The entrapment and compression neuropathies are usually diagnosed on the basis of clinical history and electrophysiologic studies (electromyography and nerve conduction studies).
MRI has proved significantly useful since it allows to identify the precise location of the injury depending on the affected muscle group and has a remarkable advantage over the EMG,
which does not show signs of muscle denervation up to 2-3 weeks after injury (Linda,
D.
et al.¹)
The denervated muscles show us the possible nerve compromised and guide us to find the location of the nerve injury.
The finding of high signal intensity in T2 and STIR secuences depicting muscle edema,
represents an acute lesion.
Fatty atrophy reflects chronic denervation,
showing hiperintense signal in T1 and T2.
The muscles which usually present a denervatory pattern are: infraspinatus,
supraspinatus,
teres minor and deltoid.
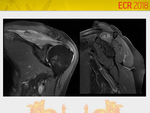
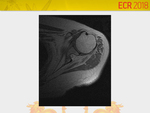
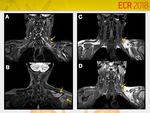
Parsonage-Turner Syndrome (Fig.
5 and 6)
Also know as acute brachial neuritis and neuralgic amyotrophy.
Etiology: Not clear.
Autoimmune mechanisms? Viral?.
Self-limited. 3rd–8th decade.
Bilateral 30%.
Characteristic manifestation:
Acute and severe shoulder pain followed by weakness.
Most common muscle involved is supraspinatus (97% of cases,
and 50% isolated according to Gaskin et al.³).
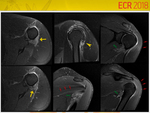
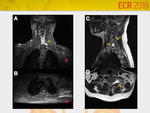
Quadrilateral Space Syndrome (Fig.
7)
Due to compression of the axillary nerve and posterior circumflex humeral artery,
resulting in tener minor and anterior and medial portions of deltoid muscle denervation.
Etiology: Traumatic and atraumatic causes
Mass lesions such as tumors, posteroinferior paralabral cysts or fibrous bands (most frequent),
posteroinferior paralabral acute lesion with edema (fig. ), osteoartritis,
etc.
Post-traumatic nerve injury may occur in almoust half of shoulder dislocations,
since the nerve is stretched over the dislocated humeral head.
Most axillary nerve injuries are secondary to brachial plexus impairment.
Isolated injury may occur in open surgical intervention with a deltoid muscle–splitting approach or reverse shoulder arthroplasty.
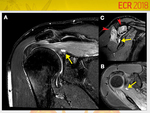
Suprascapular Nerve Entrapment
Sites of entrapment include
Suprascapular notch: supraspinatus and infraspinatus denervation (fig.
9).
Spinoglenoid notch: infraspinatus denervation.
2nd – 6th decades.
Etiology:
Compression from space-occupying lesions,
including paralabral cysts (fig.
9), tumors,
iatrogenic surgical injury,
and enlarged varicosities.
Thickened transverse scapular ligament (repetitive strain on the abducted and externally rotated shoulder),
with entrapment on the suprascapular notch.
Thoracic Outlet Syndrome
Entrapment of the brachial plexus at specific anatomic places.
Sites of entrapment include the retropectoralis minor,
costoclavicular,
and interscalene spaces (fig.
1).
Etiology: Cervical Rib; trauma (fig.
8 and 9),
fibrosis,
clavicular fracture; compresion: weight lifters,
swimmers,
tennis; tumoral: lipomas,
neurogenic tumors; Iatrogenic (Erb-Duchenne fig.
11).
Clinical presentation depends on the affected nerve,
involving more frequently axillary and supraspacular nerve.