Neuroangiography is an integral investigation in the management of patients with neuro- vascular diseases.
It is used for diagnosis,
but in many instances,
may be followed up with interventional treatment in the same sitting.
[1]
A sound understanding of the principles of appropriate periprocedural care and anatomy,
angiography technique and angiographic appearance of pathology are vital for the test to be diagnostic.
(I) Salient descriptors of normal neurovascular anatomy [1,
2]:
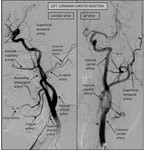
(A) Extra cranial carotid system (Figure 1):
· Common carotid artery
Left CCA form the aortic arch and right CCA from the brachiocephalic trunk.
· External carotid artery.
From the upper border of the thyroid cartilage (C4 vertebral level) to terminal branches
Branches:
I. Superior thyroid artery
II. Ascending pharyngeal artery
III. Lingual artery
IV. Facial artery
V. Occipital artery
VI.
Posterior auricular artery
VII.
Terminal branches à Superficial temporal and Internal Maxillary arteries.
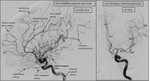
(B) Anterior circulation (Figure 2)
· Internal carotid artery (ICA): Bouthillier classification,
from below upwards:
C1 – Cervical segment.
From the common carotid bifurcation to entry into carotid canal.
C2 – Petrous segment.
Completely within bony carotid canal.
Small branches not appreciable on DSA.
C3 – Laceral segment.
Upto the Petro lingual ligament.
First 1cm of the ICA after exit from the carotid canal.
C4 – Cavernous segment.
Upto the proximal dural rim,
just inferior to the clinoid process.
Branches are Meningo hypophyseal trunk and infero lateral trunk.
C5 – Clinoid segment.
Smallest segment,
by the side of the anterior clinoid segment.
Ophthalmic artery can arise from it,
else no significant branches.
C6 – Ophthalmic segment from distal dural ring upto posterior communicating artery.
C7 – Communicating from PCOM to ICA bifurcation.
Physiology Phases:
Circulation time: time taken from contrast reaching the cavernous ICA to first cortical vein; Around 3.5 seconds is normal.
It represents the physiological perfusion time.
> 7seconds is abnormal.
Arterial,
capillary (parenchymal) and venous at least in two different planes need to be assessed.
· Middle Cerebral Artery:
M1 - Upto insula,
not the bifurcation.
The bifurcation can be of the early or lateral type.
M2 - Curved course over the surface of the insula.
M3 - Descends along the circular sulcus of the insula / operculum upto the cortical surface.
M4 - Along the convex cortical surface.
· Anterior Cerebral Artery:
A1 - From ICA bifurcation to anterior communicating artery.
A2 - ACOM to origin of the Pericallosal and Calloso marginal artery.
A3 - Distal branches supplying cortex.
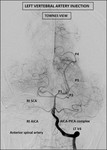
(C) Posterior circulation (Figure 3)
· Vertebral artery:
V1- Origin from SCA to Foramen transversarium of C6
V2 – C6 to C1 foramen transversarium (Acute bend in course)
V3 – C1 to dura (focal constriction);
V4 – Intra dural part of vertebral artery.
· Basilar artery:
Branches:
Anterior Inferior Cerebellar Artery versus Posterior Inferior Cerebellar Artery balance à supplement each other.
Basilar perforators – not seen on DSA.
Superior Cerebellar Artery
· Posterior Communicating Artery:
P1- Basillar bifurcation to posterior communicating artery.
P2 – Around the ambient cistern up to posterior margin of midbrain
P3 - within quadrigeminal plate cistern
P4 – Enters parieto-occipital and calcarine sulcus.
Branches: Thalamo perforator,
Posterior medial choroidal,
Lateral choroidal and Splenial artery.
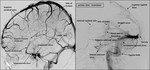
(D) Venous anatomy: superficial and deep venous system are detailed and marked in the images provided.
(Figure 4)