Aims and objectives
GIH is an emergency situation requiring a fast and timely diagnosis.
We review the current literature and report our experience in the GIH diagnosis and interventional management.
Methods and materials
74 consecutive patients with GIH (mean age 67.8y),
from April 2011-September 2017),
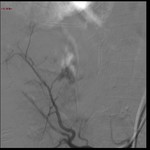
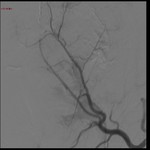
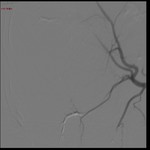
underwent to multiphasic CTA and-or DSA for imaging the site-size of bleeding,
arterial/venous origin,
and visceral complications.
The treatment was intra-arterial trans-catheter embolization,
using coils,
glue or others embolic agents.
Patient’s age,
sex,
aetiology of bleeding,
on-set time of symptom,
hemoglobin at presentation and rate of occlusion and ischemic complications were recorded and correlated using a multiple logistic regression analysis.
Results
46 CTA were performed for upper GIH (28 positive for active bleeding,
18 negative) and 28 for lower GI hemorrhage (17 positive for active bleeding,
11 negative); 30/46 (65.21%) of the uGIH patients and 21/28 (75.00%) for lGIH were successfully treated in DSA with good clinical recovery; 39.13% (18/46) of patients with upper GI bleed and 39.28% (11/28) of patients with lower GI bleed who had an initial negative CTA,
did not rebleed without the need for radiological or surgical intervention.
This difference was not...
Conclusion
CTA is mandatory for assess the vascular state in order to detect arterial abnormalities or luminal extravasation of contrast.
Failure of the endoscopy and persistent instability warrant angiography for minimally invasive and superselective embolisation.
Failure of embolisation warrants surgical intervention.
Personal information
Edoardo G.
Puglielli
Chief of Interventional and Vascular Radiology,
"G.
Mazzini" Hospital,
Teramo,
Italy
ASL TERAMO
Tel.
+39.0861.429.929 - 514
Fax: +39.0861.429.309
References
Zahid A(1),
Young CJ(2).
Making decisions using radiology in lower GI hemorrhage.Int J Surg.
2016 Jul;31:100-3.
doi: 10.1016/j.ijsu.2016.05.043.
Epub 2016 May 24.
Moss AJ(1),
Tuffaha H(2),
Malik A(3).
Lower GI bleeding: a review of current management,
controversies and advances.
Int J Colorectal Dis.
2016 Feb;31(2):175-88.
doi: 10.1007/s00384-015-2400-x.
Epub 2015 Oct 10.
Gerson LB(1),
Fidler JL(2),
Cave DR(3),
Leighton JA(4).
ACG Clinical Guideline: Diagnosis and Management of Small Bowel Bleeding.
Am J Gastroenterol.
2015 ep;110(9):1265-87; quiz 1288.
doi: 10.1038/ajg.2015.246.
Epub 2015 Aug 25.
Baker SR(1),
Shah...