiogram after 2 hours by the end of the procedure and remained under observation for 24 hours.
From April 2016 to August 2017 we performed percutaneous transthoracic procedures in 9 patients between 6 and 17 years,
5 males and 4 females; 4 patients underwent to CT-guided lung needle biopsies and 2 to mediastinal lesion biopsies.
One patient underwent to US-guided mediastinal needle biopsy.
Two patients with lung nodules underwent to CT-guided pulmonary nodules hook wires localisation immediately before surgery [16,17].