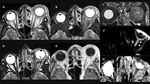
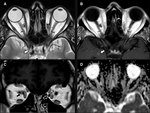
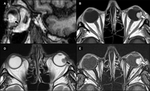
Compartmental Analysis
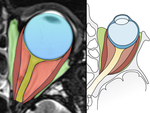
Orbits can be divided by their anatomical components,
from the outer margins to the core,
which is the globe/optic nerve complex.
(Figure 1).
Due to the high spacial resolution of CT and MR imaging,
arising tissue and compartment of specific pathologies can be identified,
therefore better diagnostic possibilities and orbital extension can be identified.
Dedicated orbital MR protocols include axial and coronal T1,
T2 both with fat suppression and axial and coronal T1 post contrast.
Bone involvement could require a CT with bone algorithm reconstruction for better spacial resolution.
Orbital Wall
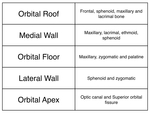
Orbits are formed by seven separate bones which couple together in to a piramidal structure with an apex and a base or opening.
They are in direct relationship with the paranasal sinuses being medially separated by a very thin structure called the lamina papyracea (Table 1).
Multiple osseous lesions can involve the orbital bony components,
including fibrous dysplasia,
primary tumours,
scarring from prior trauma and metastasis.
Less common conditions go from expansive to hyperostotic lesions.
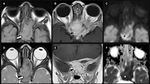
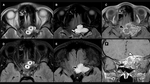
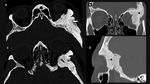
Some diagnosis to keep in mind are the granulomatous conditions like the Langerhan’s cell hystiocytosis (figure 2),
cystic lesions like the aneurysmal bone cysts (figure 3),
solid lesions like the osteoid osteomas and their atypical presentations (figure 4) and the hyperostotic reaction provoked by the meningiomas (figure 5).
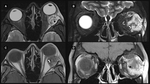
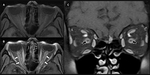
Extraconal Space
The inner aspect of the orbital chamber is covered by a strong soft tissue lining known as periorbita.
It protects the orbital components from the possible spread of infection through the natural dehiscences and sutures.
Immediately after the periorbita there is a fatty compartment called the extraconal space with support and nutritious functions.
(Figure 6).
Lesions arising merely from the extraconal are rare and most of the cases are the result of extension from bony,
paranasal sinuses and outer extension from the muscular cone pathologies.
Some other conditions like metastasis (figure 7) and infection,
specially in immunosupresed patients (figure 8),
have to be kept in mind.
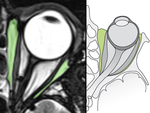
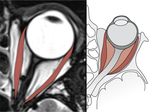
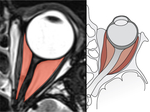
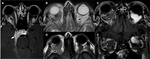
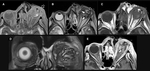
Orbital Muscles
Ocular movements are performed by the action of six muscles in each side.
Together they form a cone inserted in the orbital apex (figure 9),
surrounding part of the superior orbital fissure and the optic canal with a fibrous ring called the annulus of Zinn.
Common pathologies affecting the extraocular muscles are thyroid orbitopathy (Graves disease),
orbitary pseudotumor and neoplastic lesions like rhabdomyosarcoma in children and lymphoma in adult patients.
Metastatic and infectious compromise are always in the differential diagnosis.
Other primary benign tumors can affect the orbital muscles,
included in the very unusual conditions are spindle cell tumor or glomus (also known as glomangioma) which can arise in the orbits like any other hamartomatous lesion and have the same imaging findings of the typical peripheral glomangioma (figure 10).
Myositis may have multiple causes and facial Herpes Zoster can be an unusual one (figure 11).
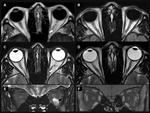
Intraconal Space
The intraconal space is located inside the inner fascial liner of the muscular cone.
It is composed mainly of fat that supports the traveling cranial nerves: optic nerve,
both superior and inferior divisions of the oculomotor nerve,
the nasociliary ramus of the trigemini and the abducens.(figure 12).
Optic nerve and ophthalmic artery as well as the superior and inferior ophthalmic veins are also structures included in this compartment.
The usual conditions affecting the intraconal space without including the optic nerve complex are vascular lesions such as carotid cavernous fistulas,
vascular malformations,
cavernous hemangiomas,
tumors arising from the nerves and fat like dermoids.
Less common conditions but important in endemic regions are infectious causes like cysticercosis (figure 13).
Other unusual finding is the presence of dilated veins due to multiple causes (figure 14),
dynamic imaging is key to diagnosis in the right clinical scenario as it is shown in (figure 15).
Optic Nerve Complex
The optic nerve is divided into 4 portions: intraocular,
which is the shortest,
intraorbital,
intracanalicular and intracranial.
Intraorbital portion has a sinuous course inside the orbit.
Because it is a CNS extension,
the optic nerve has a CSF and dural lining,
making any pathology that affect these three components a virtual possibility.
Both primary and secondary tumors can affect the optic nerve.
Gliomas account the majority of the primary tumors.
Meningiomas are less frequent and even more so the optic nerve sheath meningiomas which have been reported to be less than 5% of all orbital tumors.
(figure 16).
Secondary tumors are more common than primary lesions and usually are due to extension from primary eye tumors like retinoblastoma and choroid melanoma.
Inflammatory compromise is almost always related to optic nerve neuritis,
which is associated with multiple sclerosis. Other conditions affecting the dura and the subarachnoid space have to be kept in mind.
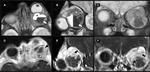
Ocular Globe
The eye occupies around 20% of the orbital volume.
The majority of the pathologies are seen in ophthalmologic evaluation.
But sometimes incidental findings and probable compromise and extension of orbital diseases requires dedicated imaging.
Tumoral conditions represent the majority of abnormal imaging findings and are divided by age groups,
with retinoblastoma being the most common tumor in the pediatric population and the uveal tract melanoma in the adult population (figure 17).
Less common tumoral entities are the metastatic lesions and lymphoma.
Intraocular infections,
specially in the right clinical scenarios,
and sequels from traumatic injuries have always a spot in the differentials list (figure 18).
Multi-compartmental
Sometimes,
pathologic conditions affecting the orbital components are aggressive with extension to the adjacent intra and extra orbital tissues.
Those lesions with vast location within the orbital cavity can be classified as multi-compartmental.
Orbital pseudotumor,
complicated infections arising from the paranasal sinuses and lymphoma are two good examples of relatively common conditions that affect more than one compartment.
Both (figure 8) and (figure 19) are illustrative examples of the involvement several compartments.