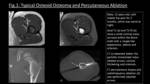
OO is a painful,
benign and common tumor,
accounting for 3% of all bone neoplasms.
The nidus,
in other words,
the tumor itself,
is small (1,2,3) and consists of osteoid matrix with variable mineralization,
osteoblasts and some osteoclasts surrounding the lesion,
interspersed by a vascular conjunctival stroma,
with inflammatory changes and reactional bone formation around the lesion (4,5).
The tumor is more prevalent in caucasians male adolescents and young adults between 7 and 25 years of age (6-11).
The typical clinical picture is intermittent pain worsening at night and relieved by salicylates(12,13).
In atypical cases,
different symptoms may be present,
such as redness and local tenderness in lesions close to the skin,
synovitis when intra or juxta-articular (9),
or even a painless clinical setting,
mainly in the phalanges of the hands and feet (14).
The pain physiopathology seems to be related to a high osteoblastic activity leading to high levels of prostaglandins synthesis and a simultaneous peripheral osteoclastic bone resorption,
increasing pressure in an innervated bone area within the nidus and particularly in the reactive zone (12,15-18).
The OO more often involves the diaphysis followed by the metaphysis of the long bones.
In the axial plane,
there are two forms of classification of the OO,
the traditional one and more used,
by means of plain radiographs,
where the lesion is classified as cortical,
medullary or subperiosteal; and the more recent,
however less used,
through axial sectional methods in which the lesion is divided into cortical,
medullary,
subperiosteal and endosteal (19-21).
The femur and tibia account for more than 50% of cases,
the humerus is also a frequent site.
The spine,
hands,
and feet correspond to approximately 30% of the cases; the skull,
scapula,
pelvis,
ribs,
mandible and patella are rarer sites (21,22).
In the axial skeleton,
the lumbar spine is the most affected,
followed by the cervical,
thoracic and sacrum,
highlighting that the posterior elements are involved 90% of the cases.
The diagnosis is made by the clinical picture and imaging tests,
whilst biopsy is recommended at the time of treatment (13),
especially in atypical cases (23).
Treatment options are surgical block resection or percutaneous imaging guided treatment (24-26) (fig 1).
As OO presents a natural history with spontaneous regression in 6 to 15 years that can be reduced to 2 to 3 years with the use of nonsteroidal anti-inflammatory drugs,
pharmacological treatment is also an option,
however,
due to the adverse effects of prolonged use of these medications,
this option is reserved only for exceptional situations (27-29).