Aims and objectives
This work demonstrates the potential of the MARIA® (Micrima Ltd,
Bristol UK) [1][2] - a non-ionising,
non-compressing whole-breast scanning system utilising radio-waves - to automatically determine the density of breast tissue.
Density can be used as a risk indicator since dense breasts are thought to be more likely to develop cancer [3].
This information can also be used to estimate patient-specificdielectric properties,
which can improve the performance of breast radio-wave imaging.
Dielectric properties determine the propagation and absorption of radio-waves through a medium.
The MARIA®...
Methods and materials
Clinical:
Patients attending symptomatic clinics at three sites were identified by clinicians as having a palpable lump.
Following informed consent,
eligible patients underwent a MARIA® scan.
The bilateral reconstructed 3D images were used in this study.
The density classification process was accessed by comparison with BIRAD density scores estimated from mammograms.
Equipment:
MARIA® is a CE-marked radio-frequency (RF) medical imaging system [1][2] comprising a patient bed,
a Scanning and Data Processing (SDP) unit which is located under the bed and a touch-screen console featuring a...
Results
The methodology has been tested using clinical bilateral data from 57 patients with known tissue properties (25 with lucent tissue and 32 with dense tissue),
leading to a population of 114 breast scans,
64/50 symptomatic/non-symptomatic.
Symptomatic here includes breasts with an inclusion e.g.
cyst,
cancer.
It was found important to account for breast size,
results demonstrated here are all from a single measurement cup size of approximate volume of 460 ml.
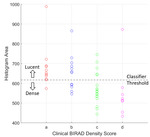
Fig.
5 shows the classifier applied to the non-symptomatic cases.
In total 76% of...
Conclusion
The results presented are a proof-of-concept demonstrating how radio-wave imaging can be used to discriminate breast density.
It has been shown that on a limited data set of 50 non-symptomatic breasts the method is able to discriminate between lucent and dense breasts with an accuracy of 76%.
Future work includes improving the methodology in the presence of lesions and study the influence of other factors (e.g.
age,
pre/post-menopausal) in the classification process.
Personal information
Dr Ana Iriarte,
Micrima Limited,
One Glass Wharf,
Bristol,
BS2 0EL
[email protected]
Gemma de Vargas,
San Pablo CEU University,
Madrid,
Spain
[email protected]
Prof Chris Bore,
Micrima Limited,
One Glass Wharf,
Bristol,
BS2 0EL
[email protected]
Dr Peter Bannister,
Micrima Limited,
One Glass Wharf,
Bristol,
BS2 0EL
[email protected]
Dr Louis Tsui,
Micrima Limited,
One Glass Wharf,
Bristol,
BS2 0EL
[email protected]
Dr David Gibbins Micrima Limited,
One Glass Wharf,
Bristol,
BS2 0EL
[email protected]
References
1.
Preece AW,
Craddock I,
Shere M,
Jones,
L,
Winton HL,
"MARIA M4: clincial evaluation of a prototype ultrawideband radar scanner for breast cancer detection." Journal of Medical Imaging,
3(3),
033502 (2016).
2.
Leendertz JA,
Preece AW,
Nilavalan R,
Craddock IJ,
Benjamin R,
"A liquid phantom medium for microwave breast imaging," 6th Int.
Congress of the European Bioelectromagnetics Association (EBEA),
Budapest,
Hungary (2003).
3.
Boyd NF,
Martin LJ,
Yaffe MJ,
Minkin S,
"Mammographic density and breast cancer risk: current understanding and future prospects,"Breast Cancer Research,...