Preoperative imaging identified 20 liver metastases in 9 patients ,15 hydatid cysts in 9 patients ,3 choloangiocarcinomas ,3 bile duct injuries and one hepatocellular carcinoma.
The medium delay between the last preoperative imaging and the operation was 11 days.
Lesion detection
Compared with preoperative imaging,
three additional liver metastases (15%) were detected in two patients intraoperatively.
One of these metastases was superficial and could only be detected by inspection.
The two others were detected by IOUS.
IOUS also detected a nodule associated with HCC in cirrhotic liver that turned out to be a nodular regenerative hyperplasia in histopathological analysis.
In one patient with intrahepatic cholangiocarcinoma,
two additional lesions were detected by inspection: a retroperitonal nodule and a superficial hepatic nodule.
In this case,
the discordance can be explained by the long delay between preoperative imaging and IOUS.
Staging and vascular anatomy
IOUS was found to play a primary role in tumor staging.
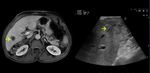
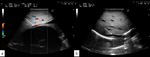
In our study the association with main vascular and biliary structures was more accurately assessed in 12 cases (48%) (Figure 3 and 4).
Moreover,
IOUS provides a real-time imaging of the liver which is a valuable tool to ensure vascular permeability before,
during and after hepatic resection.
In our study,
this was especially helpful in patients with hydatid cysts compressing hepatic or portal veins.
Compared with hepatic malignancies,
hydatid cysts cause much more vascular distortion either by compression,
destruction or displacement.
After evacuating the cysts' content,
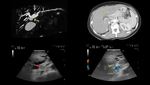
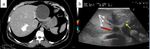
the assessment of vascular permeability was easier leading to a better choice of the radical treatment to be performed: perikystectomy or hepatectomy (Figure 5,
6 and 7).
Surgical strategy and resection guidance
Surgical plans changed owing to IOUS findings in 10 cases (40%).
These changes were motivated by additional lesions in one case,
vascular proximity or invasion in 8 cases and biliary invasion in one case.
In all cases IOUS was a valuable tool to resection guidance by helping surgeons to define surgical planes.
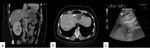
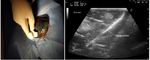
One of the methods used to demarcate the resection area in our study was methylene injection into the portal branch feeding the segments to be resected after its puncture under IOUS guidance (Figure 8).
In patients with malignant hepatic tumors,
post-operative ultrasound was helpful to ensure negative margin resection (Figure 9).