The thymus arises from the third and fourth pharyngeal pouches in the sixth week of gestational life 1.
It is in the course of the seventh week when the thymic nuclei migrate medially and caudally,
forming the so-called thymsopharyngeal conduit,
until its final location that will take place in the anterior portion of the mediastinum 1,2.
The accessory ectopic thymic tissue can appear at any point of the path of the thymsopharyngeal duct,
which extends from the mandibular branch-angle to the cranial portion of the mediastinum,
and this is mainly due to failure in the involution of ectopic thymic remains or failure in the migration.
Likewise,
the ectopic thymic tissue presents as solid,
cystic,
or solid-cystic images.
The majority of the thymic tissue located in the neck has a unilateral distribution and tends to be located in the left,
for reasons that have not yet been explained consistently.
The ectopic cervical thymus is a rare entity and usually presents as a cervical mass without associated symptoms,
or it can also present as a swollen and edematous neck on physical examination.
Up to half of the cases this occurs in children between the ages of 2 and 13,
and is slightly more common in boys than girls 2,3.
If they reach the size necessary to cause mass effect and cause compression with displacement of the adjacent structures,
they will cause a clinical dysphagia,
hoarseness or stridor,
as main symptoms.
Magnetic resonance imaging,
CT and ultrasound imaging are fundamental from the start,
in which the general radiologist or pediatric radiologist can suggest in the differential diagnosis of a cervico-thoracic mass that is ectopic thymic tissue.
However,
the definitive diagnosis is obtained by histology,
either with a needle core biopsy (usually 18G caliber) or by fine needle puncture aspiration (PAAF,
with 21-22G caliber needles usually) 2,3,4.
The echographic image is characteristic,
with a hypoechoic cortex and an echogenic layer corresponding to the medulla,
which contains echogenic and linear septa.
The vessels that run between the septa are visualized as discrete echoes of high echogenicity,
which do not always have color or energy Doppler.
At MRI,
the intensity of the tissue signal is the same as that of the mediastinal thymus,
that is,
it is usually isointense in T1 sequence with respect to the muscle,
and mild to moderately hyperintense in T2 sequence with respect to the muscle.
Tipically demonstrates chemical shift artefact between in and out of phases images.
At the CT imaging,
it is shown as a homogeneous tissue with soft tissue density,
with 60-80 HU,
and presenting a similar attenuation to the musculature.
It presens a smooth outline with convex borders in childhood (triangular in adulthood) 4.
The tissue of the ectopic thymus involves in childhood at the same rate that involutes the thymus tissue of orthotopic location 1.
The most important thing is to know that sometimes a small portion of thymic tissue in the neck of children can appear in the radiological study,
and it is important not to confuse with adenopathies or tumors,
which obviously have other implications for treatment and follow-up 1,3.
The homogeneity of the tissue and,
above all,
the contiguity with the thymic tissues located in the mediastinum are findings that should point towards a benign process in general,
and thymic tissue in particular.
Sometimes within the thymic tissue appear rounded and anechoic formations to the echographic study,
and that correspond with cysts,
which occur more frequently in the ectopic thymus than in the thymus of mediastinal location 1,4.
If there is inflammation or acute bleeding in the thickness of the ectopic thymic tissue,
the increase in local size may later reveal the existence of an ectopic thymus.
The differential diagnosis includes (specially for ectopic cervical thymus)1,2,3:
Branchial cleft cyst.
Cystic teratoma.
Thyroglossal cyst.
Esophageal duplication cyst.
Reactive adenopathy.
Lymphoproliferative disorders.
Malignant neoplams (rhabdomyosarcoma,
neuroblastoma).
Lipoblastoma.
Timolipoma.
CLINICAL CASES:
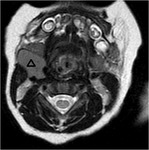
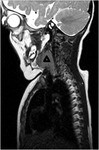
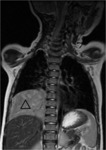
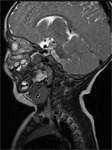
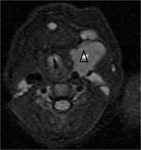
Case nº1: 6-month-old boy with 22q11.2 delectin syndrome diagnosed shortly after birth.
Column MRI is performed to rule out dysraphisms.
As a casual finding,
a right cervical structure was identified that through biopsy was found to correspond to ectopic thymic tissue of cervical location.
Figures 1 and 2.
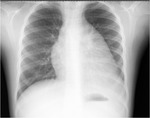
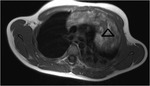
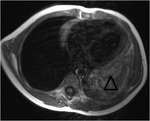
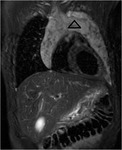
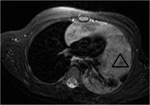
Case nº 2: 6-year-old boy with incidental chest radiograph finding.Large mass with a broad thoracic extension that finally confirmed by biopsy that it was a thymolipoma.
Surgery was performed to remove it,
without further problems.
The detailed description of the imaging techniques is described in the images.
Figures 3-8.
Case nº 3: A 20-month-old boy with Marfan syndrome who presents with fever with peaks up to 39.5ºC.
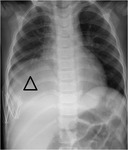
Chest radiography was performed,
visualizing a effacement of the right cardiofrenic and costophrenic angles,
of a non-infectious aspect,
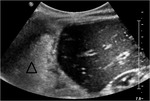
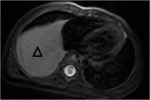
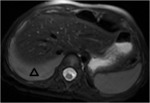
so it was decided to perform an ultrasound and then a MRI.
The mass described in the studies was biopsied,
with the result of being thymic tissue of normal characteristics.
Figures 9-13.
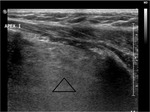
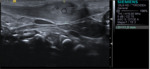
Case nº4: A 9-month-old boy in whom ultrasound is performed due to suspicion of a haematoma in the sternocleidomastoid muscles.
At ultrasound: Posterior and inferior to the right submandibular gland,
a structure of size 15 x 35 mm (AP x T) is observed (triangle in figures),
with well-defined margins,
no mass effect or englobing vessels,
and an echo-structure similar to thymus tissue visualized inferiorly.
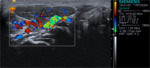
It has vascularization.
Due to the location and internal characteristics,
an ectopic thymus should be ruled out as the first possibility.
Biopsy: Thymic tissue.
Figures 14-16.
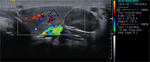
Case nº5: A 10-month-old girl with a cervical mass detected by ultrasound,
defined as a well-defined solid mass,
with a left latero-cervical location with color Doppler in the interior,
which makes it necessary to rule out hemangioma or neuroblastoma by location and age,
or thymus with ectopic location.
MRI was also performed.
Biopsy: thymic tissue.
Figures 17-20.