Disease localization
To understand the anatomic landscape is very important to localize the lesion.
If the prevertebral muscles are lifted off the vertebral body,
then the lesion is in the prevertebral space.
In contrast,
if the lesion pushes the prevertebral muscles posteriorly to the vertebral body,
it is in the RPS.
The posterior cervical space is placed posterolateral to the paraspinal space.
The posterior cervical fat separates the two spaces and serves as an anatomic landmark to help in disease localization.
Lesions contained within the paraspinal space bow the cervical fat away from the spine and displace the posterior cervical space outward,
whereas lesions in the posterior cervical space push the fat toward the central structures and cause mass effect on the paraspinal musculature.
Differential diagnosis
Diseases arising from perivertebral space may be divided according to the tissue affected.
| Infection/Inflammation |
Tumor |
| |
|
| Discitis/osteomyelitis (spondylodiscitis) |
Metastasic disease |
| Postoperative infection |
Multiple myeloma |
| Lemierre syndrome |
Chordoma |
|
Longus colli tendinitis
|
Aneurysmal bone cyst |
| |
Giant cell tumor |
| |
Schwannoma |
| Vascular |
Neurofibroma |
| |
Malignant nerve sheath tumor |
| Atherosclerotis disease |
Fibroma |
| Dissection |
Lipoma |
| Hematoma |
Chondrosarcoma |
| Vascular malformation |
|
| Hemangioma |
|
| Venolymphatic malformation |
|
| |
|
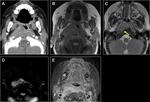
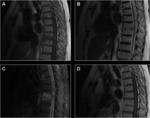
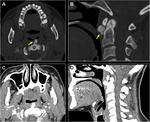
Chordoma
Chordoma is a locally destructive osseous lesion arising from midline.
Sacrococcygeal and sphenooccipital locations are more common.
C2 vertebral body is most affected when spine is involved.
T2/STIR hyperintensity is typical with variable enhancement pattern.
Fig. 3
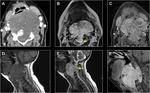
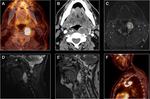
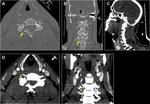
Head and neck squamous cell carcinomas
Nasopharyngeal,
oropharyngeal and hypopharyngeal carcinoma may infiltrate PVS.
They are associated with Human Papilloma Virus and smoking.
They may show T2/STIR hyperintensity and heterogeneous avid enhancement post-contrast.
Fig. 4 Fig. 5
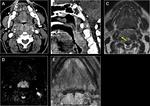
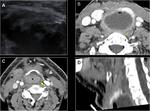
Abscess
Abscess arising in this space typically are due to discitis,
osteomyelitis or dissemination of adjacent infection.
Hyperintensity in T2/STIR with rim enhancement post contrast is characteristic of this pathology.
Fig. 6 Fig. 7
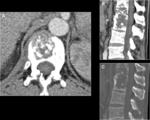
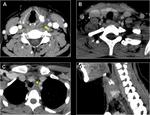
Metastases
Metastases are the most common disease in PVS.
Sclerotic osseous lesions are commonly seen in metastatic prostate,
bladder,
and carcinoid tumours,
whereas lytic metastases are observed with renal and thyroid carcinoma.
Typically spare disc spaces.
Fig. 8
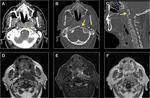
Spondylodiscitis
Spondylodiscitis affects the diabetic patient and intravenous drug abusers.
Destructive endplate changes are depict well in CT.
T1 hypointensity,
T2/STIR hyperintensity,
and patchy enhancement in vertebral endplates is typical.
When it is caused by tuberculosis is called Pott disease.
Fig. 9 Fig. 10 Fig. 11
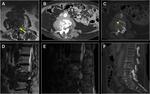
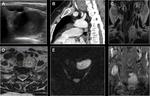
Schwannoma
15 % are extradural and 15 % are intradural and extradural with dumbbell shape.
They typically expand the neural foramen.
They may show cystic changes and rarely calcifications in CT.
Most of them are T1 isointense/hypointense and T2 hyperintense.
Enhancement is uniform.
Malignant degeneration is rare,
may produce heterogeneous enhancement and is associated with NF-1 disease.
Fig. 12 Fig. 13
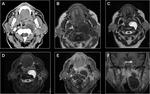
Lymphoma
Waldeyer ring is the most common site affected by lymphoma in the neck.
When it involves the nasopharynx may infiltrate PVS space.
Nasopharyngeal lymphoma is usually homogeneous,
with relatively well-defined contours and mild enhancement.
Bone destruction is less frequent than squamous carcinoma.
Lymphadenopathy is frequent.
Fig. 14
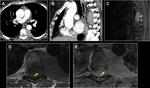
Calcific tendinitis of the longus colli muscle
Patients may present with debilitating symptoms that are unrelated to the degree of calcification seen on CT.
Amorphous calcifications are typically seen in the superior fibres of the longus colli muscle tendons at the C1-C2 level. Fig. 15
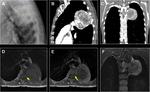
Dissection
Vertebral artery dissection is a common injury in the setting of blunt trauma.
The V3 segment is the most affected.
CTA can show subtle vessel irregularity and areas of tapering.
On MRI,
the intraluminal hematoma of dissection shows crescentic T1 and T2 hyperintense and a narrowed flow-void of the parent vessel.
Fig. 16