This study has been approved by the research ethics committee of our hospital.
Patient population
In this retrospective matched case-control study we revised the Thoracic Radiology Department database.
This database is updated every time there is an interventional chest procedure recording the procedure and its most relevant characteristics,
including whether serum was used or not when extracting the coaxial needle.
This technique was used for the first time in 2013 by one of the thoracic radiologists and from then on by other two radiologists,
based on their own criteria.
Eventually the technique became widespread.
A case and control design was carried out for this research.
The cases were recruited consecutively from the most recent procedure to the least recent of all those who underwent CT-guided lung biopsy between 2013 and 2017.
In order to homogenize the sample and make the two groups similar,
we matched the sample according to the following variables: age (+/- 5 years),
presence of emphysema and number of times the pleura was crossed to perform the procedure.
The control patient was matched when all the previous variables were coincident with the same condition for the corresponding case patient.
The control patients were recruited from the same database,
consecutively from the most recent procedure to the least recent in the same time period,
when the matching variables with each case were present.
Sample size was calculated before recruiting the patients,
according to the percentage of pneumothorax reported by other author related to lung biopsy with and without the application of sealing techniques [10-11].
Our final sample was composed by 112 patients:
- 56 cases: patients who underwent CT-guided lung biopsy between 2013 and 2017 with instillation of normal saline solution (SSLB) while removing the coaxial needle.
In this group we expected a lesser number of complications.
- 56 controls: patients who underwent CT-guided lung biopsy between 2010 and 2017 with a conventional technique (CoLB),
with no instillation of normal saline solution while removing the coaxial needle).
We excluded from the study any ultrasound-guided procedures,
patients who only underwent fine needle aspiration biopsy,
patients who developed a pneumothorax during the procedure but previously to the lung biopsy,
and those patients with thoracic lesion in whom the lung would not be violated in the biopsy procedure.
Biopsy procedure
After marking the optimum puncture point on the patient skin and proper preparation with local anesthetic (9 ml mepivacain + 1 ml sodium bicarbonate) an introducer coaxial needle was inserted up to the verge of the pulmonary lesion and a core biopsy of the lesion was performed through inspiration with either an 18-gauge or 20-gauge core biopsy needle,
depending on the choice of the performing radiologist.
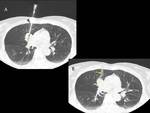
The instillation of saline solution through coaxial biopsy needle was performed after the biopsy was taken: we prepared a syringe with normal saline (5-10 ml approximately) and introduced it at the same time that we removed the coaxial needle up to the skin in order to fill the biopsy track with this inert liquid material.
The coaxial sheath was withdrawn in one swift motion (Fig. 1).
When no saline solution was instilled the coaxial sheath was withdrawn in one swift motion too.
The procedures were performed either by one of the residents radiology in training at thoracic imaging,
always under staff supervision,
or by one of the three thoracic radiologists experienced in CT-guided biopsies (9,
10 and 14 experienced years).
Patients were placed in prone,
supine or lateral decubitus positions to achieve the most direct and safe route,
depending on the location of the lesion.
All biopsies were guided by a helical Siemens CT system (Somaton Emotion).
After the procedure,
a chest located CT examination was performed to identify the presence of pneumothorax.
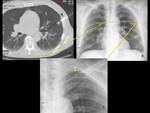
We also performed a 4 h follow-up chest X-ray (posteroanterior and lateral projections when possible) in order to identify delayed pneumothorax.
Image analysis
All cases and controls radiological images archived at our Picture Archiving and Communication System were reviewed by three resident radiologists (two at the third year of residency and the third one at the first year) using a digital reading workstation.
The reviewed images were CT images acquired during prebiopsy,
biopsy and post-biopsy processes,
and post-biopsy chest radiographs.
The following parameters were evaluated: emphysema on CT (yes/no),
emphysema along the needle path (yes/no),
maximum lesion size (mm),
needle diameter (18G and 20G),
association with fine needle aspiration biopsy (yes/no),
patient position during lung biopsy (supine,
prone,
right lateral and left lateral),
needle puncture site (anterior,
posterior and lateral wall),
lesion location (lung lobe),
lesion semiology (nodule/mass,
consolidation and mixed nodule),
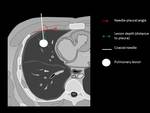
lesion depth (external margin of the lesion -pleural distance),
needle-pleural angle,
number of samples taken,
prebiopsy pneumothorax,
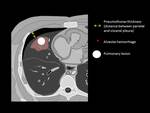
postbiopsy pneumothorax and its maximum pneumothorax thickness in CT or chest x-ray (size),
delayed pneumothorax 4h post punction on posterioranterior chest X-ray (yes/no) (Fig. 2),
pneumothorax requiring chest tube placement,
hemoptysis (yes/no),
and alveolar haemorrhage (ground glass opacity surrounding the lesion with a diameter higher than the lesion,
yes/no) (Fig. 3 and Fig. 4).
Other demographics (ie.
age) or procedure-related variables (ie.
number of passing through pleura with biopsy needle,
chest tube placement),
probably related to lung biopsy complications were also retrospectively analysed.
The anatomo-pathological report obtained from the biopsy sample was also evaluated.
Statistical analysis
We matched the cases and controls by age,
emphysema and number of passing through pleura with biopsy needle.
The Kolmogorov-Smirnov test was used to evaluate the normality distribution of the variables.
The quantitative variables are presented as means ± standard deviations (SD) and qualitative variables as absolute frequencies,
percentages and medians.
The variables of the groups studied will be analyzed with the corresponding statistical tests for each type of variable,
depending on their distribution.
In order to evaluate whether the findings were stable against the possible influence of other variables,
multiple logistic regression was performed.
For statistical analysis IBM SPSS Statistics for Windows (Armonk,
NY: IBM Corp.),
21.0.0.0 version y MedCalc for Windows,
12.7.0.0 version (MedCalc Software,
Ostend,
Belgium) were used.
P-value of less than 0.05 was considered to indicate statistically significant difference.