Pregnancy and puerperium are associated with an increased risk of thromboembolic events.
About 20% of these events are arterial,
and the other 80% are venous.
2
Venous thromboembolism
1.Deep venous Thrombosis and thrombophlebitis
Approximately 60–80% of venous thromboembolism cases that occur during pregnancy and puerperium correspond to deep venous thrombosis (DVT).2 One third of pregnancy-related DVT and half of pregnancy-related pulmonary emboli occur after delivery.3
It most commonly occurs in the lower limbs and represents a risk factor for pulmonary embolism.
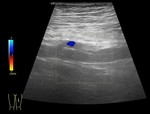
There is left-sided predominance on proximal thrombosis,
which is thought to be attributable to a relative stenosis of the left common iliac vein between the lumbar vertebral body and the right common iliac artery (Figure 1).3
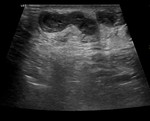
There is also an increased risk of thrombosis and phlebitis of the lower extremities superficial veins,
which is generally a benign,
self-limited disorder (Figure 2).
2. Pulmonary embolism
The rate of pulmonary embolism has been found to be the highest during the postpartum period and represents a leading cause of maternal death in the developed world.
Evaluation of pregnant and postpartum women with suspected pulmonary embolism is a controversial topic.
The D-dimer test is not reliable to exclude or stratify the risk of pulmonary embolism during this period,
since D-dimer levels may be increased even in the absence of thrombosis.
Nevertheless,
it has a high negative predictive value.
4
Doppler ultrasound plays an important role in the diagnosis of lower limb deep vein thrombosis.
Once it is confirmed,
with the appropriated clinical background,
anti-coagulant therapy may be started,
without the need to proceed to the use of ventilation–perfusion (V/Q) scintigraphy or Pulmonary CT angiography.
Additional imaging examinations are recommended when lower extremity Doppler ultrasonography fails to detect DVT,
despite clinical suspicion of pulmonary embolism.
1-3
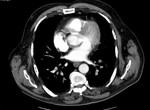
On CT angiography thrombosis can be identified as a low-attenuation filling defect of the pulmonary arteries,
that may be enlarged (Figure 3).
On V/Q scintigraphy,
classically there is a perfusion defect,
with ventilation–perfusion mismatch.3
3.
Ovarian vein thrombosis
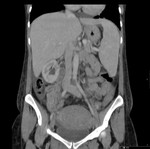
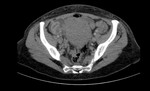
Ovarian vein thrombosis is a rare postpartum complication,
occurring in 1:2000 deliveries.5 Clinical findings are nonspecific and include abdominal pain in lower quadrants,
fever and leukocytosis,
which may mimic acute appendicitis,
pelvic infection,
ovarian torsion,
tuboovarian abscess,
hematoma of the broad ligament,
and pyelonephritis.
In 90% of cases it is located in the right flank,
possibly due to compression of the right ovarian vein against the sacral promontory by an enlarged dextroverted uterus and presence of retrograde flow in the left ovarian vein.6
Ultrasonography with colour and power Doppler study of pelvic veins is the primary imaging modality used for the diagnosis.
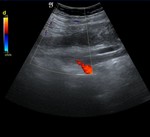
In most cases it reveals a hypoechoic tubular structure extending superiorly from the adnexa,
lateral to the IVC or aorta in the retroperitoneum,
with no color-flow filling and spectral waveform (Figure 4).
This study’s sensitivity and specificity of color is relatively low due to overlying bowel gas,
which is a limitation for sonographic visualization.
Contrast enhanced CT (CECT) venography was reported as the most sensitive imaging modality and it classically show a filling defect within the vein,
which is enlarged.
Thickening blood vessel wall and surrounding inflammatory changes may also be seen.
Unenhanced CT can demonstrate the thrombus,
that has increased or similar attenuation relative to the wall of the vein.
It is also a used to exclude other differential diagnosis of acute abdominal pain (Figure 5 and 6).2
The severity of the disease is related to the proximal extension of the thrombosis into the inferior vena cava and the risk of pulmonary embolism,
which develops in 13% of cases,
with a 4% mortality.7
Septic pelvic thrombophlebitis is a possible complication of an ovarian vein thrombosis,
with a documented incidence of 0.3:1000 deliveries.
It occurs more commonly after a cesarean section.
Typical symptoms include a spiking fever without severe abdominal pain,
or sepsis.6;7
It is important for radiologists to consider ovarian vein thrombosis’s diagnosis in patients with acute abdomen in the postpartum,
since it may prevent unnecessary surgical treatment.
4.
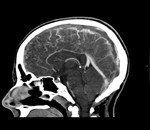
Cerebral venous sinus thrombosis
Thrombosis of a dural sinus or cerebral vein is a rare but important cause of neurological symptoms in the postpartum period,
including headache,
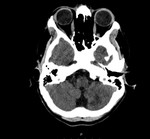
altered mental status or seizure.8 In case of the onset of neurological symptoms in the postpartum period,
CT or MR venography should be considered.
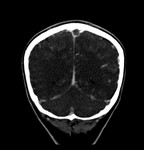
Unenhanced CT scan has low sensitivity for the detection of venous sinus thrombosis,
but it may demonstrate parenchymal abnormalities,
such has edema and hemorrhage,
which,
during this period,
should rise the possibility of this diagnosis (Figure 7 and 8).1;8
Cerebral angiography is usually reserved for cases in which a neurointerventional procedure is used to remove a thrombus that is causing rapid neurologic decline.10
When compared to other patients with dural sinus thrombosis,
this patients tend to have better prognosis after appropriate treatment.1;8
Amniotic liquid embolism
Amniotic fluid embolism is a rare,
but highly fatal complication of labor,
with an 80% maternal mortality rate.9 It is the leading cause of mortality during labor and the first few hours after delivery.10
Amniotic fluid embolism is caused by the entrance of amniotic fluid into the bloodstream through small tears in the uterine veins,
during labor.
In some cases,
it may occur after placental disruption by surgery or trauma.2;9
Classic clinical presentation is dyspnea,
cyanosis,
and shock that are abrupt in onset and usually progress rapidly to cardiopulmonary collapse.
Chest radiographic abnormalities include bilateral pulmonary opacities,
which are nonspecific and indistinguishable from acute pulmonary edema from other causes.2; 9
Arterial thromboembolism
Compared to non pregnant women,
the risk of arterial thromboembolism (strokes and heart attacks) is increased 3- to 4-fold and rises after delivery.2
1.Ischemic stroke
Approximately 90% of maternal strokes occur at delivery or in the postpartum period (Figure 9).10 Cardio-embolism is the most commonly reported etiology.
Intracranial hemorrhage is the leading cause of death in these cases,
many of which are associated with preeclampsia or eclampsia.