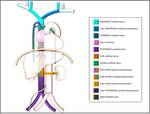
|
ANOMALIES FROM THE UPPER HALF BODY VENOUS RETURN
(SVC)
|
Isolated anomalies of the right SVC are rare,
and consist of low insertion into the right atrium,
drainage to the left atrium,
interruption,
or aneurysmal dilatation.
From the persistence of the left anterior cardinal vein results a double SVC,
and if,
in addition,
the normally persistent right cardinal vein regresses,
then there is only a left SVC. Fig. 6
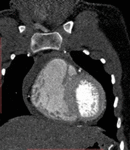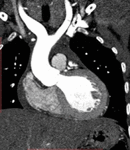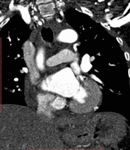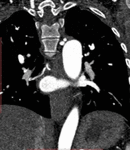
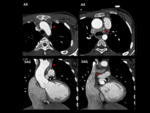
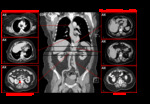
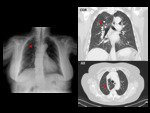
A persistent left SVC,
in most cases as a component of a duplicated SVC,
is an incidental finding in less than 0.5% of the general population,
occurring most frequently with congenital heart disease,
where the incidence can reach 4%.
In the absence of congenital heart disease,
a left SVC or left component of a duplicated SVC almost always drains into the coronary sinus,
descending lateral to the aortic arch and anterior to the hilum,
and entering the pericardium in the posterior atrioventricular groove.
On SVC duplication most frequently the left brachiocephalic vein is absent,
and the right SVC is smaller than the left.
In conventional radiography it can be identified by a focal widening of the mediastinum superior to the left side of the aortic knob,
or most commonly,
when traversed by an IV catheter. Fig. 9
Fig. 7
Fig. 8
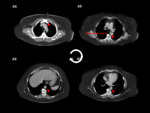
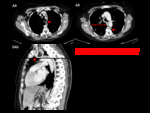
Absence of the right SVC is almost always related with a persistence of left SVC,
so total absence of SVC is a very rare anomaly,
often found with other congenital cardiac anomalies and/or conduction abnormalities.
The superior systemic veins drain into persistent azygos veins subdiaphragmatically,
with prominent collateral vessels that allow a sufficient venous return by cavo-caval anastomoses.
The patient may be asymptomatic,
but many suffer from SVC syndrome.
It also can complicate placement of IV catheters and transvenous pacemaker electrode leads.
Fig. 11
Fig. 12
- Anomalous course of the brachiocephalic veins Fig. 13
An anomalous left brachiocephalic vein rather than joining the right brachiocephalic vein ventral to the aorta,
crosses the midline dorsal to the ascending aorta to join the SVC caudal to the azygos vein.
It is usually associated with congenital heart disease.
Fig. 14
Fig. 15
|
ANOMALIES FROM THE LOWER HALF BODY VENOUS RETURN
(IVC)
|
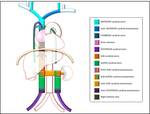
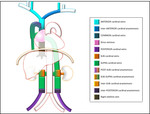
Inferior caval abnormalities are typically the result of abnormal embryologic development involving the vitelline,
posterior cardinal,
subcardinal and supracardinal veins,
yet,
even in cases of severe malformation,
one of the constituent networks invariably substitutes some form of venous flow.
Prevalence: 0.2%–3%
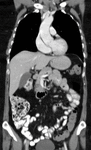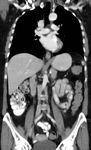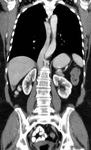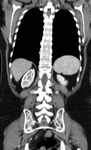
Embryology: Persistence of both supracardinal veins. Fig. 17
Anatomy: Typically the left IVC ends at the left renal vein,
which crosses anterior to the aorta in the normal fashion to join the right IVC.
However,
there may be variations in this arrangement and significant asymmetry in the sizes of the left and right veins.
Clinical relevance: Should be suspected in cases of recurrent pulmonary embolism following placement of an IVC filter.
Fig. 18
Fig. 19
Prevalence: 0.2%–0.5%
Embryology: Regression of the right supracardinal vein with persistence of the left supracardinal vein.
Anatomy: Typically,
the left IVC joins the left renal vein,
which crosses anterior to the aorta in the normal fashion,
uniting with the right renal vein to form a normal right-sided prerenal IVC.
Clinical relevance: Transjugular access to the infrarenal IVC for placement of an IVC filter may be difficult.
Fig. 21
Fig. 22
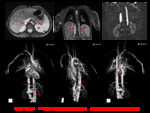
- Interruption of the infrarenal IVC with preservation of the suprarenal segment Fig. 23
Most rarely there can be an absence of the infrarenal IVC with preservation of the suprarenal segment,
resulting from abnormal embryologic development of the posterior cardinal and supracardinal veins.
Anatomy: A normal suprarenal IVC is formed by confluence of the renal veins.
The external and internal iliac veins join to form enlarged ascending lumbar veins,
which convey blood return from the lower extremities to the azygos and hemiazygos veins via anterior paravertebral collateral veins,
and thus,
blood from the caudal part of the body reaches the heart via the azygos and superior vena cava.
Clinical relevance: Patients may present with symptoms of lower-extremity venous insufficiency or idiopathic deep venous thrombosis.
- Interruption of the hepatic segment of the IVC / Azygos continuation of the IVC Fig. 24
Prevalence: 0.6%,
may reach 1.3% when concomitant congenital heart disease,
asplenia or polysplenia syndromes (left isomerism).
Embryology: Failure to form the right subcardinal–hepatic anastomosis,
with resulting atrophy of the right subcardinal vein,
causing the blood to directly shunt into the right supracardinal vein. Fig. 25
Anatomy: The renal portion of the IVC receives blood return from both kidneys and passes posterior to the diaphragmatic crura to enter the thorax as the azygos vein,
which joins the SVC at the normal location.
The azygos vein,
azygos arch,
and SVC are dilated subsequently to the increased flow.
The hepatic segment of the IVC is absent or hypoplastic,
with the hepatic veins draining into the right atrium via the suprahepatic IVC.
Clinical relevance: Preoperative knowledge may be important in planning cardiopulmonary bypass and to avoid difficulties in catheterizing the heart.
Fig. 26
Fig. 27
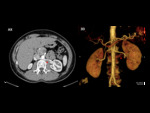
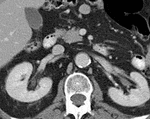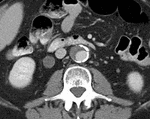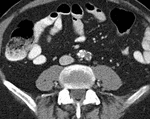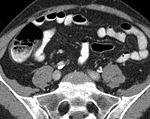
- Left Renal Vein associated anomalies
These are associated with persistence of the dorsal limb of the embryonic left renal vein and of the dorsal arch of the renal collar (intersupracardinal anastomosis) Fig. 31,
and their major clinical significance is in preoperative planning prior to nephrectomy and renal vein catheterization.
In a Circumaortic left renal vein that persistence results in the presence of two left renal veins,
one superior that receives the left adrenal vein and crosses the aorta anteriorly and one inferior that receives the left gonadal vein and crosses posterior to the aorta inferior to the normal anterior vein.
Prevalence may be as high as 8.7%.
Fig. 30
Fig. 32
In a retroaortic left renal vein that persistence is associated with regression of the ventral arch (intersubcardinal anastomosis) so that a single renal vein passes posterior to the aorta.
Prevalence is about 2%.
Fig. 28
Fig. 29
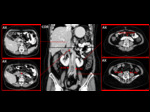
Prevalence: 0.07%
Embryology: Anomaly of the right supracardinal system with persistence of the right posterior cardinal vein positioned ventral to ureter in the definitive IVC. Fig. 34
Anatomy: The proximal ureter courses posterior to the IVC,
then emerges to the right of the aorta,
coming to lie anterior to the right iliac vessels.
Clinical relevance: Many patients are asymptomatic,
but some may develop partial right ureteral obstruction or recurrent urinary tract infections due to urinary stasis.
Fig. 35
Fig. 36
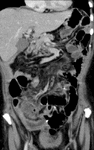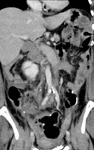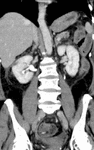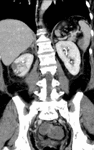
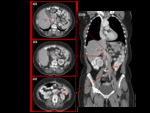
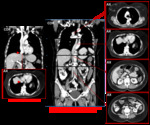
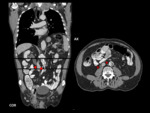
- Double IVC with retroaortic right renal vein,
interruption of the hepatic segment and hemiazygos continuation of the IVC Fig. 39
More than one anomaly can coexist in a patient,
and that is such a case.
Fig. 41
Fig. 42
|
AZYGOS-HEMIAZYGOS SYSTEM ASSOCIATED ANOMALIES
|
Variants of the azygos-hemiazygos system anatomy occur frequently,
especially the configuration of the hemiazygos and accessory hemiazygos veins,
which can form a common trunk instead of draining separately.
Variation in the azygos venous system may also be acquired,
due to collateralisation of blood flow in cases of SVC or IVC obstruction.
An anomalous course of the azygos vein in the right lung apex gives rise to an azygos lobe in approximately 0,4-1% of the population.
Its development has been attributed to the posterior cardinal vein failing to migrate over the apex of the right lung,
resulting in the abnormally located vein indenting the lung and its overlying parietal and visceral layers of pleura,
resulting in four pleural layers,
the azygos mesofissure,
similarly to a mesentery structure.
This anomaly is easily identified on imaging studies,
including conventional chest radiographs.
Fig. 44
Congenital absence of the azygos vein is rare.
Enlargement of the hemiazygos,
accessory hemiazygos,
and left superior intercostal veins is associated with it.
Fig. 46
- Azygos / hemiazygos continuation of the IVC Fig. 37
During development,
the intermediate segment of the supracardinal vein that joins the IVC and azygos-hemiazygos veins regresses,
but if the suprarenal segment of the IVC fails to develop,
it may persist,
resulting in azygos or hemiazygos continuation.
Already presented concerning the IVC.
Fig. 38
- Variable hemiazygos dreinage Fig. 47
The hemiazygos vein drains normally into the azygos vein,
but could also drain to the right SVC,
via the accessory hemiazygos vein→left superior intercostal vein→left brachiocephphalic vein,
or to a persistent left SVC.
This often occurs with duplicated IVCs and the different drainage routes will influence the imaging findings of a hemiazygos continuation of a left-sided IVC.
May result in a rarer hemiazygos lobe.
The azygos vein may also rarely drain into the right brachiocephalic vein,
right subclavian vein,
intrapericardial SVC or directly into the right atrium.
Fig. 48