Molecular basis of RCC treatment
VHL is a tumour suppressor gene identified in familiar studies of VHL syndrome.
This group is identified in >90% of VHL mutations in spontaneous clear cell RCCs.
VHL is an E3 ubiquitin ligase that regulates a number of pro-angiogenic factors for degradation,
including vascular endothelial growth factor (VEGF).
Mutations that cause loss or silencing of VHL result in activation of these pro-angiogenic factors.
Identification of these mechanisms has led to the development of multiple VEGFR inhibitors that are now approved for use in mRCC such as sorafenib,
sunitinib,
pazopanib,
axitinib,
cabozantinib,
and levantinib.
mTOR is a potent regulator of PI3K–AKT signalling that has also been associated with RCC and promotes several processes including stimulation of angiogenesis through increase of VEGF production.
mTOR inhibitors that have been approved are temsirolimus and everolimus.
Immune checkpoint receptors are negative immune regulators that limit proliferation and activity of T cells and other immune cells.
PD-1 is a transmembrane protein expressed on activated effector T cells.
PD-1 has two known ligands,
PD-L1 and PD-L2,
which can be expressed on antigen presenting cells,
tumor cells,
and T cells.
PD-1 inhibits the signaling pathways that normally lead to an effective T cell response.
Nivolumab is the only PD-1 inhibitor currently approved in mRCC.
Response assessment
RECIST 1.0 and the revised RECIST (RECIST 1.1) are the most commonly used response assessment methods utilized for metastatic RCC.
These use a 30% decrease and 20% increase in the sum long-axis diameter of target lesions to define partial response and progressive disease,
respectively.
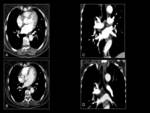
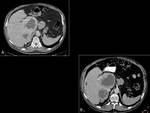
Fig. 3 However,
with TAT the tumors often remain stables for a prolonged time even in patients in whom there is no significant tumor shrinkage.
Besides,
in patients being treated with antiangiogenic agents,
the changes in tumor vascular density have been shown to correlate with treatment response and treatment resistance.
Sometimes metastatic lesions grow in size simulate disease progression by simple size measurements; however,
this is the result of intratumoral edema or necrosis induced by the antiangiogenic therapy.
In order to obtain an accurate response assessment with targeted therapies,
several morphologic tumor response criteria have been created,
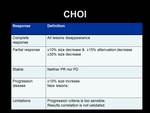
such as Choi and revised Choi criteria.
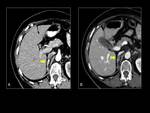
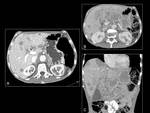
With latter,
partial response is defined as a decrease in size more than 10% and a decrease in attenuation more than 15% or a decrease in size more than 30%,
while progressive disease is defined as an increase in size more than 10 %.
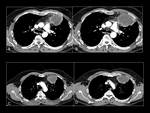
Fig. 4
Another criteria is the morphology,
attenuation,
size,
and structure,
or MASS criteria.
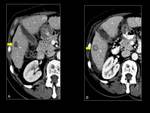
Here partial response is defined by a decrease in size >20%,
decrease in attenuation >40 HU or central necrosis >50% of solid enhancing lesion.
On the other hand,
progressive disease is defined by increase in size more than 20% without central necrosis or decreased attenuation.
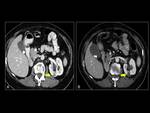
Fig. 5 Fig. 6
These morphologic criteria,
which combine the changes in size and attenuation,
attempt to overcome some of the limitations of the purely size-based RECIST criteria,
and in multiple studies have been correlated better with overall survival or with progression free survival.
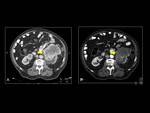
Fig. 7 Fig. 8Fig. 9 Fig. 10 Fig. 11
Sometimes,
in patients whom clinical response is clear,
there is an increase in size and attenuation of the lesions as a result of intratumoral hemorrhage when the tumor is starved of its blood supply.
Fig. 12 In such a case,
neither size- nor attenuation-based assessment would help; however,
fluid-fluid level within the lesion is a helpful indicator of intratumoral hemorrhage.
When intratumoral hemorrhage is suspected,
MRI can be performed to demonstrate the high signal intensity on T1- weighted images.
Sometimes waxing and waning size of the lesions can be observed due to recurrent hemorrhage within the lesions.
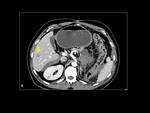
Another atypical response pattern is appearance of new lesions Fig. 13 .
This happens when the metastatic lesions are initially undetectable because they are isodense to the surrounding parenchyma and become newly visible with antiangiogenic treatment as a result of decreased attenuation with response.
Changes in the tumor margin with treatment from nodular to sharp and smooth borders is a sign of response; when present,
this sign is useful in image interpretation.
Moreover,
immune checkpoint blockers produce initial increase in tumor or appearance of new lesions followed by response and decrease in size.
Fig. 14
Thus,
knowledge of the ongoing treatment with TAT and the mechanism of action can help to the radiologists detect these atypical patterns and avoid pitfalls in response assessment.
Fig. 15
When an atypical response pattern is suspected,
is important to be aware to changes in lesions in other sites and correlate it with the clinical performance status.
When doubt persists,
a short-interval CT study after 6–8 weeks can be obtained,
which would typically demonstrate a decrease in tumor burden.
Hyperprogressive disease
Although anti PD-1 and anti PD-L1 monotherapy can lead to intense and durable tumour responses,
some studies have shown that a subset of patients appears to experience a tumor flare under these agents.
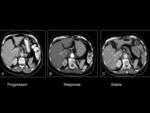
In one study,
9 % of patients were identified as experiencing hyperprogressive disease (HPD) (defined as a ≥two-fold increase of tumor growth rate (TGR) in patients with disease progression) Fig. 16 .
However,
the frequency might be higher.
The age of presentation is higher in patients with HPD vs.
non HPD.
This pattern had been observed with other therapeutic agents.
Also,
rapid progression at treatment discontinuation after long-term response under VEGFR or EGFR TKI has been reported.
Therefore,
early tumor assessment with TGR evaluation might help to decide between HPD and progressive disease from stable diasease or partial response in this subset of patients.
Toxicities Associated with TAT
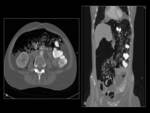
Antiangiogenics are associated with complications including bowel perforation,
tumor-bowel fistula,
hypertension,
hemorrhage,
and arterial thrombosis.
Abdominal complications have been associated with VEGF-targeted tyrosine kinase inhibitors,
possibly due to necrosis of serosal tumor implants,
and impaired healing leading to microperforations.
Continued treatment or rechallenge with the same drug can cause worsening or recurrence of pneumatosis and/or perforation Fig. 17.
Hypertension is not uncommon and may represent a potential biomarker of longer survival.
Hemorrhage is another known complication of VEGF-targeted therapy,
reported in up to 30% of patients with various cancers,
severe in less than 5% of patients.
Arterial thromboembolic events is also increased in antiangiogenic treatments.
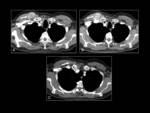
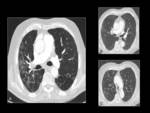
Pneumonitis is present up to 30% of the patients with RCC using mTOR inhibitors.
Pneumonitis commonly occurs during the first 6 months of therapy as bibasilar,
peripheral,
reticular,
and ground-glass opacities,
less commonly as consolidation,
in a cryptogenic organizing pneumonia pattern,
a nonspecific interstitial pneumonia pattern,
or a combination of the two.
Patients can be managed effectively without therapy cessation.
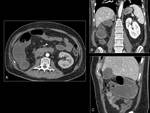
mTOR-associated enteritis is a less common.
Fig. 18
Immune checkpoint inhibitors,
can potentiate autoimmune phenomena.
These are well described in anti-CTLA-4 antibody,
ipilimumab,
treatment of metastatic melanoma,
occurring in up to 31%of patients.
One of the most commonly cited toxicities in this treatment setting is colitis Fig. 19. Sarcoid-like reaction and pneumonitis also occur,
though less frequently.
With antiPD-1 antibodies such as nivolumab,
autoimmune pneumonitis is a potentially lethal complication.
This can manifest as ground-glass and reticular opacities in a peripheral and basilar distribution or may mimic an adult respiratory distress syndrome pattern.