Various breast lesions can be observed in CT images,
including inflammatory,
infectious and post procedure findings (scars,
seromas) as well as malignant lesions such as breast primary (carcinoma,
lymphoma,
sarcoma) and secondary breast or other tumors metastasis.
BREAST CT LEXICON
Accurate assessment of breast lesions requires standardized terminology to describe and categorize abnormal findings.
For mammography,
breast US,
and breast MR imaging,
the Breast Imaging Reporting and Data System lexicon of the American College of Radiology provides the framework for standardized interpretation.
Similarly,
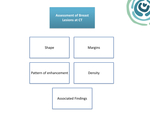
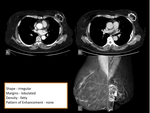
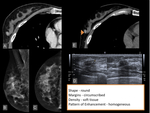
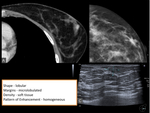
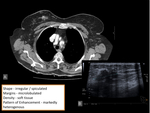
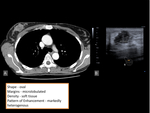
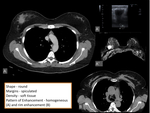
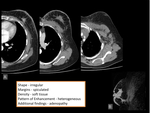
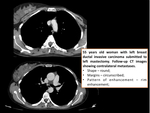
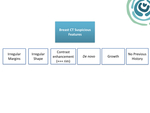
breast lesions detected with multidetetor CT should be described by using a similar lexicon (figure 1):
- Shape: round,
oval,
lobular,
irregular.
- Margins: circumscribed,
microlobulated,
obscured,
indistinct,
spiculated.
- Breast CT findings should be classified according to density in Hounsfield units and categorized as either fat,
air,
fluid,
or soft tissue.
- If contrast material was administered,
the pattern of enhancement should be further characterized if possible as homogeneous,
heterogeneous,
rim enhancing,
central enhancement,
or enhancing internal septations.
- It is important to describe associated findings,
as they will help in further characterizing a malignant or benign process.
These include edema,
skin retraction,
nipple retraction,
skin thickening,
lymphadenopathy,
chest wall or skin invasion,
presence of a hematoma or blood,
architectural distortion,
and stability of findings compared to previous CT scans.
BENIGN LESIONS
- Postoperative changes
Postoperative changes in the breast may mimic a malignancy; therefore,
it is important to obtain an accurate history as to the timing of biopsy or surgery and to follow the changes in lesion morphology over time.
Other clues to evaluate postoperative findings include patient symptoms suggesting infection,
such as fever,
and surrounding surgical changes that may include clips from biopsy or axillary dissection.
Abscess formation is uncommon in the postoperative setting.
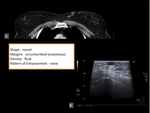
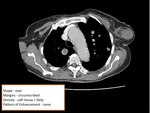
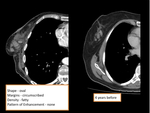
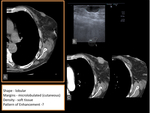
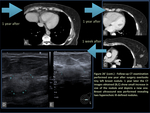
- Hematoma/Seroma (figure 2,
3)
Breast hematomas and seromas can be seen after biopsy,
trauma,
or surgery.
Their diagnosis can be made by correlating the finding to the clinical history.
Immediately after surgery or biopsy,
the surrounding edema may obscure a hematoma.
Hematomas will become smaller over time and eventually resorb and therefore can be distinguished from other masses.
An abscess may have a similar appearance at CT,
although a clinical history of a fever and an elevated white blood cell count may suggest the diagnosis.
As a hematoma resolves,
the blood- filled mass changes to serous fluid,
forming a seroma.
At CT,
seromas appear as well-defined,
relatively high-attenuation fluid collections.
There may be associated calcifications,
metallic clips,
or air-fluid levels,
along with peripheral enhancement after contrast material administration.
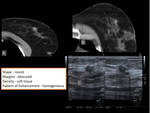
- Scars (figure 4)
As a scar develops the surrounding glandular tissue is drawn to a central dense nidus of fibrous tissue.
If the scar can be shown to occupy a surgical or biopsy site,
then the spiculated appearance is not of concern.
In differentiating a scar from cancer,
correlating prior biopsy locations from the patient history,
reviewing prior images,
and noting linear scar markers in the locations of prior biopsy are very important.
Masses not corresponding to a postbiopsy scar should be considered suspicious.
In addition,
any new tissue growth in a previously identified postoperative scar (particularly after cancer resection) should be viewed with suspicion.
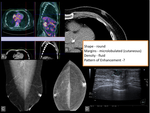
- Fat necrosis (figure 5)
Fat necrosis may result from accidental trauma,
but most cases are seen after surgery or radiation therapy.
When symptomatic,
fat necrosis typically presents as a small,
painless,
ill defined breast mass.
Fat necrosis can present as lipid cysts,
coarse calcifications,
focal asymmetries,
microcalcifications,
or spiculated masses.
The features depend on the amount of fibrosis.
2.
Benign Breast Abnormalities (figure 6,7,8)
The absence of malignant features at CT,
and familiarity with characteristics of benign masses and calcifications at mammography and benign masses at MR imaging are currently the sole bases for recognizing benign breast lesions at CT.
Note should be taken that any mass with benign features at CT requires additional validation of benignity with demonstration of long-term stability or additional diagnostic mammographic work-up with or without sonographic evaluation.
2.1 Fibroadenoma (figure 9)
Fibroadenoma is the most common benign breast tumor.
These benign lesions are most commonly found in women ranging from 15 to 40 years of age and are caused by proliferation of connective tissue within the lobule.
At CT,
fibroadenomas appear as circumscribed,
round or oval masses that may demonstrate coarse popcornlike calcifications.
Nonenhancing fibrous septations are a specific feature seen in some fibroadenomas at MR imaging; however,
this has not yet been confirmed as an imaging characteristic at CT.
2.2 Hamartoma (figure 10,
11)
Hamartoma (fibroadenolipoma) is an uncommon,
often palpable tumor that contains fat and glandular tissue and is often referred to as a “breast within a breast.” At CT,
fibroadenolipomas appear as a circumscribed,
mixed-density lesion that contains macroscopic fat.
2.3 Benign calcifications
Calcifications can appear with or without an associated lesion,
and their morphologies and distribution provide clues as to their cause.
Typically,
benign calcifications include lucent-centered calcifications,
eggshell or rim calcifications,
coarse or popcornlike calcifications,
large rodlike calcifications,
and round calcifications.
Nearly all calcifications currently seen at CT are benign,
on the basis of size alone,
due to the limited spatial resolution.
Uniform large,
round calcifications are more likely benign,
whereas fine pleomorphic calcifications smaller than 0.5 mm have a higher probability of indicating malignancy and are rarely visualized at CT.
MALIGNANT LESIONS
Irregular margins,
irregular shape,
and rim enhancement are the most highly predictive features for malignancy in the studies.
A spiculated and irregular margin is the most accurate sign for malignancy.
A washout pattern on postcontrast images has high positive predictive value and sensitivity,
although low negative predictive value and specificity.
Diffuse regional enhancement is also shown to have high positive predictive value for malignancy.
CT has the advantage of demonstrating the margin of tumor invasion without overlapping tissues,
an added advantage over mammography,
and it may allow identification of contralateral lesions.
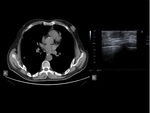
- Invasive Ductal Carcinoma (figure 12 - 16)
Invasive ductal carcinoma is the most common breast cancer,
accounting for about 80%–90% of all invasive cancers .
The cancer usually grows as an irregular mass that is firm at palpation.
At CT,
invasive ductal carcinoma appears as a dense,
spiculated mass with marked early and/or peripheral enhancement.
The presence of rim enhancement and internal enhancing septations can be suggestive signs.
In advanced cases,
associated skin thickening,
lymphadenopathy,
or pleural effusions may be seen.
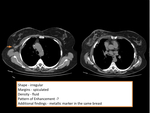
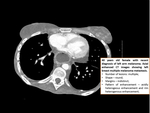
- Invasive lobular Carcinoma (figure 17)
Invasive lobular carcinoma accounts for 10%– 15% of invasive breast cancers.
It spreads through the breast parenchyma by means of diffuse infiltration,
which may cause little disruption of the underlying anatomic structures.
CT findings may be non-specific,
some cases appearing as an asymmetric soft-tissue density with or without associated skin thickening while others may manifest as a mass.
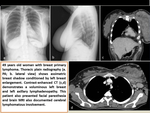
- Lymphoma of the Breast (figure 18)
Breast manifestation of lymphoma elsewhere in the body,
secondary lymphoma,
is more common than primary lymphoma,
although both are rare.
Lymphadenopathy is the most common manifestation of secondary lymphoma involving the breast,
seen on mammograms as large,
round lymph nodes in the axilla with loss of the fatty hila.
Secondary breast lymphoma is usually caused by non-Hodgkin lymphomatous infiltration of breast tissue.
It is a rare cause of an ill-defined mass that resembles invasive ductal cancer at mammography.
The borders of the mass may be indistinct due to lymphomatous infiltration into surrounding glandular tissue.
If a patient has a primary diagnosis of lymphoma elsewhere in the body and a new ill-defined breast mass,
primary breast cancer should still be the leading diagnosis; however,
secondary lymphoma should be considered as a differential possibility.
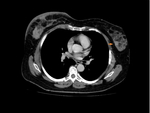
- Inflammatory Carcinoma (figure 19-20)
Inflammatory carcinoma is an uncommon,
aggressive tumor with early dermal lymphatic invasion and poor prognosis.
Clinical diagnosis is based on increased warmth,
induration of breast skin,
erysipeloid edge (peau d’orange),
and nipple retraction.
In some cases,
inflammatory carcinoma may be indistinguishable from mastitis and abscess but fails to respond to antibiotics.
Inflammatory carcinoma should be considered in the differential diagnosis when breast edema is accompanied by clinical signs of infection.
The CT appearance is aggressive with marked skin thickening,
breast edema and peripheral enhancement.
A discrete mass is often absent with inflammatory cancer.
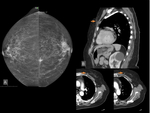
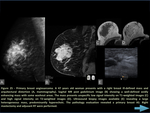
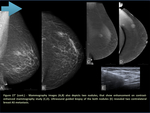
- Metastasis (figure 21-23)
Metastases to the breast from non-mammary primary tumors are uncommon and account for 0.5-2.0% of all breast malignancies.
Metastases tend to be found in the subcutaneous fat,
whereas primary breast cancers develop in glandular tissue.
They do not tend to cause retraction of the skin or nipple. Metastatic lesions are much more likely to be multiple or bilateral than primary cancers.
Like other metastasis,
metastases to the breast tend to be rounded and well defined.
They typically lack spiculation.
As opposed to breast cancer, calcification is unusual.
Microcalcifications are rare but can occur with some primary type (e.g,
psammoma bodies in ovarian cancer).
The most frequent source of a metastatic breast lesion is the contralateral breast.
Among metastatic lesions to the breast,
multicentric lymphoid malignancies and disseminated melanoma constitute the most likely sources.
Other,
less common sources are carcinomas of the lung,
ovary,
stomach,
and,
infrequently,
carcinoid tumors,
hypernephromas,
and carcinomas of the liver,
tonsil,
pleura,
pancreas,
cervix,
perineum,
endometrium,
and bladder.
In children and adolescents,
rhabdomyosarcoma is one of the common tumors reported to give rise to breast metastasis.
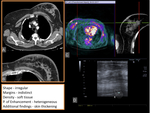
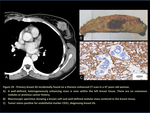
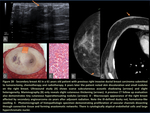
- Tumors Associated to Treatments - Angiosarcoma (figure 24 - 28)
The discovery of a breast mass in a patient known to have had previous therapy for cancer at another site may present a difficult diagnostic and therapeutic problem.
Breast angiosarcoma presents as primary tumors of the breast,
or as secondary lesions that are most commonly associated with previous radiotherapy.
Primary angiosarcoma has been observed in women age 30-50 years presenting with poorly defined masses.
It accounts for <0.04% of malignant neoplasms and typically arises in the parenchyma of the breast with occasional skin involvement.
In contrast,
secondary angiosarcoma presents in older women (median age 67-71 years) following a median of 10.5 years after radiotherapy for breast cancer.
Incidentally breast CT findings such as enhancing parenchymal or cutaneous breast nodules may raise suspicion for this entity in the proper scenario.