TABLE OF CONTENTS
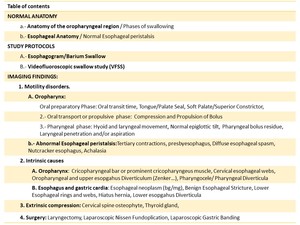
Table 1: Table of contents
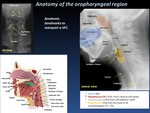
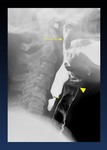
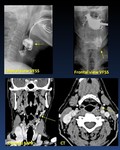
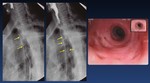
a.- Anatomy of the oropharyngeal region ( Fig. 1 )
The anatomy of mouth,
larynx,
and pharynx should be understood to evaluate the physiology of swallowing.
Pharynx extends from the nasal cavity to the UES at the crycopharyngeus muscle.
It is composed of inner circular and outer longitudinal layers of striated muscle.
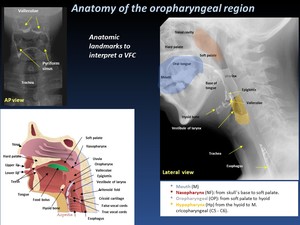
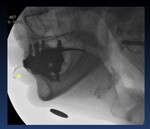
Fig. 1: Anatomy of the oropharyngeal region
In addition,
understanding the mechanism of swallowing is essential to understand swallowing disorders.
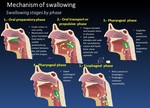
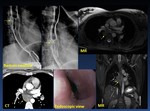
Phases of swallowing. ( Fig. 2 and Fig. 3 )
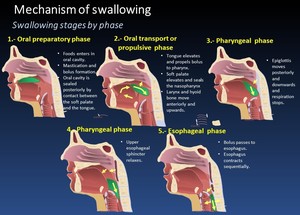
Fig. 2: Mechanism of swallowing
Fig. 3: Videofluoroscopy Swallow Study (VFSS)
b.- Esophageal Anatomy
Fibromuscular tube about 25 cm long extending from level C6 to T10.
It starts at lower border of cricoid cartilage,
courses through the posterior mediastinum and ends at the gastroesophageal junction.
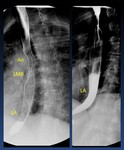
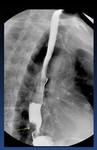
There are three physiological esophageal constrictions: aortic arch,
left mainstem bronchus and left atrium ( Fig. 4 ).
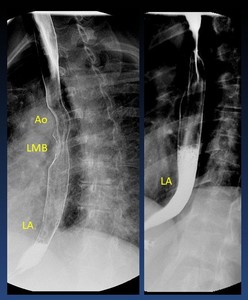
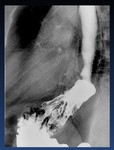
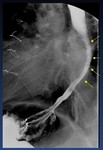
Fig. 4: Oblique view of a normal barium swallow shows the normal impressions made by the (Ao) aortic arch, (LMB) left mainstem bronchus, and (LA) left atrium on the esophagus.
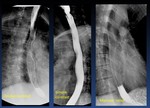
Normal Esophageal peristalsis ( Fig. 5 )
· Primary contraction: Propels bolus through the esophagus
· Secondary contraction: Follows primary contraction and propels any remaining bolus from thoracic esophagus
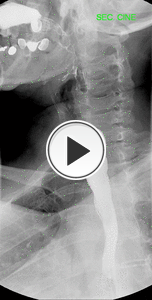
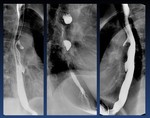
Fig. 5: Normal Esophageal peristalsis
A.- Esophagogram/Barium Swallow
Patient Preparation: NPO for a minimum of 6 hours
Contrast Material: “Thin” and “Thick” Barium (or Water Soluble contrast).
“Fizzies” allow to create “double contrast” to evaluate the mucosa.
“Fizzies” are not employed in children and post-operative patients .
The esophagus can be studied with simple contrast,
double contrast or mucous relief ( Fig. 6 )
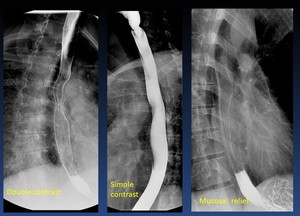
Fig. 6: Barium swalow: doublé, contrast, simple contrast and mucosal relief
1.
First explain the patient what you are going to do.
2.
Begin with the adult in the standing position facing you.
If our patient is post-operative or frail he will not be able to stand.
In that case the study can be performed in the supine or reverse Trendelenburg position.
3.
Fluoroscopy the chest and remove any artifacts – such as clips and leads from the patient.
4.
If fizzies are employed, administer them to the patient at this point and instruct the patient not to “burp”.
The gas is what gives us the contrast for mucosal evaluation.
5.
Ask the patient to take a mouthful of the “thick” barium” and watch the patient swallow.
For the first swallow you do not have to obtain any images,
this is for you to understand the patient’s motility and ability to perform the study.
6.
Then position the patient in the LPO position standing and ask to swallow a mouthful of barium (3 swallows for your 3 shots).
a.
Shoot the proximal (cervical) esophagus.
b.
Shoot the mid thoracic esophagus.
c.
Shoot the distal thoracic esophagus.
7.
We will then lie the patient down on the table and place him in the right lateral position and obtain lateral pictures of the esophagus (obtain a column of barium in the esophagus).
a.
Center first over the upper thoracic esophagus.
b.
Include a shot of the open lower esophageal sphincter (LES) on the last two views that you take
8.
Afterwards evaluate for reflux.
a.
Place the patient in the RPO position,
this will allow the contrast to pool into the cardia of the stomach.
If you observe the patient refluxing,
it is important to note three things:
1.
The maneuver that elicited the reflux.
2.
How far patient refluxed (cervical,
upper,
mid,
distal thoracic esophagus).
3.
Time it takes for the esophagus to clear the reflux.
B Videofluoroscopic swallow study (VFSS) ( Fig. 3 )
Dynamic X ray examination of oral cavity,
pharynx and cervical esophagus used to assess swallowing function by giving the patients liquids and solids of different consistencies and assessing swallowing fluoroscopically.
It is considered the gold standard for diagnosis and management of oropharyngeal dysphagia.
Videofluoroscopy swallow study is unable to detect:
• Gastroesophageal reflux.
• Aspiration unrelated to swallowing: e.g.
of saliva during sleep.
• Relationship between pharyngeal and esophageal events (although an
esophageal sweep may be included for screening purposes).
Study protocol:
Oral contrast agents.
-Contrast type.
Either barium or nonionic water soluble contrast.
- Contrast preparation.
Contrast may be prepared in different concentrations,
and/or mixed with thickening agents to simulate different liquid and food consistencies.
- Image recording.
Fluoroscopic images are recorded in real-time by high definition digital video recording equipment.
(30 frames per second fps),
Patient preparation prior to study.
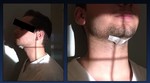
A radiopaque disk or coin is secured to the patient's chin at hyoids level ( Fig. 7 ) with tape to allow for later calibration during the on screen calculation of objective fluoroscopic swallow measures.
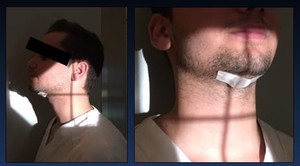
Fig. 7: Patient preparation prior to study. A radiopaque disk or coin is secured to the
patient's chin at hyoids level.
Patient positioning.
- All patients should ideally be examined in both the lateral and frontal positions.
- The visualization field includes the lips anteriorly,
nasal cavity superiorly,
cervical spinal column posteriorly,
and the entire pharyngoesophageal segment inferiorly.
( Fig. 8 )
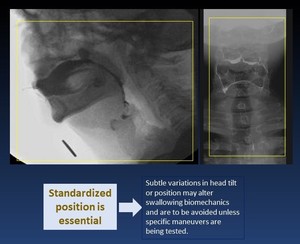
Fig. 8: The boundaries of the fluoroscopy field in the lateral view are the lips anteriorly,
nasopharynx superiorly, cervical spine posteriorly, and cervical esophagus inferiorly.
The boundaries of the fluoroscopy field in the anterior-posterior (AP) view are the
walls of the pharynx laterally, the nasopharynx superiorly, and the cervical esophagus
inferiorly.
Bolus administration.
Small or large bolus volumes,
consistencies (liquid to semisolid) are administered Fig. 9

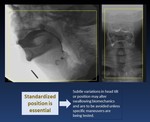
Fig. 9: The consistencies of the contrast material and the volumes administered have not been standardized across most clinics.
Different therapeutic strategies can be tested during the TVSS examination.
A.
Oropharynx:
1.- Oral preparatory Phase:
Abnormal oral phase: Weakness of the lip seal results in drooling ( Fig. 10 )
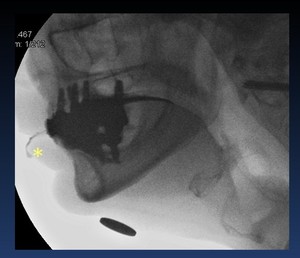
Fig. 10: Video capture of a lateral view VFSS. Weakness of the lip seal results in drooling
Oral transit time: The importance of this parameter is due to its impact on the total duration of a meal. Consequence may be an unfavorable nutritional prognosis.
( Fig. 11 )
Fig. 11: Video VFSS, solid bolus (biscuit): Increase Oral Preparatory Phase and Oral Transit Phase (>17 S).
Tongue/Palate Seal:
Incompetence of the seal between the tongue and the palate results in premature leakage from the mouth into the pharynx before initiation of swallowing,
with the potential for aspiration into the open,
unprotected larynx ( Fig. 12 )
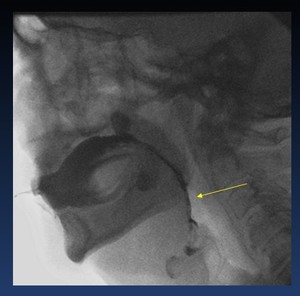
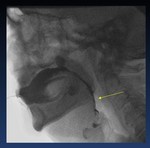
Fig. 12: Videocapture VFSS.- Premature spillage of liquid during the oral phase (arrows
Soft Palate/Superior Constrictor:
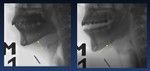
Abnormal palate/constrictor seal Weakness of the soft palate or superior constrictor muscle can result in nasopharyngeal regurgitation ( Fig. 13 )
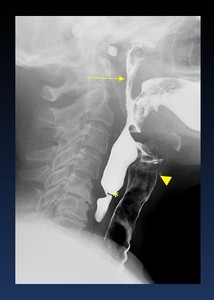
Fig. 13: Nasal regurgitation (arrow) of liquid bolus into nasopharynx caused by impaired velopharyngeal closure.
Aspiration of barium entering the trachea (arrowheads).
Stricture at Killian mouth (*)
2.- Oral transport or propulsive phase:
Compression and Propulsion of Bolus
Bolus is propelled and compressed by a combination of pharyngeal contraction and tongue base retraction.
Tongue base retraction should be completely backward to appose the converging pharyngeal wall.( Fig. 14 )
Fig. 14: woman 57 yo, with oculopharyngeal dystrophy. In all the sequences adequate laryngeal elevation that maintains during all the swallows (fractionated swallowing x5-6) and conserved posterior seal.
Lack of base contact of tongue with posterior oropharynx wall.
Important oral residue that produces a fractional swallowing.
Severe pharyngeal penetration.
Severe residue in vallecula in all the sequences that it is not able to clean and moderate residue in hypopharynx and pyriform sinus
3.- Pharyngeal phase
Hyoid and laryngeal movement
As the bolus enters the pharynx,
the hyoid begins to elevate,
moving upward and forward,
apposing to the angle of the mandible.
Descent to the resting position occurs in a one-step fashion simultaneously with the upward tilting of the epiglottis to its resting position.
( Fig. 15 )( Fig. 16 )
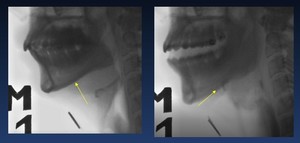
Fig. 15: VFS Honey 15 cc.- Normal Hyoid movement
Fig. 16: Abnormal hyoid motion
The hyoid may elevate incompletely or move not at all. It may elevate momentarily and not be sustained.
Normal epiglottic tilt
Epiglottic tilt is a two-step movement in most people.
The initial movement,
to the horizontal position is passive and related to hyoid elevation and tongue thrust.
The second movement,
to the completely inverted position,
is active,
probably the result of contraction of the thyroepiglottic muscle.
Pharyngeal bolus residue.
In patients with dysphagia,
pharyngeal bolus residue is a significant predictor of postswallow aspiration
Residue is due to incomplete bolus clearance with poor propulsion,
weak pharyngeal vigor,
and/or impaired UES relaxation
The BRS scored for postswallow residue:
Table 2 and Fig. 17
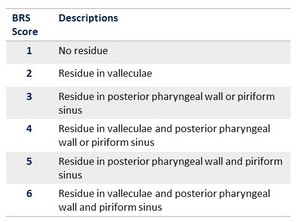
Table 2: Residuo score
Fig. 17: Bolus honey 15 cc- Residue in valleculae and posterior pharyngeal wall and piriform sinus. No penetration or aspiration
Laryngeal penetration and/or aspiration (Fig. 18 and Table 2 )
Laryngeal penetration and/or aspiration are the primary consequences of impaired closure of the glottis.
• Laryngeal penetration refers to the presence of barium contrast in the laryngeal vestibule that does not pass below the level of the true vocal folds into the trachea.
• Aspiration refers to the presence of barium contrast below the level of the true vocal folds in the subglottis or trachea.
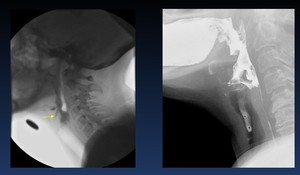
Fig. 18: A.- Video capture of a lateral view of a laryngeal penetration (arrow) without aspiration, the contrast remains above the true vocal folds
b.- Gross aspiration of barium entering the trachea

Table 3: A penetration aspiration scale
b.- Abnormal Esophageal peristalsis:
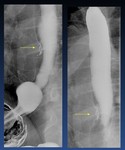
Tertiary contractions,
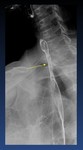
presbyesophagus ( Fig. 19 ) : Nonpropulsive contractions.
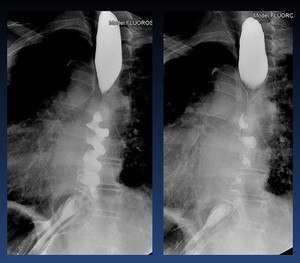
Fig. 19: Tertiary contractions, presbyesophagus
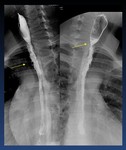
Diffuse esophageal spasm ( Fig. 19 Fig. 20 ) . Diffuse esophageal spasm produces intermittent contractions of the mid and distal esophageal smooth muscle,
associated with chest symptoms.
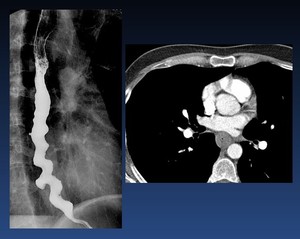
Fig. 20: Diffuse esophageal spasm
Manometry shows simultaneous nonpropulsive contractions on at least 10% of swallows.
Diagnosis is based on imaging,
manometry,
and symptoms.
Nutcracker esophagus. It is a non-cardiac cause of chest pain attributed to high amplitude distal esophageal peristalsis.
This is a controversial diagnosis that is made by manometry and does not have imaging manifestations
Decreased peristalsis resulting from achalasia,
scleroderma,
dermatomyositis,
polymyositis,
esophagitis,
and secondary to many other diseases
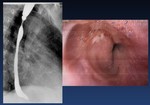
Achalasia ( Fig. 21 )
A motility disorder of the distal esophagus,
of unknown etiology.
The irreversible destruction of esophageal myenteric plexus neurons causes aperistalsis (Absent primary peristaltic waves) and the failure of lower esophageal sphincter to relax during deglutition.
Esophagram:
- Dilation with absent peristalsis
- Smooth tapering at esophageal hiatus
- Distal carcinoma may simulate achalasia (pseudoachalasia)
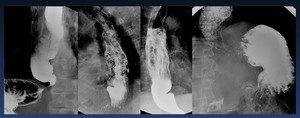
Fig. 21: Achalasia. Dilation with absent peristalsis and Smooth tapering at esophageal hiatus
A.
Oropharynx:
1.- Cricopharyngeal bar or prominent cricopharyngeus muscle ( Fig. 22 ):
The cricopharyngeal bar is a smooth,
posterior bar- or band-like protrusion into the lumen and the barium column,
seen on the lateral view,
at the junction of the hypopharynx and cervical esophagus,
at about the level of C5–C6
Cricopharyngeal bar may be seen in 5–10% of asymptomatic patients
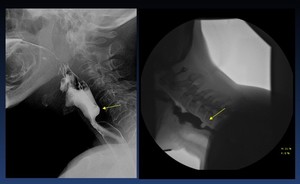
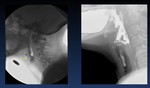
Fig. 22: Lateral view and Video capture of a lateral view of a cricopharyngeal bar (prominent cricopharyngeal muscle) arrows without aspiration
2.- Cervical esophageal webs ( Fig. 23 )
Cervical webs represent thin mucosal folds,
congenital or acquired,
frequently located along the anterior wall of the lower hypopharynx and proximal cervical esophagus.
Symptoms appear if more than 50% lumen is compromised.
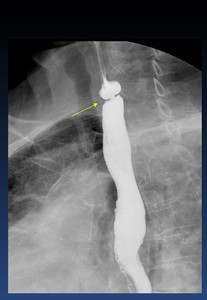
Fig. 23: Cervical esophageal web (arrow)
Sideropenic dysphagia (Plummer-Vinson syndrome): Iron deficiency anemia,
Esophageal web with dysphagia,
Increased incidence of carcinoma.
3.- Oropharyngeal and upper esopgahus Diverticulum
Several types of diverticula may be visible,
either on oropharyngeal or upper GI barium studies, including pharyngeal diverticula and pouches,
Zenker’s Diverticulum and Killian-Jamieson Diverticulum
Zencker´s diverticulum ( Fig. 24 ): mucosal outpouching of the hypopharyngeal wall located in Killian’s triangle between the upper fibers of the cricopharyngeus and inferior pharyngeal constrictor muscles.
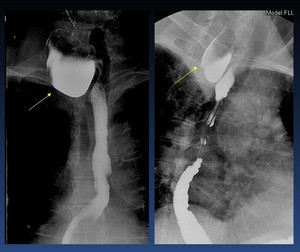
Fig. 24: Zencker´s diverticulum (arrows)
Killian-Jamieson diverticulum is a pulsion diverticulum,
protruding through a lateral anatomic weak site of the cervical esophagus below the cricopharyngeus muscle,
unlike the posterior,
midline origin of a Zenker's diverticulum.
Pharyngocele/ Pharyngeal Diverticula ( Fig. 25 )
Pharyngocele is a pharyngeal diverticulum formed by hernial protrusion of the mucosa,
through a weakness of the hypopharynx.
Usually asymptomatic but may cause dysphagia and regurgitation.
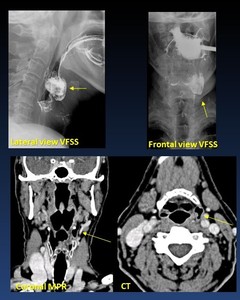
Fig. 25: Pharyngocele/ Pharyngeal Diverticula. 67 yo woman with dysphagia. Left outpouching of the lateral pharyngeal wall (arrows)
B.
Esophagus and gastric cardia:
1.- Esophageal neoplasm.-
Benign tumors
Benign esophageal tumors are rare lesions ( 1% of esophageal neoplasms) Nearly two thirds of them are leiomyomas ( Fig. 26 ); the rest are mostly polyps and cysts.
The clinical presentation depends on tumor size:
•Small tumours (<5 cm): usually no symptoms.
•Large tumours: dysphagia,
regurgitation,
oesophageal obstruction,
chest pain,
cough,
or bleeding (rare).
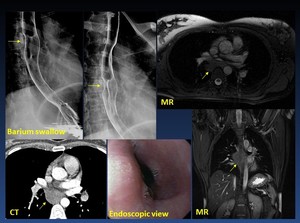
Fig. 26: Esophageal Leiomyoma
Hyperplastic polyps ( Fig. 27 ):
Hyperplastic polyps are uncommon lesions characterized by hyperplastic epithelium (foveolar-type,
squamous,
or both) with variable amounts of inflamed stroma.
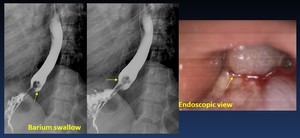
Fig. 27: Esophageal Hyperplastic Polyp
Malignant neoplasms:
Different malignancies may appear:
- Squamous carcinoma
- Adenocarcinoma
- Spindle cell carcinoma
- Leiomyosarcoma
- Lymphoma
- Metastases
An early esophageal carcinoma may be impossible to detect on a single contrast esophagram,
but an air-contrast esophagram may help in visualization by showing a surface irregularity ( Fig. 28 ).
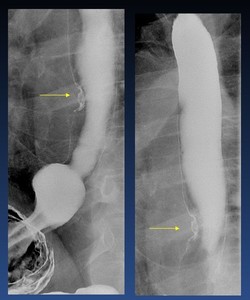
Fig. 28: early esophageal carcinoma
Advanced carcinoma may present with different gross appearances ( Fig. 29 Fig. 30 ):
- Polypoid
- Varicoid
- Infiltrative
- Ulcerative
- Superficial spreading
- Stricture
- Pseudoachalasia
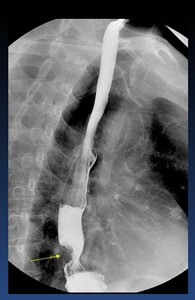
Fig. 29: Distal esophagus Carcinoma
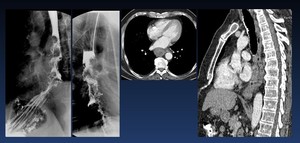
Fig. 30: Squamous cell carcinoma
2.- Benign Esophageal Stricture
Narrowing or tightening of the esophagus,
occuring when stomach acids damage the lining of the esophagus over time,
causing inflammation (esophagitis) and scarring.
The most common cause is gastroesophageal reflux disease (GERD) ( Fig. 31 Fig. 32 Fig. 33 ).
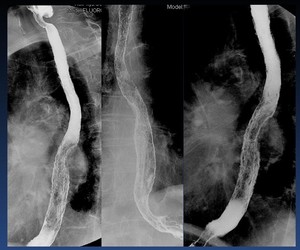
Fig. 31: Gastroesophageal reflux disease (GERD) with esophagitis and Barret,s esophagus
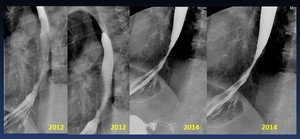
Fig. 32: Peptic esophageal stenosis. Foloww up
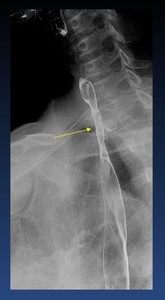
Fig. 33: Benign caustic stenosis (arrow)
Other causes of benign esophageal stricture include:
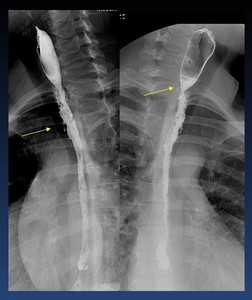
Fig. 34: Upper stricture (arrow) following caustic ingestion and esophagitis
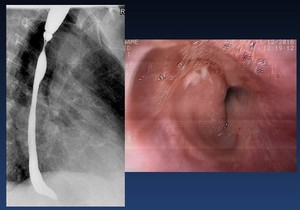
Fig. 35: Eosinophilic esophagitis. Stricture
3.- Lower Esophageal rings and webs
Patients with esophageal rings or webs are usually asymptomatic.
Symptomatic patients present with intermittent dysphagia to solids.
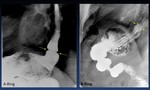
Types of lower esophageal rings ( Fig. 36 ):
A-Ring.- Muscular contraction at the junction of tubular and vestibular esophagus.
No definite anatomic correlate appears.
B-Ring.- Mucosal ring at anatomic squamocolumnar junction (Z-line).
Best or only seen with vestibular distension.
They may cause episodic dysphagia if esophagus is narrowed,
then termed a Schatzki ring (> 20 mm wide: no obstruction,
13-20 mm wide: obstruction may appear).
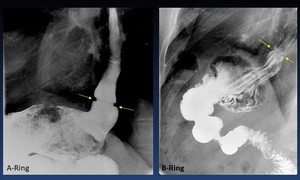
Fig. 36: Lower esophageal rings
4.- Hiatus hernia
Hernia in which abdominal organs (typically the stomach) slip through the diaphragm into the mediastinum.This may result in gastroesophageal reflux disease (GERD). Symptoms may include disphagia and chest pain.
Complications may include iron deficiency anemia,
volvulus,
or bowel obstruction.
Types ( Fig. 37 Fig. 38 ):
a.-Sliding:
- GE junction > 2cm above hiatus
- >95% of all hernias
b.- Paraesophageal:
- Gastric fundus protrudes through hiatus
- GE junction remains below diaphragm
- <5% of all hernias
c.- Mixed:
- Gastric fundus herniates beside distal esophagus
- GE junction is also above the diaphragm
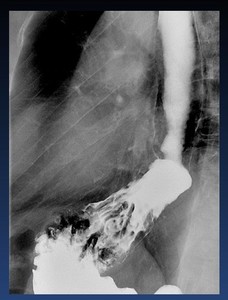
Fig. 37: Sliding hernia
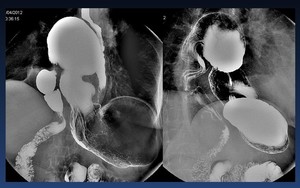
Fig. 38: Paraesophageal hernia
5.- Lower esopgahus Diverticula ( Fig. 39 Fig. 40 )
Pulsion diverticula are due to increased intraluminal pressure.
Types:
- Epiphrenic
- Midesophagus
- Aortopulmonary recess
Traction diverticula are secondary to adjacent disease.
Most located in mid-esophagus.
Epiphrenic diverticulum
These pulsion diverticula are classified by their location near the diaphragm.
If they are large they can narrow the esophagus or lead to aspiration.
Aortopulmonary window diverticulum
The normal esophagus transiently protrudes into the aortopulmonary window.
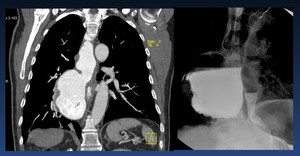
Fig. 39: Giant esophageal diverticulum
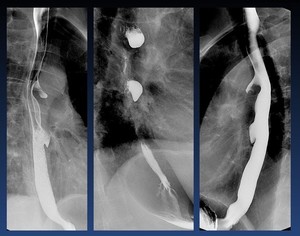
Fig. 40: Esophageal diverticula
Esophageal intramural pseudodiverticulosis ( Fig. 41 )
Rare benign disease characterized by multiple tiny flask-shaped outpouching lesions of the esophageal wall.
Pathologic findings include dilatation of excretory ducts of submucosal glands.
The predominant symptom is dysphagia,
and esophageal stricture occurs frequently.
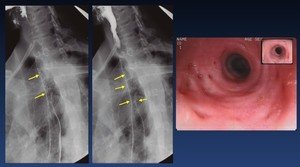
Fig. 41: Esophageal intramural pseudodiverticulosis
| 3.
Extrinsic compression: |
Cervical spine osteophyte( Fig. 42 )
Large syndesmophyte/osteophyte in diffuse idiopathic skeletal hyperostosis (DISH),
or degenerative disc diseases can cause dysphagia.
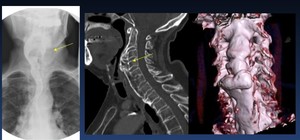
Fig. 42: Cervical osteophyte C3-C4 narrowing the esophageal lumen (arrow)
VFS.- Frontal view showing anterior osteophytes in the region of C 3, C 5 causing narrowing of the hypopharynx and retention in left pyriform sinus.
Thyroid gland.
– ( Fig. 43 )
Cervical goiter enlargement over time may extend into the thoracic space,
causing dysphagia.
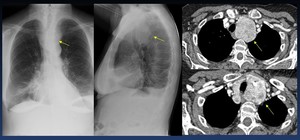
Fig. 43: intrathoracic goiter
Other causes:
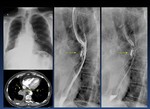
Left atrial dilatation ( Fig. 44 ),
lung cancer ( Fig. 45 )
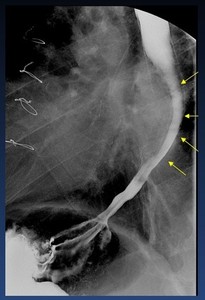
Fig. 44: Dysphagia secondary to left atrial dilatation (arrows)
A 84-year-old female patient with left atrial dilatation, presenting with dysphagia and weight loss
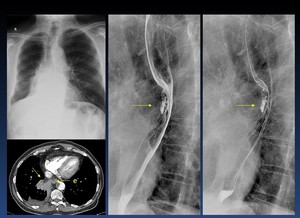
Fig. 45: Compression and esophageal ulceration caused by lung cancer
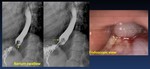
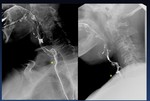
Laryngectomy ( Fig. 46 )
Dysphagia after total laryngectomy is a real and common problem that is underreported.
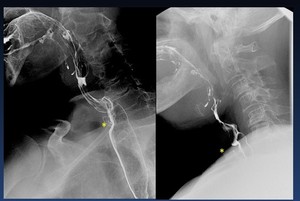
Fig. 46: 67-yo man total laryngectomy with implantation of a phonatory prosthesis (*) with clinical dysphagia.
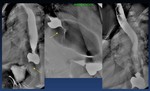
Laparoscopic Nissen Fundoplication ( Fig. 47 )
Laparoscopic Nissen fundoplication is now considered the standard surgical approach for treatment of severe gastroesophageal reflux disease (GERD)
A number of recognized complications are associated with fundoplication surgery; these include dysphagia,
gasbloat syndrome,
abnormal gastric motility,
gastric hypersensitivity,
and return of GERD symptoms.
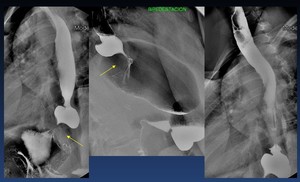
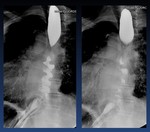
Fig. 47: Laparoscopic nissen Fundoplication (arrows). Difficulty in esophageal emptying and dysphagia. Note the esophageal dilation.
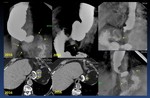
Laparoscopic Gastric Banding ( Fig. 48 )
Adjustable gastric banding (also known as “Lap Band” or “Realize band”) is considered by many to be the least invasive surgery for weight loss,
this procedure falls under the subcategory of restrictive bariatric surgery.
The procedure involves placing an implant,
a soft silicone ring with an expandable balloon in the centre,
around the top part of the stomach.
It effectively creates a two-compartment stomach,
with a much smaller top part above the band.
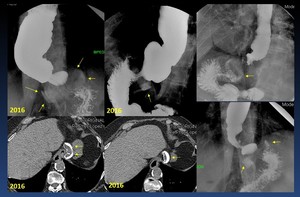
Fig. 48: 2016.- Gastric band too tight with secondary dilatation of esophagus and slow gastric emptying. 2017 The band is deflated. post treatment control