Normal nerve,
axial plane → "honeycomb"
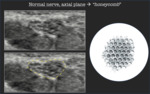
Normal nerve,
longitudinal plane → "rigatoni sign"
From the histologic point of view,
a normal nerve has an external sheath (the outer epineurium) which surrounds the nerve fascicles.
The connective tissue between the outer epineurium and the fascicles is the interfascicular epineurium (or internal epineurium) [1,2].
On axial plane,
high resolution ultrasound shows the nerve as an “honeycombed structure” composed of hypoechoic spots in an hyperechoic background.
The hypoechoic spots correspond to the fascicles that run longitudinally within the nerve; the hyperechoic background represents the interfascicular epineurium [1,2] (Fig.1).
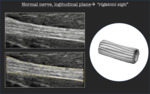
On longitudinal plane,
the nerve assumes an elongated appearance with hypoechoic parallel bands,
which represent the neuronal fascicles,
separated by the hyperechoic bands (interfascicular epineurium) [1,2] (Fig.2).
Ulnar nerve between flexor muscles → "butterfly wings"
The ulnar nerve,
approximately 1 cm distal to its passage in the ulnar groove (an osteofibrous channel where the nerve has a very superficial location) enters the proper cubital tunnel,
that is an important site of nerve compression,
and then lies between the ulnar and the humeral head of the flexor carpi ulnaris muscle [2].
The nerve with the flexor muscles takes on a configuration comparable to the “butterfly wings” (Fig.3).
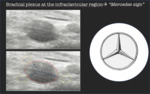
Brachial plexus at the infraclavicular region → "Mercedes sign"
Ultrasonography is an useful tool to depict normal brachial plexus anatomy at several levels including the paravertebral,
interscalenic,
supraclavicular,
infraclavicular and axillary regions.
The study of the brachial plexus is very important to evaluate eventual nervous lesion that may compromise the upper limb mobility.
The brachial plexus is formed by the union of the ventral roots of nerves from C5 to T1,
extending from the cervical spine to the axilla,
and it gives rise to important peripheric nerve of the upper limb,
among which radial,
ulnar and median nerves.
The union of the ventral roots forms three nervous trunks: upper (C5-C6),
medium (C7) and lower (C8-T1),
which course in the interscalenic plane.
At the infraclavicular region,
they form three cords: posterior,
medial and lateral,
in relation to the axillary artery.
This particular configuration remembers the symbol of an important car company,
that of Mercedes [2,
3] (Fig.4).
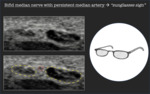
Bifid median nerve with persistent median artery → "sunglasses sign"
A bifid median nerve is an anatomic variant of median nerve.
It’s characterized by the presence of two trunks of median nerve (a radial trunk and an ulnar trunk).
The persistent median artery is an accessory artery that arises from the ulnar artery and accompanies the median nerve along its course.
If the median nerve is bifid,
the artery lies between the two nerves trunks and this configuration remember the shape of “sunglasses” (Fig.5).
A persistent median artery is a common condition in healthy people and can be related to median nerve anatomic variations. The persistent median artery has a superficial course close to the transverse carpal ligament and his presence is an important information for the surgeon for preoperative planning because the artery can be injured during arthroscopic release of the transverse carpal ligament [2,4].
A bifid median nerve is a condition relatively frequently in patient with carpal tunnel syndrome.
The relatively higher cross sectional area of a bifid median nerve is more commonly associated with compression of the nerve in the carpal tunnel.
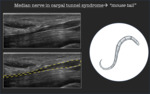
Median nerve in carpal tunnel syndrome → "mouse tail"
The carpal tunnel is an osteofibrose canal where 9 tendons (4 of the superficial flexor tendon,
4 of the deep flexor tendon and the longus flexor tendon of the thumb) and the median nerve pass.
It is posteriorly delimited by carpal bones (scaphoid and trapeze laterally,
pisiform and hamate medially) and anteriorly by flexor retinaculum (normal thickness 1-1,5 mm).
The carpal tunnel syndrome consists of a compression of the median nerve and occurs mostly in women about 45-50 years.
Sensibility disorders are the typical clinical presentation,
with dysesthesia/paraesthesia in the innervation territory (first three fingers and the radial half of the annular).
It may be caused by space-occupying lesions (as cysts or lipomas),
anatomical variants (bifid median nerve) or direct injury of the nerve (acute o chronic).
Diagnosis is confirmed by electroneurography.
Ultrasonography is very useful to evaluate the cause of this syndrome and the suffering signs of the nerve.
One of the most important signs of nervous compression is the abrupt caliber reduction of median nerve when it passes under flexor retinaculum,
especially visible in sagittal scan,
similar “to a mouse tail” (Fig.6).
Other suffering signs are the loss of typical follicular aspect,
the reduction of nerve mobility at dynamic tests and the section surface increase ( normal value ≤9mm2 or ≤15mm2) [2,5].
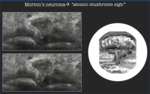
Morton's neuroma → "atomic mushroom sign"
Morton’s neuroma is a perineural fibrotic process of common digital plantar nerve.
It occurs mostly in middle-aged women and causes metatarsal pain,
radiating to the fingers.
Principal risk factors are overweight and high heel shoes.
It essentially affects II and III inter-metatarsal spaces.
The ultrasonography examination is performed with Mulder test,
to facilitate the visualization of the lesion: the examiner exercises a lateral pression on the forefoot,
to enucleate Morton’s neuroma from the intermetatarsal space.
It appears as a ovoidal hypoechoic lesion between metatarsal heads,
better viewed on axial plane,
very similar to an “atomic mushroom” (Fig.7); however,
it must be differentiated from an intermetatarsal bursitis [5].
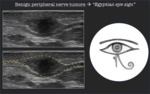
Benign peripheral nerve tumors → "Egyptian eye sign"
A peripheral nerve sheath tumor is a soft-tissue neoplasm derived from Schwann cells.
The most common types of benign peripheral nerve tumors are Schwannomas and Neurofibromas,
that are difficult to distinguish with imaging.
Malignant transformation is rare but can occur with both neurofibromas and schwannomas [2].
Both benign peripheral nerve sheath tumors (schwannomas and neurofibromas) and malignant peripheral nerve sheath tumors have variable sonographic features.
More commonly,
they appear as a solid hypoechoic mass in direct continuity with a nerve at its proximal and distal poles [2].
This shape recalls "the Egyptian eye",
one of the most famous and immediately recognizable symbols of ancient Egypt (Fig.8).
Schwannoma is a slowly growing encapsulated tumor,
found more commonly in the extremities.
It appears as a globoid mass located along a nerve and eccentric to the nerve axis.
At color and power Doppler examination hypervascularization is typical.
Neurofibroma appears as a fusiform fashion with the nerve entering and exiting from the extremities of the lesion.
Neurofibromas may present as a solitary mass or as multiple masses as part of neurofibromatosis.
There are three types of neurofibroma: localized,
diffuse and plexiform (associated with Neurofibromatosis I) [2].
Malignant peripheral nerve tumors are indistinguishable from schwannoma and neurofibroma.
It can appeas with indistinct margins and adhesions of the mass with surrounding tissues and it can increase in size rapidly [2].
The role of ultrasound is to identify the lesion and to give preoperative assessment of the extent of the disease.
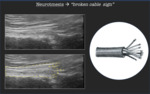
Neurotmesis → "broken cable sign"
Sunderland in 1951 described five degrees of peripheral nerve injury [6]:
-Neuroapraxia (Sunderland I)
-Mild axonotmesis (Sunderland II,
Sunderland III)
-Severe axonotmesis (Sunderland IV)
-Neurotmesis (Sunderland V).
Neurotmesis is the breaking of the nerve,
with loss of continuity of the entire nervous trunk [6,7].
We can consider the nerve as a cable like structure,
in which fascicles runs separately throughout the entire nerve length.
When the rupture of the nerve occurs,
the end trunk of the nerve appears as “a broken cable” (Fig.9).
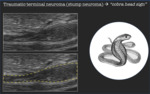
Traumatic terminal neuroma (stump neuroma) → "cobra head sign"
Traumatic neuroma may occurs from acute or chronic injury to a nerve.
After a peripheral nerve lesion,
the mechanical trauma leads nerve’s regeneration.
The terminal neuroma occurs after transection of the nerve.
The typical histopathologic features of a neuroma are nerve fibers and fascicles in various stages of maturation and varying orientation with the presence of scar tissue [7,8,9,10].
Clinically,
a neuroma can be either asymptomatic or symptomatic.
If symptomatic, the pain is the most important feature together with altered sensation in the distribution of the involved nerve.
The typical ultrasound appearance of neuromas is that of an ovoid,
well defined, incompressible, hypoechoic region of focal swelling in continuity proximally with a normal nerve,
resembling a “cobra head” in the longitudinal scans [7,8,9,10] (Fig.10).