Muscle edema can occur from a variety of causes,
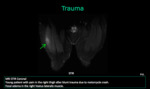
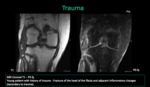
such as trauma,
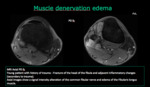
subacute denervation,
during and after muscle exercise,
early myositis ossificans,
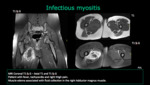
infectious myositis with abscess formation and autoimmune conditions.
Muscle contusions are caused by trauma.
The direct blow causes interstitial hemorrhage and edema,
which is evident in the MR images at the site of the injury and compromise the overlying subcutaneous tissues.
More severe cases may have hematomas and thus appears as a masslike lesion in addition to edema.
Muscle denervation in the subacute phase (2 days - 4 weeks after denervation) causes edema uniformly throughout the involved muscle.
This mechanism is poorly understood but appears likely to reflect shifting of water from intracellular to extracellular spaces.
Some denervation mechanisms are spinal cord injury,
poliomyelitis,
peripheral nerve injury or compression.
Some studies have shown edemalike signal intensity as a transient,
physiologic finding during and following vigorous exercise.
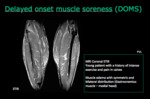
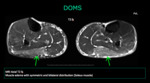
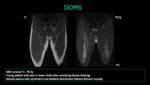
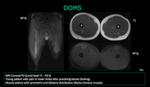
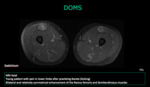
Delayed onset muscle soreness (DOMS) is a type of overuse injury that become symptomatic hours or days after the overuse episode.
Muscle edema at MRI often reveals symmetric and bilateral distribution in the involved muscles and their antagonists (flexors and extensors).
Mild DOMS is frequently seen in recreational athletes.
Severe forms may progress to rhabdomyolysis.
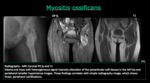
Myositis ossificans typically manifests as a soft tissue mass that develops characteristic peripheral calcification after 6–8 weeks.
This may develop spontaneously but usually results from trauma.
It may also be seen in patients with paralysis,
burns or intramuscular hematoma.
The findings at MRI correlate with what is found in radiographs.
Initially,
heterogeneous muscle edema is seen,
which progresses to a masslike lesion of high signal intensity on T2 weighted images.
It can be difficult to differentiate this lesions from a sarcoma.
Older lesions develop peripheral calcification that is best identified on radiographs and computed tomographic scans.
Recognition of the peripheral calcifications is important for making the diagnosis,
because biopsy may lead to a false diagnosis of osteosarcoma due to the abundant osteoid and mitotic cells.
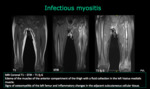
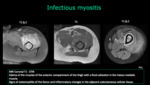
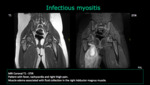
Muscle infection produce edema and it can be the only anormality.
Abscess formations or necrosis may be seen at MR images with intravenous paramagnetic contrast medium.
Bacterial myositis usually result from direct extension of infection in tissues adjacent to a muscle,
such as osteomyelitis or a subcutaneous abscess.
This entity is seen primarily in immunocompromised patients.
In immunocompetent patients,
it results from hematogenous spread,
direct trauma,
after intramuscular injection or surgery.
Staphylococcus aureus is the most common pathogen.
Autoimmune inflammatory conditions may cause muscle edema.
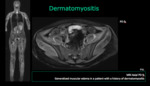
Polymyositis and dermatomyositis are caused by a cell mediated (type IV) autoimmune attack on skeletal muscle.
Clinically characterized by gradual onset of muscle weakness in the thighs and pelvic girdle that progresses to involve the upper extremities,
neck and pharyngeal musculature.
Polymyositis involves only skeletal muscle; dermatomyositis involves both skeletal muscle and skin.
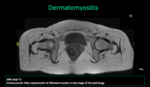
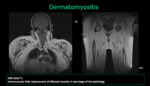
MR images show muscular edema in all muscle groups predominantly in the thighs and pelvic girdle.
In late stages of the pathologies T1-weighted images allow the identification of intramuscular fatty replacement of affected muscles.